
Lessons Learned From a Community-Based Health Care Project
In 1970, life in dry and dusty Jamkhed, India, was hard. Many villagers suffered from cholera, malaria, and other infectious diseases, and 40 percent of children under 5 were malnourished. Virtually no women used family planning or had any prenatal care. Serious pregnancy-related complications were common, and maternal death rates were high.
Thirty-seven years later, the picture has changed dramatically. Less than 5 percent of young children are malnourished, and chronic and infectious diseases are far less common. Prenatal care is nearly universal, maternal death rates have plunged, and use of family planning is on par with that of developed countries.
Much of the improvement is credited to the work of the Comprehensive Rural Health Project (CRHP), the vision of two Indian doctors trying to improve the lives of the rural poor. The community-based health program that began in a handful of villages in 1970 now concentrates on 130 villages in western Maharashtra state.
Project Emphasizes Community Participation, Not a Top-Down Approach
The project, based in Jamkhed about 250 miles east of Mumbai, uses a holistic approach that integrates preventive and primary health care, good environmental practices, and socioeconomic development to attack the problems that cause disease and ill health and improve the quality of life of the poor and marginalized. Fundamental to CRHP’s approach is raising the status of women and breaking down caste barriers.
“We are trying to empower people to take health into their own hands,” says Dr. Shobha Arole, the project’s associate director, whose parents founded the project. Enabling people to take responsibility for their health and well being, she says, “is more powerful than telling people what they should do.”
Community participation is essential because local people must “feel it’s their project,” she says. Rather than trying to impose changes, CRHP works with villagers, many of whom are illiterate, to educate them about basic health care. “You make people think through things,” Arole says, “so they understand why you’re doing what you’re doing.”
Building Trust and Emphasizing Preventive Health
When Drs. Mabelle and Rajanikant Arole first visited the Jamkhed area, they found that most health problems stemmed from malnutrition, lack of clean water, poor sanitation, and chronic infections. Doctors were scarce. Medical facilities were costly and far away. They also saw that the low status of women and caste-based discrimination contributed to poor individual and community health.
The Aroles estimated that 80 percent of the health problems could be prevented or managed with relatively simple measures, but they also learned early that their work could begin only after they gained the trust of local people. Though they had intended to integrate curative and preventive health care at the start, they acceded to local wishes for a hospital. With financial support from local businessmen and traders, the Aroles began by fashioning a rudimentary medical center out of a former veterinary dispensary and nearby buildings.
They also began running weekly health clinics in the villages, and helped villagers drill wells to provide stable sources of clean water that would improve sanitation and reduce water-borne infections. Project staff taught villagers to dig simple drainage systems to improve sanitation and eliminate standing water where mosquitoes breed. When drought and famine struck the area in 1972, the project helped farmers improve agricultural methods and produce more nutritious food. The Aroles made concerted efforts to ensure that improvements reached all members the community, such as by drilling village wells in sections where the lowest caste members lived.
Village health workers became the key component of their health efforts. They are women selected by their village who attend weekly training sessions. They provide basic maternal, child, and other health care, and flag problems that require a higher level of care. They also serve as health educators to demystify medicine and emphasize prevention.
A mobile team composed of a nurse, social worker, paramedic, and doctor visits the villages regularly to provide higher-level care, and a 40-bed hospital handles emergencies, surgery, and diagnostic tests.
Health Indicators Show Marked Improvement
Through village health workers, prenatal care now reaches 99 percent of women in project villages, up from less than 1 percent at the beginning of the project. Maternal death rates have fallen from around 700 maternal deaths per 100,000 live births to 70. Infant mortality has dropped from 176 infant deaths per 1,000 births to 24.
A study of 2,861 deliveries in 25 project villages between 1996 and 1999 reported just two maternal deaths, even with 85 percent of the women giving birth at home.
Use of family planning has risen from less than 1 percent of married women before the project began to 68 percent today (see Figure 1).
Figure 1
Family Planning Use Increased in the Project Area.
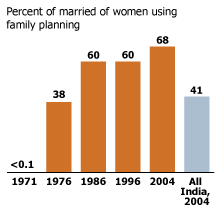
Source: Comprehensive Rural Health Project.
Women have an average of two to three children, down from about five in 1970. As a result, the crude birth rate has dropped from 40 per 1,000 people to 19 (see Figure 2).
Figure 2
Birth Rates Declined in the Project Area.
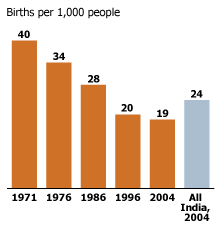
Source: Comprehensive Rural Health Project.
In addition, virtually all children are immunized against polio, diphtheria, pertussis, and tetanus compared with less than 1 percent at the start of the project, and less than 70 percent in rural Maharashtra today.
Village health workers, who get most of the credit for improving maternal health, provide regular checkups during and after pregnancy, conduct home deliveries, and teach others in the community how to deliver babies safely. Village health workers also organize and coordinate the activities of women’s clubs, farmers’ clubs and other community groups.
As crucial as they turned out to be, however, village health workers were not part of the Aroles’ original plan, which had called for trained nurse midwives to live in the villages and provide health care and education. However, because the communities did not trust outsiders, the village health workers proved to be essential.
Some of the improvement in health indicators may be due to modernization, such as the arrival of electricity and paved roads. In addition, a tradition of social conservatism in the project region strongly discourages premarital sex, so out-of-wedlock pregnancies and related sexual health issues are not a significant problem.
Key Principles: Equity, Integration, Empowerment
CRHP’s annual operating budget of about $500,000 is funded through a charitable trust; foundation and other grants; income from its training center and from products sold by a farm the project runs; and hospital fees.
Through its training institute, CRHP has trained 2,000 international health and development workers, as well as 5,000 from the government and nonprofit sectors in India.
The training emphasizes the project’s principles of equity, integration, and empowerment. Equity gives every person access to health information and services, regardless of wealth, color, caste, or creed. Integration blends preventive and curative care as well as social and economic aspects of development so all systems work together. Empowerment begins by putting knowledge in people’s hands and teaching them how to use it, a process that takes time, Dr. Arole says.
“To a certain extent, you have to have all three working at the same time in order to bring about some change,” she says. Although dramatic improvements can be seen in five years, she estimates that a commitment of 10 to 15 years is needed to bring about sustained changes in attitude and behavior.
Deborah Mesce is the manager of media programs for the Population Reference Bureau’s international programs. She recently accompanied journalists in PRB’s Women’s Edition program on a visit to Jamkhed to learn about the Comprehensive Rural Health Project.
References
Mabelle Arole and Rajanikant Arole, Jamkhed: A Comprehensive Rural Health Project (London: Macmillan Press, 1994).
Comprehensive Rural Health Project website: www.jamkhed.org.
Colin McCord et al., “Efficient and Effective Emergency Obstetric Care In a Rural Indian Community Where Most Deliveries Are At Home,” International Journal of Gynecology & Obstetrics 75, no. 3 (2001): 297-307.
