
Fewer Malaria Cases in Cambodia
Date
December 20, 2002
Author
(December 2002) According to the World Health Organization (WHO), around 300 million people worldwide suffer from malaria each year resulting in at least 1 million deaths. Malaria is endemic in 100 countries, a factor that places more than 40 percent of the world’s population at risk.1 Sixty percent of Cambodia’s landscape poses a malarial risk. One million Cambodians are infected with malaria each year. Of those infected, between 1.5 percent and 10 percent in some remote provinces, die.2 Efforts taken by Cambodia’s National Malaria Control Program (NMCP) have led to reductions of malaria outbreaks in the last decade. Between 1997 and 2001, the number of new malaria cases decreased by more than one third, from 15.05 cases per 1,000 in 1995 to 9.60 cases per 1,000 in 2001 (see Figure 1).3 Malaria remains one of the primary causes of mortality in Cambodia, however. Sustained efforts through local and national malaria control will be necessary to contain Cambodia’s malaria epidemic.
Figure 1
Malaria Incidence Rates in Cambodia, 1997-2001
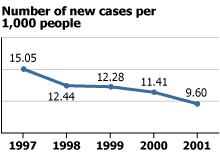
Source: National Malaria Control Program, Cambodia.
Transmission
Malaria is passed to humans by infected female mosquitoes. When the mosquito bites a person, it passes a parasite to the human bloodstream. The parasite is carried to a person’s liver and eventually multiplies. Another mosquito can then pick up the parasite by biting an infected person and can continue to spread the disease by biting another person.
Of the four human malaria strains, Plasmodium falciparum is the most common and deadly form, responsible for the vast majority of malaria death worldwide. In Cambodia, this parasite is responsible for the majority (88%) of malaria infections and deaths.4 Symptoms including fever, chills, headache, nausea, vomiting, diarrhea, and night-sweats occur 8 to 30 days after initial infection. Unlike other types of malaria, if not promptly treated Plasmodium falciparum may cause kidney failure, seizures, confusion, coma, and death. Prevention, early recognition of symptoms, and immediate treatment are key to curbing malaria-related deaths.
At-Risk Populations
Malaria-infected areas tend to be those where mosquitoes can breed and survive easily such as wooded, shady areas and places where water and moist climate are common. In Cambodia, malaria tends to be found in the forest regions bordering Thailand, as well as in the rubber plantations found in the east and northwest. Urban and coastal areas are only slightly affected. These affected areas translate into a large number of Cambodians who are at risk of contracting malaria: An estimated 15 percent of the population is at medium to high risk of malaria infection.5 The populations most affected include forest inhabitants, migrant and border workers, pregnant women, and infants and children.
Forest Inhabitants
Though the population of the hilly and forested areas of Cambodia is small, malaria prevalence there is the highest in the country, ranging from about 15 percent to 40 percent in villages near or in forested areas, to 0 percent to 3 percent in the plains and surrounding rice fields. In Rotanak Kiri, Mondol Kiri, and Stueng Treng near the borders of Laos and Vietnam, forest populations account for 25 percent of recorded cases in the country but make up only 2 percent of the population.6 In these endemic regions, people are constantly infected with malaria. Over time, however, this continued exposure becomes a protective immunity against the parasite and its infection of the bloodstream.
Migrant and Border Workers
Migrant and border workers are exposed to malaria because their jobs — collecting wood, working on rubber plantations, and laboring in gem and gold mines — often bring them from areas of no or low malaria transmission to work in endemic areas. Unlike forest inhabitants who permanently live in endemic areas, these individuals have no built-up immunity to malaria. Immigrants and new settlers form a large nonimmune risk population — approximately 2 million people each year.7 Many migrant and border workers have limited access to health care and treatment, making malaria diagnosis and treatment difficult.
Pregnant Women
Pregnant women become more susceptible to malaria after their 14th week of pregnancy when any prior immunity to malaria breaks down.8 Malaria infections during pregnancy can cause anemia and lead to an increased risk of maternal death. Malaria in pregnancy also increases the risk of miscarriage and stillbirth. Babies born to mothers with malaria often have low birth weight, which endangers the survival and healthy development of newborns. Medical personnel advocate the use of antimalarial drugs throughout a pregnancy, as well as the use of insecticide-treated mosquito nets (ITNs) as part of prevention efforts.
Infants and Children
Children under age 5 make up 71 percent of all malaria deaths worldwide.9 A child’s most vulnerable period begins at 6 months of age when the mother’s protective immunity wears off and before the child has established his or her own robust immune system. In Cambodia, 9 percent of all malaria cases occur in children under age 5.10 Malaria is often fatal as an infected child’s condition may deteriorate quickly: Children can die within 48 hours after the first symptoms appear. For those who survive, repeated bouts of malaria hamper learning through missed school days and hinder a child’s physical and cognitive development. Children with malaria can, in most cases, be quickly and effectively treated with a course of inexpensive oral tablets called Malarine. Families and communities must be trained to recognize the symptoms of malaria and to seek treatment as quickly as possible.
Prevention
Malaria can be prevented by avoiding contact with mosquitoes through the use of ITNs; eliminating mosquito breeding sites; and spraying households with insectide to repel or kill mosquitoes. In Cambodia, ITNs are an important cornerstone of government, nongovernmental organization (NGO), and donor malaria control strategies. The insecticide-impregnated nets repel mosquitoes and prevent bites that can lead to malaria. While ITN campaigns have been launched in various areas throughout Cambodia, universal coverage has yet to be achieved in high-risk areas. Increased distribution of ITNs and hammock nest targeted toward migrant populations are key to the long-term protection of vulnerable groups. Health education messages on malaria transmission tailored to communities’ social, cultural, and geographical settings and needs are also an important part of preventive measures.
Diagnosis and Treatment
As malaria can be fatal, early recognition of symptoms and immediate treatment are critical. Unfortunately, because malaria symptoms often resemble influenza or other febrile illnesses, individuals do not always seek medical advice. Thirty-two percent of rural children under 5 with malaria symptoms go without treatment or medical advice, compared to 23 percent of urban children.11
Cost and access often deter people from seeking diagnosis or treatment. Clinical diagnosis typically requires laboratory technology and skilled lab technicians to read the slides of blood under a microscope. Unfortunately, this level of technology and training is still rare in Cambodia. For this reason, a rapid diagnostic “dipstick” test has been introduced in Cambodia. This inexpensive test can be easily used in rural areas, increasing access to malaria testing.
Drug resistance complicates effective treatment of malaria in Cambodia. Cambodia has the largest number of drug-resistant forms of malaria in the world. There are many reasons for this: Mosquitoes are developing resistance to certain insecticides; environmental changes are creating new breeding sites; and people are commonly not finishing the full course of malaria medications or taking cheap, ineffective antimalarial drugs available on the market. Unlike other malaria-stricken countries, Cambodia cannot use the common malaria treatment Chloroquine, because it has strong drug resistance in northwest and southeast Cambodia. Mefloquine resistance has also been found in western provinces since 1995, but has not spread to other parts of the country. National drug policies have adapted to the changing resistance patterns, but the complexity of the situation has made implementation difficult. The recommended malaria treatment throughout much of Cambodia includes Mefloquine and Artemether.
Malaria treatment in Cambodia is further complicated by poor drug quality. In recent years, counterfeit drugs containing no active antimalarial substance have been found in private drug stores throughout the country.12 These fake drugs make it difficult to fight infection and result in increased malaria-related deaths. Government actions to produce antimalarial drugs in easy-to-identify packages and to restrict the selling of counterfeit drugs have assisted in efforts to improve drug quality. But more work is needed to ensure that individuals finish the full course of authentic malaria medications to prevent future strains of drug-resistant malaria.
Policy Implications
The technology exists to prevent, monitor, diagnose, and treat malaria. Prevention campaigns must ensure that at-risk populations have access to ITNs and information on the signs and symptoms of malaria. Testing must be encouraged once symptoms appear and should be accessible and affordable to the general population. In addition, government efforts must focus on removing counterfeit drugs from the market and ensuring that malaria medications meet their prescribed potency. Sustained efforts through local and national malaria control programs are important to contain the malaria epidemic in Cambodia.
References
- The Global Fund to Fight AIDS, Tuberculosis & Malaria, Malaria: Key Facts, accessed online at www.globalfundatm.org/journalists/
fsheets/malaria.htm, on Aug. 15, 2002. - National Malaria Center, Cambodia, “Malaria,” Vector Borne Disease Watch, accessed online at www.cnm.gov.kh/vbd.htm, on Aug. 1, 2002.
- Cambodian Ministry of Health, National Malaria Control Program (NMCP), “Malaria Situation in Cambodia: Strategies, Implementation, and Challenges, 2001,” public dissemination of NMCP data (Phnom Penh: NMCP, 2002).
- Cambodian Ministry of Health, NMCP, public dissemination of NMCP data (Phnom Penh: NMCP, 2002).
- Cambodian Ministry of Health, NMCP, public dissemination of NMCP data (Phnom Penh: NMCP, 2002).
- World Health Organization (WHO), Western Pacific Region, Malaria, Other Vectorborne and Parasitic Diseases, accessed online at www.wpro.who.int.themes_focuses/theme1/focus2/tlf2cambodia.asp, on July 29, 2002.
- European Commission (EC) Regional Malaria Control Program, MMF Issue 1, accessed online at www.mekong-malaria.org/mcis/
mmf3_27.htm, July 29, 2002. - WHO, Maternal Mortality: A Global Factbook (Geneva: WHO, 1991): 9-10
- WHO, “Protecting Children From Malaria,” Roll Back Malaria Campaign, accessed online at www.rbm.who.int/newdesign2/children/
children.htm, Aug. 1, 2002. - WHO, “Protecting Children From Malaria,” Roll Back Malaria Campaign.
- National Institute of Statistics (NIS), Directorate General for Health [Cambodia] and ORC Macro, Cambodia Demographic and Health Survey (CDHS) 2000 (Phnom Penh, Cambodia, and Calverton, Maryland: NIS Directorate General for Health and ORC Macro, 2001): 154-57.
- J. Rozendaal, D. Tith, and A. Thy, “Malaria Drug Quality in Cambodia, Summary of a Country Wide Investigation in November-December 1999,” in Malaria Control in Complex Emergencies: Cambodia, accessed online at www.lshtm.ac.uk/itd/dcvbu/malcon/Cambodia.pdf, on Aug. 1, 2002.
For More Information
Please contact the Department of Planning and Health Information, Ministry of Health, #151-153, Blvd Kampuchea Krom Ave., Phnom Penh, Cambodia
