Sandra Yin
Former Associate Editor

November 9, 2007
Former Associate Editor
How long one lives depends on gender and context, among other factors.
Gender differences in mortality and life expectancy vary by country. But in most countries, men live shorter lives than women (see figure). In Russia, for instance, the difference between male and female life expectancy is 13 years (59 vs. 72). In other countries, such as the United States, the male disadvantage is smaller: 5 years (75 vs. 80). And in some countries, such as Afghanistan, there is little or no male disadvantage (42 vs. 42).1
Life Expectancy at Birth by Sex, 2007
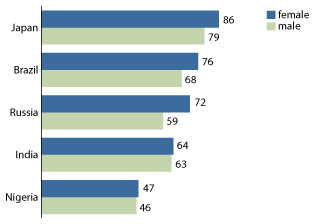
Source: C. Haub, 2007 World Population Data Sheet.
What’s behind the male/female gap in life expectancy? Factors that influence gender differences in mortality include biological factors such as hormonal influences on physiology and behavior, and environmental factors, such as cultural influences on gender differences in health behaviors.
The importance of specific factors may reflect the environmental context. How developed a country is can affect or shape the most important influences on gender differences in mortality.2
In developed countries, men’s more risky unhealthy behaviors are a major reason they die younger. Their higher rates of cigarette smoking, heavy drinking, gun use, employment in hazardous occupations, and risk taking in recreation and driving are responsible for males’ higher death rate due to lung cancer, accidents, suicide, and homicide.3
Risky male behavior may be fueled by biology and culture. Research suggests that testosterone contributes to males’ greater physical activity and aggressiveness; this “domino effect” leads to their higher death rate due to accidents and homicide. But when looking at gender disparities in health and mortality, it can be hard to get at biological differences. “You can’t tease out the societal differences from the biology,” says Ingrid Waldron, a professor of biology at the University of Pennsylvania. “They come as a package.”
Men’s risky behaviors also contribute to their having higher mortality rates in developing countries, but in developing countries the gender gap in mortality has been smaller than in developed countries. Environmental factors such as unsafe water and inadequate nutrition increase the death rate due to infectious diseases for both sexes. Women, however, face additional risks associated with childbirth. Maternal mortality is high in sub-Saharan Africa, and there are higher suicide rates for women than men in China.
Another reason the gender gap in mortality is smaller in developing countries is because in many of these countries, women have much lower social status than men. As women’s status catches up with men’s in these countries, the gender gap is expected to increase in the developing nations. But in developed countries, the gender gap is expected to decrease as women adopt unhealthy behaviors similar to men’s—drinking and smoking more, experiencing more job-related stress.
Differences in what is expected of men and women and how they are taught to behave also contribute to variation in health-related behaviors. For example, many cultures encourage or condone men’s heavy drinking, but discourage it in women. Also, in many cultures, women are not expected to work outside the home in the cash economy while men are expected to be part of the labor force.
Because women are less likely to be part of the work force than men, they suffer less from the ravages of work. As a result, their health deteriorates less quickly.4
Low-paid or manual work seems to take a toll in terms of health. People in the bottom income group tend to have both worse health and more rapidly deteriorating health while they are working. Yet, while manual workers are typically less healthy on average, the differences among male and female workers in this occupational group are much smaller than differences across occupations.5
Changes over time can affect the gap in life expectancies. In most developed countries, men’s widespread adoption of cigarette smoking during the first half of the 20th century was a major factor behind males’ widening mortality disadvantage. Later, in the United States, the mortality gap narrowed as women began to smoke more and men smoked less than before. The difference in male and female life expectancy has narrowed in recent years, from at least 7.7 years from 1972-1979 to 5.2 years in 2004, according to the U.S. National Center for Health Statistics. Changes in smoking patterns tend to affect men more than women, because more men have smoked and because smoking has elevated death rates more for men than for women.6 As smoking becomes even less common, mortality rates will probably decline further.7
While women rate their health worse than men and visit the hospital more often than men from early adolescence to late middle age, they are less likely to die at each age. This paradox can be explained at least in part by differences in the prevalence of chronic conditions men and women face.8
Women experience higher rates of pain (headache, arthritis), and some respiratory conditions, including bronchitis, asthma, and lung problems not related to cancer. They are also much more likely to suffer from reproductive cancers, hypertension, vision problems, and depression. Men are more likely to suffer from hearing loss; smoking-related ailments, such as emphysema and respiratory cancer; and circulatory problems including cardiovascular disease and diabetes.
However, women and men with the same chronic conditions have the same self-rated health. Yet men with respiratory cancer, cardiovascular disease, and bronchitis are more likely to die than women with these conditions. This implies that men may experience more severe forms of these conditions.
Researchers have found that conditions associated with excess male hospitalizations and deaths tend to be smoking-related. Indeed, men with smoking-related conditions are significantly more likely to die in two years than women with the same conditions. This may be the case, because typically, men are exposed to smoking for a longer time on average than women.9
Public campaigns have helped decrease deaths related to unhealthy behaviors, particularly those associated with male deaths. These efforts may well help narrow the male-female mortality gap in the United States. The 40-year-old antismoking campaign has led to a drop in lung cancer death rates for men. And the efforts to reduce drunk driving have been effective, Waldron notes. Pointing to public concerns about secondhand smoke and the efforts of Mothers Against Drunk Driving to alert the public of the risks of drunk driving, Waldron says that the grassroots support made it easier to push through policy change. “In this country [the United States], movements that have had big benefits had citizens’ support,” she says. “Leadership was important, but not everything.”
