
Maternal Mortality a Leading Cause of Death in Cambodia
(January 2003) Motherhood should be a time of anticipation and delight for a woman, her family, and her community. For many women, however, it is a time laden with risk and danger. In developing countries, more than half a million mothers die each year from maternal causes. For every woman who dies, about 30 suffer devastating health problems such as infertility and damage to their reproductive organs.1 In Cambodia, maternity-related complications are one of the leading causes of death among women ages 15 to 49. Motherhood can be a safer time for women when health systems address the serious and life-threatening complications of pregnancy and childbirth as they occur. This requires interventions aimed at improving the health and well-being of women at each step of motherhood: pregnancy, childbirth, and the postpartum period.
While pregnancy is a normal, healthy state for women of reproductive age in developed countries, women in developing countries risk death and disability every time they become pregnant. Complications before, during, and after childbirth can often be fatal in the developing world.
A maternal death is any death that occurs during pregnancy, childbirth, or within two months after giving birth or terminating a pregnancy. Worldwide, there are 430 maternal deaths per 100,000 live births.2 In Cambodia there are 437 deaths per 100,000 live births, making maternity-related complications one of the leading causes of death for Cambodian women ages 15 to 49. According to the 2000 Cambodia Demographic and Health Survey (CDHS), about 1 in 5 Cambodian women who died in the seven years preceding the survey died from pregnancy-related causes.3 The vast majority of these deaths could have been prevented through good quality care during pregnancy, delivery, and the postpartum period.
Caring for Expectant Mothers
Antenatal care can provide an essential link between women and the health system and deliver other essential health services to the expectant mother. Antenatal care offers providers the opportunity to detect and treat chronic conditions such as anemia and high blood pressure; to give advice on proper nutrition during pregnancy; and to help families plan for deliveries.
In Cambodia, over half (55 percent) of mothers do not receive any health care during pregnancy. Only 2 in 5 mothers receive antenatal care from trained medical personnel (doctors, nurses, and midwives). Regional differences in antenatal care is significant: 84 percent of mothers in Phnom Penh receive care from a trained health professional, as compared to only 20 percent in Mondol Kiri/Rotanak Kiri. Of those who do seek care, most get it from midwives (32 percent), with a smaller number seeking service from nurses (5 percent), and doctors (1 percent). Seven percent receive care from untrained traditional birth attendants (TBAs).4 More research is needed to identify and overcome obstacles that keep pregnant mothers from using antenatal services. Factors can include dissatisfaction with the attitudes of health staff; the time, costs, and difficulties associated with reaching service; and the preference of many women to be seen only by female health workers.
Maternal Nutrition Linked to Children’s Nutrition
A woman’s nutritional status has a direct bearing on her chances of surviving pregnancy and on her child’s likelihood of leading a healthy life. Calorie, vitamin, mineral, and protein requirements increase markedly during pregnancy. Women in resource-poor settings and those with little access to health care may be unable to meet these increased dietary requirements.
Iron deficiency is the most common form of maternal malnutrition and the most common cause of anemia. Iron deficiency anemia can be the result of lack of iron in the diet, poor absorption of dietary iron, malaria, or other parasitic infections. Mothers with severe anemia are at increased risk of complications during pregnancy and of maternal death. The United Nations Children’s Fund (UNICEF) estimates that anemia alone may contribute to as much as 20 percent of maternal mortality worldwide.5 In Cambodia, 66 percent of pregnant women are anemic (as are 55 percent of nonpregnant, nonlactating women).6 Pregnant women are at greater risk of anemia than nonpregnant women, as they pass some of their iron stores and other nutrients to their developing fetus.
Interventions to control iron deficiency include iron fortification of food staples, condiments, or other complementary foods. The use of iron/folate supplements to prevent iron deficiency in malaria-endemic regions has been endorsed by the World Health Organization (WHO) and the Asian Development Bank. Food and vitamin supplements to improve maternal nutrition should be part of a wide-scale development effort aimed at alleviating poverty, ensuring household food security, and promoting healthy diets.
Skilled Assistance at Delivery
Most births in Cambodia (89 percent) take place outside of health facilities (see Figure 1). The proportion of births delivered in a health facility is low in all regions (14 percent or less), except in Phnom Penh (71 percent). The fewest births in health facilities occur in Siem Reab/Otdar Mean Chey and Prey Veaeng (2 percent).7 Births at home can be safe, provided a woman’s family and attendants can recognize the signs of complications and, if complications occur, be able to move her to a facility where trained professionals can provide care. Unfortunately, too few births are attended by professionals able to recognize the signs of complications and provide the needed care. Training staff with midwifery skills and deploying them to underserved regions is critical to improvements in maternal and child health.
Figure 1
Births in Cambodia by Place of Delivery
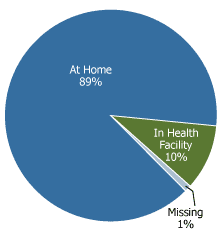
Source: Cambodia Demographic and Health Survey (CDHS) 2000.
Women are most in need of skilled care during delivery and the immediate postpartum period, when roughly three-fourths of all maternal deaths occur. Providing skilled care means ensuring that health professionals can manage normal deliveries and treat life-threatening complications of pregnancy and childbirth. WHO, UNICEF, and the United Nations Population Fund (UNFPA) have identified skilled assistance at delivery as among the most critical interventions to help prevent maternal deaths. With support from functioning health and transportation systems, these professionals can reduce maternal mortality by providing a hygienic environment and treating or stabilizing women when complications arise.
In Cambodia, only 32 percent of births are attended by a skilled professional. Twenty-eight percent of births are attended by midwives and 2 percent each by doctors and nurses (see Figure 2). Skilled assistance varies by residence, education level, age, and birth order. Urban women are more than twice as likely (57 percent) to receive assistance from a skilled professional during childbirth than rural women (28 percent). Women with secondary education or higher (66 percent) are also more likely to receive skilled assistance than women with no education (19 percent). Births to mothers under age 35 and first births are also more likely to be assisted by a trained health professional.8
Figure 2
Assistance at Delivery, Cambodia
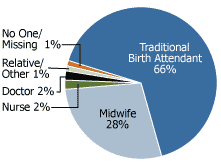
Source: Cambodia Demographic and Health Survey (CDHS) 2000.
Postpartum Care
Postpartum care is especially important for the health of a mother and her child. Of women worldwide who die of pregnancy-related causes, about a quarter die during pregnancy, about 15 percent at delivery, and 61 percent after delivery.9 Care during the postpartum period enables health workers to check that the mother and baby are doing well and if not, to detect and manage any postpartum problems early. It also offers providers the opportunity to encourage positive health behaviors such as breastfeeding and adequate nutrition; to counsel on hygiene and immunization; and to provide family planning and other reproductive health services.
In Cambodia, only 49 percent of mothers benefit from postpartum care. Unfortunately, few receive care from skilled professionals. About 1 in 7 women receive care from a midwife (14 percent); and only 1 percent each from a doctor or nurse. About one-third (34 percent) of women receive postpartum care from untrained TBAs. Skilled professionals are more likely to provide postpartum care to mothers in urban (27 percent) than in rural areas (14 percent), while rural women are more likely to receive care from untrained TBAs (34 percent) than urban women (28 percent).10
Consequences of Maternal Morbidity and Mortality for Policymakers
Because the vast majority of women who die from or are seriously injured by maternity-related causes are in the prime or their lives, their illnesses and deaths have serious social and economic consequences for their families and their communities. Newborns whose mothers die are less likely to survive. Surviving children are less likely to attend school regularly as they often must drop out to meet household needs. Additionally, since maternal deaths affect women in their most productive years, these deaths can have a deep impact on the local and national economies.
Support and commitment are needed to make the process of bringing new lives into the world safer for mothers. Maternal deaths can be prevented with improved maternal health, nutrition, and skilled care during pregnancy and immediately after childbirth. WHO’s Mother-Baby Package estimates that key health interventions cost only US$1 to US$3 per person.12 In addition, access to family planning can help to reduce both the number of unwanted pregnancies and unsafe abortions. Cambodia’s Safe Motherhood program has made lowering maternal mortality a public health priority. Reducing the tragic loss of mothers during this life-giving event will require well-coordinated and sustained efforts at all levels: in the home, in the community, in the clinic, in the country, and at the international level. This commitment will help ensure that motherhood is a safe, joyful, and rewarding experience.
References
- Elizabeth Ransom and Nancy Yinger, Making Motherhood Safer: Overcoming Obstacles on the Pathway to Care (Washington, DC: Population Reference Bureau, 2002).
- World Health Organization (WHO), Maternal Mortality in 1995: Estimates developed by WHO, UNICEF and UNFPA (Geneva: WHO, 2001).
- National Institute of Statistics (NIS), Directorate General for Health [Cambodia] and ORC Macro, Cambodia Demographic and Health Survey (CDHS) 2000 (Phnom Penh, Cambodia, and Calverton, Maryland: NIS Directorate General for Health and ORC Macro, 2001): 117.
- NIS, Directorate General for Health [Cambodia] and ORC Macro, CDHS 2000: 133.
- UNICEF, “Maternal Nutrition and Low Birthweight,” accessed online at www.unicef.org/programme/nutrition/focus/maternal.html, on Aug. 15, 2002.
- NIS, Directorate General for Health [Cambodia] and ORC Macro, CDHS 2000: 181.
- NIS, Directorate General for Health [Cambodia] and ORC Macro, CDHS 2000: 139.
- WHO, Maternal Mortality in 1995.
- Ann Starrs, The Safe Motherhood Action Agenda: Priorities for the Next Decade, report on the Safe Motherhood Technical Consultation (New York: Family Care International, 1998): 37.
- NIS, Directorate General for Health [Cambodia] and ORC Macro, CDHS 2000: 145.
For More Information
Please contact the Department of Planning and Health Information, Ministry of Health, #151-153, Blvd Kampuchea Krom Ave., Phnom Penh, Cambodia, Tel: (855 23) 425 368, E-mail: ratnary@bigpond.com.kh
