Leslie Elder
Director of Food and Nutrition Technical Assistance at the Academy for Educational Development

July 21, 2003
Director of Food and Nutrition Technical Assistance at the Academy for Educational Development
Former Policy Analyst
Malnutrition, defined as ill health caused by deficiencies of calories, protein, vitamins, and minerals interacting with infections and other poor health and social conditions, saps the strength and well-being of millions of women and adolescent girls around the world. [In this brief, the term malnutrition will refer to conditions of nutritional deficiency, including undernutrition and micronutrient deficiencies, though malnutrition actually also relates to problems of nutritional excess.]
Although malnutrition’s effects on this group have been recognized for decades, there has been little measurable progress in addressing the specific nutritional problems of women and adolescent girls. Ignorance about the symptoms of malnutrition, such as the lethargy and depression caused by iron deficiency, may be dismissed as “normal” or unimportant, further exacerbating the problem.1
Adequate nutrition, a fundamental cornerstone of any individual’s health, is especially critical for women because inadequate nutrition wreaks havoc not only on women’s own health but also on the health of their children. Children of malnourished women are more likely to face cognitive impairments, short stature, lower resistance to infections, and a higher risk of disease and death throughout their lives (see Figure 1).
Figure 1
Poor Nutrition Throughout the Life Cycle
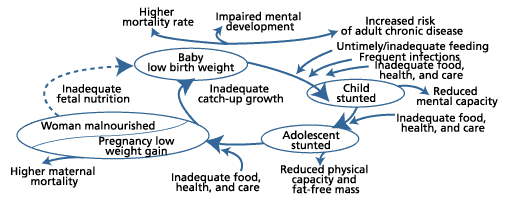
Source: Adapted from the ACC/SCN-appointed Commission on the Nutrition Challenges of the 21st Century.
Malnutrition poses a variety of threats to women. It weakens women’s ability to survive childbirth, makes them more susceptible to infections, and leaves them with fewer reserves to recover from illness. HIV-infected mothers who are malnourished may be more likely to transmit the virus to their infants and to experience a more rapid transition from HIV to full-blown AIDS. Malnutrition undermines women’s productivity, capacity to generate income, and ability to care for their families.
Addressing women’s malnutrition has a range of positive effects because healthy women can fulfill their multiple roles — generating income, ensuring their families’ nutrition, and having healthy children — more effectively and thereby help advance countries’ socioeconomic development. Women are often responsible for producing and preparing food for the household, so their knowledge — or lack thereof — about nutrition can affect the health and nutritional status of the entire family. Promoting greater gender equality, including increasing women’s control over resources and their ability to make decisions, is crucial. Improving women’s nutrition can also help nations achieve three of the Millennium Development Goals, which are commonly accepted as a framework for measuring development progress (see Table 1). This brief discusses the importance of improving women’s nutrition and suggests policy options for achieving positive change.
Table 1
Better Nutrition Helps Achieve Millennium Development Goals
| Millennium Development Goal | How Improving Women and Adolescent Girls’ Nutrition Helps |
|---|---|
| Goal #1: Eradicate extreme poverty and hunger. | |
| Halve, between 1990 and 2015, the proportion of people who suffer from hunger. |
|
| Goal #4: Reduce child mortality. | |
| Reduce, by two-thirds, between 1990 and 2015, the under-5 mortality rate. |
|
| Goal #5: Improve maternal health. | |
| Reduce by three-quarters, between 1990 and 2015, the maternal mortality ratio. |
|
Women are more likely to suffer from nutritional deficiencies than men are, for reasons including women’s reproductive biology, low social status, poverty, and lack of education. Sociocultural traditions and disparities in household work patterns can also increase women’s chances of being malnourished (see Box 1 at end of article). Globally, 50 percent of all pregnant women are anemic, and at least 120 million women in less developed countries are underweight.2 Research shows that being underweight hinders women’s productivity and can lead to increased rates of illness and mortality. In some regions, the majority of women are underweight: In South Asia, for example, an estimated 60 percent of women are underweight.
Many women who are underweight are also stunted, or below the median height for their age. Stunting is a known risk factor for obstetric complications such as obstructed labor and the need for skilled intervention during delivery, leading to injury or death for mothers and their newborns. It also is associated with reduced work capacity.3
Adolescent girls are particularly vulnerable to malnutrition because they are growing faster than at any time after their first year of life. They need protein, iron, and other micronutrients to support the adolescent growth spurt and meet the body’s increased demand for iron during menstruation. Adolescents who become pregnant are at greater risk of various complications since they may not yet have finished growing. Pregnant adolescents who are underweight or stunted are especially likely to experience obstructed labor and other obstetric complications. There is evidence that the bodies of the still-growing adolescent mother and her baby may compete for nutrients, raising the infant’s risk of low birth weight (defined as a birth weight of less than 2,500 grams) and early death.
Iron Deficiency and Anemia
Iron deficiency and anemia are the most prevalent nutritional deficiencies in the world. The body uses iron to produce hemoglobin, a protein that transports oxygen from the lungs to other tissues in the body via the blood stream, and anemia is defined as having a hemoglobin level below a specific level (less than 12 grams of hemoglobin per deciliter of blood [g/dl] in nonpregnant women; less than 10 g/dl in pregnant women).4 Most women who develop anemia in less developed countries are not consuming enough iron-rich foods or are eating foods that inhibit the absorption of iron. However, malaria can also cause anemia and is responsible for much of the endemic anemia in some areas. Other causes of anemia include hookworm and schistosomiasis, HIV/AIDS, other micronutrient deficiencies, and genetic disorders.
Anemia affects about 43 percent of women of reproductive age in less developed countries. Women are especially susceptible to iron deficiency and anemia during pregnancy, and about half of all pregnant women in less developed countries are anemic, although rates vary significantly among regions.5 Iron deficiency and anemia cause fatigue, reduce work capacity, and make people more susceptible to infection. Severe anemia places women at higher risk of death during delivery and the period following childbirth.6 Recent research suggests that even mild anemia puts women at greater risk of death.7
Iodine Deficiency
Failing to meet the body’s iodine requirements impairs mental functioning and can cause goiter (a swelling of the thyroid gland) and hypothyroidism, a condition marked by fatigue and weakness. Among adolescent girls, iodine deficiency may cause mental impairments, impede physical development, and harm school performance. Although programs to iodize salt have reduced the prevalence of iodine deficiency disorders dramatically in the past 10 years, there is still wide variation in household access to iodized salt, ranging from 80 percent in Latin America to 28 percent in Central and eastern Europe. At least 130 countries have serious pockets of iodine deficiency disorders.
Vitamin A Deficiency (VAD)
VAD, which can cause growth retardation and impaired vision, remains a significant public health issue among populations that do not consume enough vitamin A, which is found in animal products and certain fruits, including mangos. Severe VAD causes blindness; less severe VAD impairs the immune system, making people more susceptible to infection and putting them at increased risk of death. Concurrent infection with parasites and illnesses such as diarrhea, as well as having several pregnancies too close together, can exacerbate VAD. Pregnant women are especially vulnerable to VAD. In Nepal, for example, where VAD is prevalent in some communities, as many as one in 10 pregnant women experience night blindness due to VAD.8
Low Birth Weight
A variety of nutritional deficits, including iron deficiency and insufficient caloric intake, can increase a woman’s chances of having a low birth-weight infant. Low birth weight affects more than 20 million infants in less developed countries every year and is the strongest determinant of a child’s survival.10 Infants with low birth weight account for the majority of infant deaths in the first week of life in many less developed countries and are at higher risk of death throughout infancy. Those who survive tend to remain shorter and lighter than their peers, which damages their ability to work during adulthood. Low birth-weight infants often suffer from cognitive impairment, developmental problems, and a greater susceptibility to illness. Low birth weight is also associated with a higher burden of disease and early mortality.
Women’s deprivation in terms of nutrition and health care rebounds on society in the form of ill-health of their offspring — males and females alike. – Siddiq Osmani and Amartya Sen
Micronutrient Deficiencies
Micronutrient deficiencies in mothers place their infants at risk, since the fetus receives essential nutrients from the mother. Even mild maternal malnutrition can impair fetal development.
Iron
Anemia is responsible for about 35 percent of preventable low birth weight: Because less iron is transferred from anemic mothers to their fetuses, babies are at risk of iron deficiency and anemia early in infancy.11 Infants born to mothers with anemia are at greater risk of low birth weight, premature birth, and impaired cognitive development.12
Vitamin A
Low maternal stores of vitamin A compromise children’s stores of vitamin A, putting those children at greater risk of illness and death. A recent study showed that providing vitamin A supplements to pregnant women with HIV in Malawi improved birth weight and neonatal growth and reduced the prevalence of anemia in infants, as well as reducing rates of HIV transmission from mothers to infants.13
Iodine
Mothers who do not consume enough iodine are more likely to miscarry or have a stillborn child. The physical growth and mental development of the children who do survive is often severely impaired, and children may suffer irreversible mental retardation.14 In areas where iodine deficiency is widespread, providing iodine supplements to pregnant women has led to decreased infant mortality and higher birth weights.15
Folate and Other B Vitamins
Folate deficiency at the time of conception can cause neural tube defects in infants, and maternal zinc deficiency is associated with preterm delivery, low birth weight, and increased infant mortality. Other B vitamins, including B6 and B12, are important for ensuring children’s healthy neurological development.
Malnutrition in women leads to economic losses for families, communities, and countries because malnutrition reduces women’s ability to work and can create ripple effects that stretch through generations. Countries where malnutrition is common must deal with its immediate costs, including reduced income from malnourished citizens, and face long-term problems that may be related to low birth weight, including high rates of cardiac disease and diabetes in adults.16
Illnesses associated with nutrient deficiencies have significantly reduced the productivity of women in less developed countries. It is difficult to determine exactly what proportion of those losses are due to maternal malnutrition, but recent research indicates that 60 percent of deaths of children under age 5 are associated with malnutrition — and children’s malnutrition is strongly correlated with mothers’ poor nutritional status.17 Problems related to anemia, for example, including cognitive impairment in children and low productivity in adults, cost US$5 billion a year in South Asia alone.18 Illness associated with nutrient deficiencies have significantly reduced the productivity of women in less developed countries.19 A recent report from Asia shows that malnutrition reduces human productivity by 10 percent to 15 percent and gross domestic product by 5 percent to 10 percent.20 By improving the nutrition of adolescent girls and women, nations can reduce health care costs, increase intellectual capacity, and improve adult productivity.21
The Millennium Development Goals established by the UN member states in 2000 challenge nations to create effective interventions to improve women’s and adolescent girls’ nutrition. Taking such action not only improves the health of girls and women today, it has far-reaching intergenerational effects that can help countries develop.
Preventing malnutrition requires a political commitment. Public health systems need to prevent and treat micronutrient deficiencies, encourage households to meet the dietary needs of women and adolescent girls throughout their lives, and ensure their access to high-quality health services, clean water, and adequate sanitation. Policymakers should also address women’s low social status and ensure that girls have access to education — which should include information on nutrition. Such policy measures can help increase women’s age at first pregnancy, an important determinant of maternal health and child survival, and can encourage women to space their births.
Improve Nutrition Throughout Women’s Lives
Addressing the needs of girls and women throughout their lives — the “life cycle approach” — can improve women’s nutritional status. Many nutritional deficits experienced in infancy and childhood have irreversible consequences, so interventions to support adequate nutrition from infancy onward directly benefit women later in life. Because the causes of malnutrition are rarely simple, programs need to address the range of factors determining the target population’s nutrition. It is also important that the community be involved in developing and supporting the interventions and that programs ensure that their approaches do not conflict.
Infancy
Exclusive breastfeeding during the first six months of an infant’s life benefits both mother and child. Breastfeeding protects infants and children from illness and helps ensure healthy growth and development, and starting breastfeeding soon after birth may help prevent excessive maternal bleeding. Breastfeeding for up to two years can also help mothers keep their iron levels up by delaying the return of menstruation. Estimates suggest that improving breastfeeding practices by encouraging women to breastfeed their infants immediately after birth and to avoid supplemental feeding for at least the first six months could save the lives of 1.5 million children each year.22
Childhood
In late infancy and early childhood, children should receive adequate amounts of appropriate food — and, if necessary, supplements of iron and other nutrients — to complement their continued intake of breast milk and as they are weaned. Monitoring whether the children in a community are growing can help families identify and address problems, including vitamin deficiencies and infections. Common supplements for children include iron, vitamin A, and iodine. Iron is critical for cognitive development during the first two years of life, and girls may be at particular risk of iron deficiency if scarce iron-rich foods are given mainly to boys. Fortifying cereals with iron, although helpful, may not be enough, so children may need iron supplements. Iodine can be provided in iodized salt, although it is important that the level of fortification be monitored by national authorities.23
Adolescence
Adolescent girls need access to information and services related to nutrition, reproductive health, family planning, and general health. Programs can reach girls through a variety of avenues, including schools, workplaces, marriage registration systems, and youth-oriented health programs. Schools can be a key part of helping adolescent girls become healthy adults: Research shows that promoting female education and literacy can improve nutrition and encourage females to seek regular health care.24 Ensuring that adolescent girls receive enough food, iron and folate supplements, and iron and iodine-fortified foods, as well as helping them delay their first pregnancy and protect themselves from sexually transmitted infections and other diseases, can help girls become healthy women. Teaching girls to use their knowledge of nutrition when preparing and handling food can also improve their health and that of their families: In Peru, for example, adolescent girls participating in community kitchens learned to enhance their diets by adding low-cost iron-rich items, such as chicken livers, and foods that enhance iron absorption, including lemons.
In communities where many adolescent girls are underweight, supplements may improve girls’ overall health and their pregnancy outcomes, including reducing their risk of bearing low birth-weight babies. In India and Egypt, for example, where iron supplements have been given out in schools, the prevalence of anemia has fallen significantly.25 Interventions that reach adolescents help establish healthy habits that continue into adulthood. Such programs should also involve males: Boys who receive information about women’s increased nutritional requirements during pregnancy and lactation may be better partners when they form families.
Pregnancy
Pregnancy is typically the first point after early childhood when women seek out and receive health services. Because even women who have not used health care services in the past often make contact with health systems when pregnant, it is vital that nutrition interventions be integrated into antenatal care programs.
Women should consume daily iron and folate supplements when they are pregnant and for at least three months after childbirth and should receive other micronutrients as needed. In areas where many women suffer chronic energy deficiency and there is a high incidence of low birth weight, pregnant and lactating women may need high-energy food supplements. Educational programs and public information campaigns can also help address cultural norms that prevent women from eating enough (see Box 1 at end of article).26
The Postpartum Period
Women’s energy requirements remain high after delivery, especially when women are breastfeeding, so it is important that they continue to receive enough food. Women require approximately 50 percent more calories while breastfeeding than they need during pregnancy. Maintaining adequate levels of vitamin A is particularly important for nursing mothers, since vitamin A is passed on to the infant through breast milk and can help reduce the risk of maternal and infant illness and death. Nursing mothers should receive supplements of vitamin A if necessary.27
Lifetime Nutrition
Efforts to improve the nutrition of entire populations do benefit women, and governments can use a variety of approaches to ensure that their citizens receive enough calories and nutrients. Teaching people about which local foods, such as mangos, papayas, and chicken livers, contain essential nutrients can help diversify diets. Programs can also improve nutrition by fortifying widely consumed staple foods to deliver iron, iodine, vitamin A, and other micronutrients to large populations. In China and Vietnam, for example, researchers have found that fortifying soy sauce and fish sauce with iron has helped reduce anemia in all population groups in the areas where the projects were conducted.28 Other countries have successfully fortified sugar with vitamin A and wheat flour with iron.29 Agricultural policies that promote the production of nutritionally rich crops and techniques that add nutritional value to food crops, fish, and livestock can also help promote health, as can providing clean water and improving sanitation to prevent the transmission of intestinal parasites that can exacerbate existing malnutrition.30
In areas where most mother suffer from malnutrition, giving women energy-rich food during interbirth intervals may increase the birth weight of the next child.31 Increasing the amount of time between births is also thought to be helpful because it helps women’s bodies rebuild their stores of fat and micronutrients, leading to improved maternal health as well as better pregnancy outcomes.
Several important non-nutrition interventions lead to improved birth weight and better maternal health and nutritional: treating women for parasitic infections, including hookworm; providing preventive doses of antimalarial drugs; encouraging the use of insecticide-treated bed nets; and counseling women about the dangers of smoking and how to reduce their exposure to indoor air pollution.
Improve Women’s Status
Policymakers can help improve women and children’s nutrition by addressing women’s low status in society. Gender inequalities are often greatest among the poor, particularly in terms of household investments in health and education.33 Addressing gender inequalities can help ensure that women can get the nutrition they need, improving their own health and that of their families and, ultimately, contributing to their societies’ development.
The quality of care and feeding offered to children … is critically dependent on women’s education, social status, and workload. – UN Sub-Committee on Nutrition
Research indicates that women who have greater control over household resources tend to be healthier and better nourished — as do their families — because women tend to spend more on the nutrition, health, and well-being of their households. In addition to being responsible for preparing food, women often make significant contributions to their families’ production of essential crops. In sub-Saharan Africa, for example, women provide 60 percent to 80 percent of the labor involved in producing food for household consumption and sale.34
For these reasons, programs to improve nutrition should focus on increasing women’s knowledge about nutrition and their decisionmaking power. One program in Kenya, for example, worked with women farmers to encourage them to raise and serve orange-fleshed sweet potatoes, which are higher in vitamin A than those traditionally raised in the region. The women received planting materials, nutrition education, and training in preparing the sweet potatoes for market sale and household consumption.35
Microfinance programs, which provide women with small loans for their businesses, are another way to raise women’s status and improve their ability to provide for themselves and for their families. In Ghana, for example, an innovative health program combined health education with access to microfinance. Women received village banking services, including access to loans, as well as education about breastfeeding, child nutrition, diarrhea treatment and prevention, immunization, and family planning practices. An assessment conducted three years after the program began found that participants’ 1-year-old children were healthier and better nourished than those of nonparticipants.36
Track Indicators of Women’s Nutrition
Data on women’s nutritional status can be a powerful tool for informing communities and governments about the nature, extent, and consequences of female malnutrition, but data need to be collected regularly, analyzed, and disseminated.
Policymakers should ensure that data on the prevalence of birth weight, the number of children who are underweight and how many of them are girls, and anemia prevalence among adolescent girls and women of reproductive age are collected. Policymakers can also make the government and program managers accountable for improving outcomes. Because nutrition is affected by a complex set of factors, governments and programs are most likely to succeed in addressing malnutrition if they approach the problem from a variety of angles. The impact of programs and policies dealing with health, agriculture, food security, and water and sanitation should be taken into account.
Adequate nutrition is important for women not only because it helps them be productive members of society but also because of the direct effect maternal nutrition has on the health and development of the next generation. There is also increasing concern about the possibility that maternal malnutrition may contribute to the growing burden of cardiovascular and other noncommunicable diseases of adults in less developed countries. Finally, maternal malnutrition’s toll on maternal and infant survival stands in the way of countries’ work toward key global development goals.
Acknowledgments
Leslie Elder and Elizabeth Ransom prepared this brief. Robert Johnson prepared a first draft, and PRB staff members, including Lori Ashford, Liz Creel, Vijay Rao, and Nancy Yinger, reviewed early drafts of the brief. Lisa Colson, Britt Herstad, and Haruna Kashiwase helped prepare the figures in the text. Special thanks are due to the technical experts who reviewed the brief, including Eunyong Chung, Frances Davidson, Charlotte Johnson-Welch, Kathleen Kurz, Luann Martin, and Mary Ellen Stanton.
