
Americans Living Longer, Not Necessarily Healthier, Lives
(March 2001) Questions about the health of older people have arisen as mortality at older ages has decreased remarkably over the last 30 years. Reductions in mortality from heart disease are the major reason for this trend, but death rates from almost all major diseases typically experienced at older ages also have declined. Consequently, there has been an increase in life expectancy after age 65 and even after age 85. But are older Americans healthier today than they were a generation ago? The answer depends on which indicator of health is used to measure change.
Figure 2
Causes of Death in the United States, Selected Years, 1950 to 1998
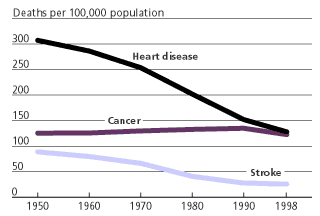
Source: PRB, based on data from the National Center for Health Statistics.
We know heart disease death rates have fallen dramatically (see Figure 1). It is possible that this has come about because heart disease has been prevented or because people are experiencing its onset at older ages. But most of the evidence so far indicates that falling mortality rates are due to better treatment, allowing people to live longer following the onset of heart disease. As people live longer with the disease, the number of older people reporting that they have it has increased.
Improvement in health does not necessarily accompany an increase in life expectancy since only about half of the disability and functioning loss at older ages is caused by lethal diseases. The other half is caused by conditions that are not linked to mortality trends, including arthritis, vision loss, and Alzheimer’s disease. This means that some people are surviving heart disease but suffering from crippling arthritis or dementia (see Figure 2). Nonlethal diseases are thus going to become increasingly important causes of disability and functioning loss in old age unless they too can be delayed or eliminated.
Figure 2
Percent of People Ages 70 and Older Who Reported Having Selected Chronic Conditions, by Sex, 1984 and 1995
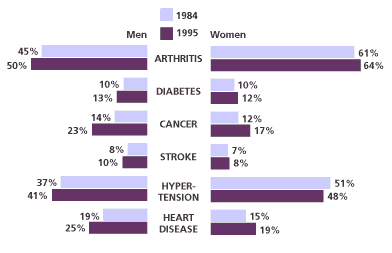
Note: 1984 percentages are age-adjusted to the 1995 population. Reference population: These data refer to the civilian noninstitutional population.
Source: Federal Interagency Forum on Aging Related Statistics, Older Americans 2000: Key Indicators of Well-Being.
Health care for older people is moving toward delaying the onset and progression of both lethal and nonlethal diseases and providing people with the personal and home care they need to cope with the disabilities that stem from these conditions. Delaying onset and progression requires both pharmaceutical and behavioral interventions. Many people from advanced middle age onward are using drugs to control both hypertension and cholesterol in the hope of delaying or preventing the onset of clinical heart disease. New generations of drugs have been developed to control the loss of functioning and disability associated with arthritis. Because approximately half the older population has this condition, for which there is no cure, a large proportion of people are likely to use these drugs for some period of their lives. The use of medication to delay the disability connected with diseases such as Alzheimer’s is going to increase markedly in the near future.
Current approaches to disease control are the result of the expansion of biological knowledge of the basic disease processes. Continued growth in this knowledge — some of it coming from better understanding of the human genome — will greatly increase our ability to intervene early in the prevention of disease and disability.
The overall reduction in mortality, increasing life expectancy from 40 to 75 years, is regarded by many as the central accomplishment of the 20th century. In 1900, we would not have predicted our ability to so effectively reduce death at younger ages from infectious diseases. The development of the germ theory of disease at the end of the 19th century laid the groundwork for this marked improvement in life expectancy. Deeper understanding of the human genome and of the biology of aging at the end of the 20th century has similarly provided a foundation for the delay and prevention of the major diseases and conditions of old age.
By the end of this century, we will certainly live longer, and we should not suffer from heart disease or cancer until much later in life. However, unless we die in perfect health, we will still have a period of disease and disability before death.
As life expectancy has increased, emphasis has shifted from quantity to quality of life. Researchers and policymakers are increasingly focusing on how to extend healthy and active life. This has resulted in a growing use of measures of expected healthy life or life without disease or disability, in addition to traditional measures of life expectancy, to monitor health trends and health differences.
Eileen M. Crimmins is Edna M. Jones Professor of Gerontology at the Andrus Gerontology Center of the University of Southern California in Los Angeles.
References
Andrew Bebbington, Margaret Bone, Carol Jagger, Kevin Morgan, and Geraldine Nicolaas, Health Expectancy and Its Uses (London: Her Majesty’s Stationery Office, 1995 [DP1047/3]).
Margaret L. Campbell, Eileen M. Crimmins, Mitchell P. LaPlante, Michelle Putnam, Fernando Torres-Gil, and Barbara Silverstone, “Is Disability Declining Among the Elderly? Trends and Implications for the Next Millennium,” Critical Issues in Aging 2 (1998): 9-13.
J. Chen and W. J. Millar, “Are Recent Cohorts Healthier Than Their Predecessors?” Health Reports 11, no. 4 (Ottawa, Ontario: Statistics Canada, Spring 2000): 9-23.
Eileen M. Crimmins and Yosuhito Saito, “Change in the Prevalence of Diseases Among Older Americans: 1984-1994,” Demographic Research 3, no. 9 (2000). Available online at www.demographic-research.org/volumes/vol3/9/.
Eileen M. Crimmins, Sandra L. Reynolds, and Yosuhito Saito, “Trends in Health and Ability to Work Among the Older Working-Age Population,” Journal of Gerontology 54B, no. 1 (1999): S31-40.
Eileen M. Crimmins, Yosuhito Saito, and Sandra L. Reynolds, “Further Evidence on Recent Trends in the Prevalence and Incidence of Disability Among Older Americans From Two Sources: the LSOA and the NHIS,” Journal of Gerontology: Social Sciences 52B, no. 2 (1997): S59-71.
Eileen M. Crimmins, “Mixed Trends in Population Health Among Older Adults,” Journal of Gerontology: Social Sciences 51B, no. 5 (1996): S223-S225.
Eileen M. Crimmins, “Evidence on the Compression of Morbidity,” Gerontologica Perspecta 1 (1987): 45-49.
Eileen M. Crimmins, “Are Americans Healthier As Well As Longer-Lived?” Journal of Insurance Medicine 22, no. 2 (1990): 89-92.
Vicki A. Freedman and Linda G. Martin, “Understanding Trends in Functional Limitations Among Older Americans,” American Journal of Public Health 88 (1998): 1457-1462.
Kenneth G. Manton, Larry Corder, and Eric Stallard, “Chronic Disability Trends in Elderly United States Populations: 1982-1994,” Proceedings of the National Academy of Sciences 94 (1997): 2593-2598.
Kenneth G. Manton, Eric Stallard, and Larry Corder, “Changes in Morbidity and Chronic Disability in the U.S. Elderly Population: Evidence From the 1982, 1984, and 1989 National Long Term Care Surveys,” Journal of Gerontology: Social Sciences 50B (1995): S194-204.
Sandra L. Reynolds, Eileen M. Crimmins, and Yosuhito Saito, “Cohort Differences in Disability and Disease Presence,” The Gerontologist 38, no. 5 (1998): 578-590.
Jean-Marie Robine, Pierre Mormiche, and C. Sermet, “Examination of the Causes and Mechanisms of the Increase in Disability-Free Life Expectancy,” Journal of Aging and Health 10, no. 2 (1998): 171-191.
Lois M. Verbrugge and A.M. Jette, “The Disablement Process,” Social Science and Medicine 38, no. 1 (1994): 1-14.
Timothy A. Waidmann, John Bound, and Michael Schoenbaum, “The Illusion of Failure: Trends in the Self-Reported Health of the U.S. Elderly,” The Milbank Quarterly 73, no. 2 (1995): 253-287.
