Sandra Yin
Former Associate Editor

January 1, 2006
Former Associate Editor
As avian flu kills a growing number of people and outbreaks of the virus are reported in birds from China to Turkey, public health officials fear a new global influenza pandemic could already be brewing.
Mindful of the deadly 1918-1919 flu epidemic—which killed an estimated 50 million people worldwide—vaccine manufacturers are racing to develop a preventive vaccine as countries scramble to stockpile existing flu vaccines.1 But while experts agree that another global influenza pandemic is inevitable, no one knows when or where the next flu pandemic will emerge, how severe it will be, or even if the new virus will be its source. What we do know is that the current virus bears some resemblance to the 1918 strain, which attacked alarmingly large numbers of healthy young adults.
| Year | Worldwide | United States |
|---|---|---|
| 1918-1919 | 50,000,000 | 675,000 |
| 1957-1958 | 2,000,000 | 60,000 |
| 1968-1969 | 1,000,000 | 40,000 |
Sources: Lone Simonsen et al., “Pandemic Influenza and Mortality,” in The Threat of Pandemic Influenza, eds. Stacey Knobler et al. (2005); Centers for Disease Control and Prevention, “Researchers Reconstruct 1918 Pandemic Influenza Virus,” (www.cdc.gov, accessed on Dec. 12, 2005); and World Health Organization, “Ten Things You Need to Know about Pandemic Influenza,” (www.who.int, accessed Dec. 12, 2005).
Avian influenza, or “bird flu,” is a contagious disease caused by viruses that normally infect birds only.2 In rare instances, the virus crosses the species barrier and infects pigs or humans.3 Outbreaks of bird flu in poultry put humans at risk of direct infection.4
The consequences can be dramatic: The 1918 flu epidemic—which scientists believe was caused by an avian-like virus—killed 675,000 people in the United States in addition to its global death toll (see Table 1).5 In contrast, seasonal flu kills an average of 36,000 people per year in the United States.6
Health authorities have been monitoring a new and extremely pathogenic virus—the avian influenza A (H5N1)—since 1997, when a human case was first documented in Hong Kong.7 Of the few bird flu viruses in recent years that have jumped the species barrier, H5N1 has already caused the largest number of cases of severe disease and death in humans.8
The World Health Organization (WHO) began counting human cases of H5N1 in 2003, when three laboratory-confirmed cases in Vietnam all ended in deaths. By early 2006, WHO had linked 78 deaths to the virus out of 147 reported cases of H5N1 bird flu in humans.9 Human cases have been confirmed in six countries: Cambodia, Indonesia, Thailand, Vietnam, China, and Turkey (see Table 2).10
| Countries with confirmed cases | Year of onset | Total | ||||
|---|---|---|---|---|---|---|
| 2003 | 2004 | 2005 | 2006 | |||
| Cambodia | Deaths | 0 | 0 | 4 | 0 | 4 |
| Cases | 0 | 0 | 4 | 0 | 4 | |
| China | Deaths | 0 | 0 | 5 | 0 | 5 |
| Cases | 0 | 0 | 7 | 1 | 8 | |
| Indonesia | Deaths | 0 | 0 | 11 | 0 | 11 |
| Cases | 0 | 0 | 16 | 0 | 16 | |
| Thailand | Deaths | 0 | 12 | 2 | 0 | 14 |
| Cases | 0 | 17 | 5 | 0 | 22 | |
| Turkey | Deaths | 0 | 0 | 0 | 2 | 2 |
| Cases | 0 | 0 | 0 | 4 | 4 | |
| Vietnam | Deaths | 3 | 20 | 19 | 0 | 42 |
| Cases | 3 | 29 | 61 | 0 | 93 | |
| Total | Deaths | 3 | 32 | 41 | 2 | 78 |
| Cases | 3 | 46 | 93 | 5 | 147 | |
Note: Cases are laboratory-confirmed cases reported to WHO as of Jan. 10, 2006.
Source: World Health Organization, Cumulative Number of Confirmed Human Cases of Avian Influenza A/(H5N1) Reported to WHO (www.who.int, accessed Jan. 10, 2006).
Avian flu is normally difficult to catch from a bird. But of the 15 extant bird flu virus subtypes, H5N1 is particularly worrisome: It mutates rapidly, has a documented propensity to acquire genes from viruses infecting other animal species, and can cause severe disease in humans.11
Unlike seasonal influenza, which usually leads to only mild respiratory symptoms such as fever, cough, sore throat, and muscle aches, H5N1 has caused severe respiratory illness that can lead to rapid deterioration, life-threatening complications, and what appears to be high probability of fatality. Primary viral pneumonia and multiple organ failure are common hallmarks.12
The spread of H5N1 virus from person to person has thus far been rare and not continued beyond one person.13 However, scientists worry that the H5N1 virus may morph into a form that spreads easily from one person to another. Such a change could signal the beginning of a global outbreak, or pandemic.14
The H5N1 flu virus bears some similarities to the 1918-1919 outbreak, the most deadly influenza virus of the 20th century (see Table 1). The 1918 virus may have started out as an avian flu virus that later adapted to humans.15 In addition, certain genes in the 1918 flu allowed it to replicate efficiently in human bronchial cells—genes similar to some found in H5N1.16
What’s more, recent research has shown that human lung cells infected with the H5N1 bird flu virus become intensely inflamed, responding more vigorously to the virus than to an ordinary flu virus.17 Autopsies of H5N1 avian flu victims have revealed lungs choked with debris from the excessive inflammation. Similar lung damage was reported by doctors in 1918-19 flu victims.18
But it remains unclear whether the next flu pandemic will rival the death toll of the 1918 pandemic or be less fatal, such as the pandemics of 1957 and 1968.19 And the H5N1 virus is not guaranteed to lead to an epidemic. However, as long as the H5N1 virus continues to circulate in birds, human infections will be possible and a risk of pandemic will exist—a situation that could drag on for years.20 In the best-case scenario, H5N1 could die out in birds and no longer pose a pandemic risk among humans.
“There will be another pandemic,” says Michael Osterholm, director of the Center for Infectious Disease Research & Policy at the University of Minnesota. “But I can’t tell you it will be H5N1.”
Although health officials can’t predict when the next flu epidemic will strike, they worry that a new pandemic could be more devastating than earlier ones, given changes in population, demographics, and lifestyle over the past three decades.
The rise in international travel could speed the spread of viruses around the world. And once the virus arrives somewhere, it could also spread quickly within populations because of increased urbanization. The potential for more complications and deaths could also grow because of a rise in the number of elderly people, and by extension, those living with chronic medical conditions.
Researchers are still trying to explain what made the 1918 virus so deadly. Berkeley demographer Andrew Noymer believes tuberculosis, or TB, played a role in the 1918 epidemic in the United States.21 Looking at mortality patterns in the United States after the epidemic, Noymer discovered that death rates from TB fell dramatically in 1919 and 1920. He found that many who died from the flu had underlying TB.
Noymer says that the flu turned into pneumonia in many people during the 1918 outbreak, and that these pneumonia cases became especially severe in people with compromised lungs. Their early demise depressed the death rate from TB for many years. “If H5N1 were transmitted from human to human, then we could expect higher death rates in developing countries where TB is prevalent,” Noymer says.
On the other hand, infectious disease experts believe young adults’ strong immune response may have made that group more susceptible during the 1918 pandemic. In contrast to seasonal flu, which tends to target the elderly, one of the 1918-1919 pandemic’s most striking features was its ability to kill people in the prime of life—the people with the strongest immune systems.22 The death curve of this pandemic was “W-shaped,” peaking for babies and children under age 5, the elderly, and people ages 25 to 34 (see figure).
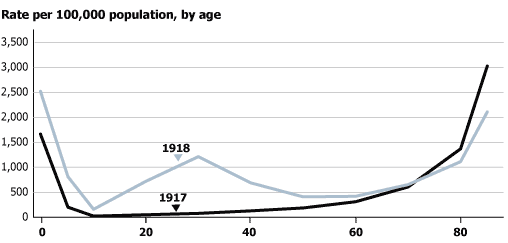
Source: U.S. Department of Health, Education, and Welfare (1956).
Osterholm speculates that the stronger immune response of young adults translated into harsher symptoms during the 1918-19 pandemic, as their immune system attacked good bystander cells as well as infected ones—in effect, destroying lungs in order to kill the virus.
If an H5N1-based pandemic virus were to emerge, no one would have built-in immunity, and a vaccine that targets specifically that virus would not be available for six to eight months—and even then only in “dribs and drabs,” according to Osterholm. Given that the demand for vaccine would far outweigh supply, public health officials will need to define high-priority groups for vaccinations. The populations deemed most at risk, given the nature of the virus, would be the first to be vaccinated. Others would likely have to go without.
Analysts warn that the world needs to start preparing for an influenza pandemic now to avert a public health crisis. But influenza research has not been a health priority for decades. From the end of World War II until only recently, almost no flu research was conducted. And after WWII, the United States virtually abandoned research into vaccine technology. The result: 1930s chicken egg-based technology is still used to make most vaccines.
“We assumed that infectious diseases were conquered,” says Victoria Harden, director of the National Institutes of Health Office of NIH History and Stetten Museum. She urges government officials to support ongoing vaccine development.
“Policymakers should never assume any disease has been conquered,” Harden says, “because nature continually surprises us.”
Sandra Yin is associate editor at the Population Reference Bureau.
Suggested Reading
John M. Barry, The Great Influenza: The Epic Story of the Deadliest Plague in History (New York: Penguin, 2004).
Alfred W. Crosby, America’s Forgotten Pandemic: The Influenza of 1918 (Cambridge: Cambridge University Press, 1989).
Stacey L. Knobler et al. (eds.), The Threat of Pandemic Influenza: Are We Ready? (Washington, DC: The National Academies Press, 2005).
Gina Kolata, Flu: The Story of the Great Influenza Pandemic of 1918 and the Search for the Virus That Caused It (New York: Simon & Schuster, 1999).
Howard Phillips and David Killingray (eds.), The Spanish Influenza Pandemic of 1918-19: New Perspectives (London: Routledge, 2003).
