
Children's Environmental Health: Risks and Remedies
Date
July 29, 2002
Author
View / Download
Overall child mortality declined significantly in the 1990s, but environmental hazards still kill at least 3 million children under age 5 every year.1
Such young children make up roughly 10 percent of the world’s population, but comprise more than 40 percent of the population suffering from health problems related to the environment.2 Children worldwide require special protection from longstanding risks such as smoke from traditional fuels and from emerging risks such as exposure to an increasing number of hazardous chemicals.
Although new regulatory standards and greater awareness of children’s vulnerability to such hazards have improved children’s situation in a number of more developed countries, many children, especially in less developed countries, continue to be exposed to toxins. Their vulnerability is exacerbated by the lack of protective policies and medical and public health interventions. Short-term curative responses can save some lives, but addressing underlying risk factors is key for long-term change. Efforts to measure children’s environmental health risks, develop policies and programs to mitigate such exposures worldwide, and strengthen efforts to address the problem at all levels are needed. This policy brief, part of PRB’s Emerging Policy Issues in Population, Health, and Environment series, explores children’s special vulnerability, outlines the risks and the conditions that increase such risks, and highlights what is being done to address the problem.
Children’s Vulnerability
Due to their size, physiology, and behavior, children are more vulnerable than adults to environmental hazards. Children are more heavily exposed to toxins in proportion to their body weight, and have more years of life ahead of them in which they may suffer long-term effects from early exposure.3 Perinatal conditions, which can be influenced by environmental conditions, cause 20 percent of deaths worldwide in children under age 5.4 Furthermore, fetal exposure to chemicals such as lead increases a child’s chances of having brain damage or developmental problems. Children at all ages, not just the very young, are at greater risk than adults. Children under age 5 breathe more air, drink more water, and eat more food per unit of body weight than adults do, so they may experience higher rates of exposure to pathogens and pollutants. Typical childhood behaviors, such as crawling and putting objects in the mouth, can also lead to increased risks. Children between ages 5 and 18 may face higher risks of injuries, including exposure to hazardous chemicals, due to their growing participation in household chores and work outside of the home. Many school-age children attend schools without sanitation facilities, making them more likely to contract various diseases and less likely to go to school. According to UNICEF, about 10 percent of school-age African girls either do not attend school during menstruation or drop out at puberty because of the lack of sanitary facilities.5
Environmental Risks to Children’s Health
Indoor Air Pollution
Half of the world’s households use biomass fuels, including wood, animal dung, or crop residues, that produce particulates, carbon monoxide, and other indoor pollutants. The World Health Organization (WHO) has determined that as many as 1 billion people, mostly women and children, are regularly exposed to levels of indoor air pollution that are up to 100 times those considered acceptable.6 Young children, who spend more time indoors, are more exposed to the noxious byproducts of cooking and heating. In India, where 80 percent of households use biomass fuel, estimates show that nearly 500,000 women and children under age 5 die every year from indoor pollution, largely from acute respiratory infections (ARIs).7 The figure for other less developed countries is similar.8
Exposure to indoor pollutants can cause or aggravate ARIs, including upper respiratory infections such as colds and sore throats, and lower respiratory infections such as pneumonia. Acute lower respiratory infections are one of the primary causes of child mortality in developing countries, and led to 2.2 million deaths in children under age 5 in 2001.9 ARIs can also increase mortality from measles, malaria, and other diseases. Other factors that can worsen ARIs include low birth weight, poor nutrition, inadequate housing and poor hygiene conditions, overcrowding, and reduced access to health care.
Asthma Studies in less developed countries have linked indoor air pollution to lung cancer, stillbirths, low birth weight, heart ailments, and chronic respiratory diseases, including asthma.10 Asthma, a disease characterized by recurrent attacks of breathlessness and wheezing, affects between 100 million and 150 million people worldwide. The disease causes over 180,000 deaths every year, including 25,000 children’s deaths.11 Worldwide rates of asthma have risen by 50 percent every 10 years since 1980; urbanization and increased time spent indoors are strongly associated with this increase.12 According to WHO, prevalence of asthma symptoms in children in Brazil, Costa Rica, Panama, Peru, and Uruguay varies from 20 percent to 30 percent; in Kenya, it approaches 20 percent.13
The strongest risk factors for development of asthma appear to be exposure to indoor allergens and a family history of asthma or allergies. Exposure to environmental tobacco smoke (ETS, or secondhand smoke), chemical irritants, air pollutants, and cold weather are also risk factors for the disease, as are low birth weight, respiratory infections, and physical exercise. Children whose mothers smoke have 70 percent more respiratory problems and middle-ear infections than children of nonsmokers. Studies show that asthmatic children’s condition is significantly likely to be worsened by ETS.14
Outdoor Air Pollution
Data suggest that over 60 percent of the diseases associated with respiratory infections are linked to exposure to air pollution.15 Outdoor pollutants such as sulfur dioxide, ozone, nitrogen oxide, carbon monoxide, and volatile organic compounds come mainly from motor vehicle exhaust, power plant emissions, open burning of solid waste, and construction and related activities. According to one report, children in cities with populations greater than 10 million are exposed to levels of air pollution two times to eight times higher than the level WHO considers acceptable.16 In Mexico City, pollution levels are well above WHO’s limits of 90 micrograms per cubic meter (µg/m3) for particulates and 50 µg/m3 for sulfur dioxide and nitrogen dioxide (see Figure 1).17
Figure 1
Pollution Levels in Selected Cities
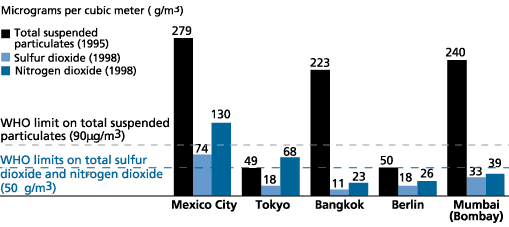
Note: WHO limits for nitrogen dioxide and sulfur dioxide are 50 µg/m3 for each type of pollutant.
Source: World Bank, World Development Indicators 2002.
Unsafe Drinking Water and Poor Sanitation
Contaminated water and inadequate sanitation cause a range of diseases, many of which are life-threatening. The most deadly are diarrheal diseases, 80 percent to 90 percent of which result from environmental factors. In 2001, diarrheal infections caused nearly 2 million deaths in children under age 5, primarily due to dehydration; many more children suffer from nonfatal diarrhea that leaves them underweight, physically stunted, vulnerable to disease, and drained of energy.18 Poor sanitation conditions and inadequate personal, household, and community hygiene are responsible for most diarrheal infections.19
Despite significant investments in improving water supplies and sanitation over the last 20 years, about 18 percent of the world’s population still lacks access to safe drinking water, and nearly 40 percent have no access to sanitation.20 At present, people in rural areas are the most affected, although continual urbanization means that increasing numbers of people live in densely populated cities, where they face shortages of potable water supplies and sanitation systems, as well as growing pollution. More than 1 billion people, mostly in Africa, Asia, and Latin America, currently live in slums or as squatters.21
Infectious Disease Vectors
Vector-borne diseases, such as malaria, represent an international public health problem, particularly in tropical areas of Africa, Asia, and Latin America. Approximately 1 million children under age 5 in sub-Saharan Africa die of malaria each year; malaria causes about 25 percent of all deaths among children in the region, especially among children living in remote rural areas with poor access to health services.22 Malaria also contributes to low birth weight, one of the leading risk factors for infant mortality, because pregnant women are more susceptible to both malaria and anemia.23
The prevalence of malaria is strongly related to environmental factors such as irrigation and other agricultural practices, land clearing, and changing demographic patterns. Higher temperatures, heavier rainfall, and other changes in climate, as well as deforestation, increase the risk of malaria and related epidemics.24
Exposure to Hazardous Chemicals
As countries pursue economic development, the increased risk of exposure to chemical hazards may worsen other risks to children’s health, such as unsafe water and poor hygiene. Industrialization and modernized agriculture have many benefits, but they have often been accompanied by problems, such as exposure to pesticides, that disproportionately affect children. Other potential toxins include lead discharged from battery-recycling operations; mercury in fish; and nitrates, arsenic, and fluoride in drinking water.
In many countries, children are exposed to toxic chemicals in the workplace. According to the International Labour Organization (ILO), more than 352 million children ages 5 to 17 engage in “economic activity,” an internationally accepted standard that includes unpaid and illegal work and work in the informal sector. Of those children, about 50 percent work in hazardous occupations or situations, defined as those “likely to have adverse effects on the health, safety, or moral development of children.”25 The ILO has classified mining, construction, manufacturing, retail, personal service, transportation, and agriculture, as well as any work where a child works more than 43 hours per week, as being hazardous.26 Hazardous labor is often informal: Some children scavenge rubbish dumps, where they may be exposed to discarded batteries, medical waste, and pesticides. In one district of Manila, for example, a government report suggests that there are nearly 14,000 child scavengers.27
Lead Exposure to lead remains the main environmental problem for young children in developing countries, according to Environmental Defense and the Alliance to End Childhood Lead Poisoning.28 Even small amounts of lead can be dangerous, especially for the development of the brain: Studies have shown that IQ falls by up to six points for every 10 micrograms of lead per deciliter of blood (µg/dl). Lead exposure can also cause anemia, kidney disease, hearing damage, and impaired fertility; at high levels, it can result in coma or death.29 Leaded gasoline accounts for 80 percent to 90 percent of airborne lead pollution in some large cities, elevating the blood lead levels of people living in the area.30 For example, Figure 2 shows that 75 percent of Indian children in high-traffic areas have blood lead levels above 10 µg/dl. Children can also be exposed to lead from food-can solder, lead-based paints, ceramic glazes, drinking water systems, and cosmetics and folk remedies. Lead can contaminate soil, air, drinking water, and food, thereby posing a significant threat to young children, whose digestive systems absorb lead at significantly higher rates than do those of adults.
Figure 2
Percentage of Indian Children With Average Blood Lead Levels Above 10 µg/dl (n = 1,477)
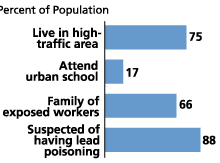
Source: The Alliance to End Childhood Lead Poisoning and Environmental Defense, The Global Dimensions of Lead Poisoning (1994).
Pesticides Pesticides, including some that have been banned in more developed countries, are widely used in less developed countries. People who come into contact with pesticides that are being applied to crops or who consume food that is carrying pesticide residues can become ill. Pesticides can also seep into the ground and contaminate drinking water.31 Although pesticides are used worldwide, some regions are particularly affected: Central America, for example, uses 1.5 kilograms of pesticides per person each year, more than any other region.32
Symptoms of pesticide poisoning in children resemble those in adults, and include eye, skin, and respiratory irritations and higher rates of long-term health problems such as cancer.33 But children are much more susceptible to these hazards, since they eat and drink more per unit of body weight, making them likely to absorb higher amounts of pesticides from food and water.34
Taking Action Against Risks
Environmental health risks to children are increasingly being recognized as an international problem. Although progress has been made in reducing mortality from environmentally mediated diseases, such as ARIs and diarrheal disease, more needs to be done to prevent these illnesses and to focus on new threats from increased industrialization, urbanization, and agricultural commercialization. Global environmental threats such as climate change may compound many of these issues, and efforts to mitigate certain hazards may create other problems. For instance, efforts to provide more drinking water in Bangladesh resulted in widespread poisoning, since the country’s well water was heavily contaminated with arsenic.35
Experience and research suggest there are a number of actions that policymakers and planners can take to address environmental health threats to children.
Encourage the development and support of community-level initiatives to reduce environmental health threats to children. In many less developed countries, municipal governments are increasingly managing local resources, especially drinking water and firewood. Community- and household-level interventions could also be adopted to reduce exposure to and transmission of ARIs, diarrheal disease, and malaria. For instance, numerous field studies have indicated that good personal and household hygiene practices can help reduce the occurrence of diarrheal disease, even when there is no access to safe water or modern sanitation.36
Continue to raise awareness and provide education about children’s environmental health issues. Since 1997, when the G-8 countries first declared their responsibility for children’s environmental health, many international, regional, and national conferences have been held, and international organizations have developed special units to address environmental health concerns affecting children. In addition, several nongovernmental organizations (NGOs), including the Children’s Environmental Health Network and the International Research and Information Network on Children’s Health, Environment, and Safety (INCHES), have been created specifically to protect children from environmental hazards and to promote a healthy environment. At the local level, efforts need to be made to teach children, families, and communities to identify environmental threats to children, to adopt practices that reduce risks of exposure, and to work with local authorities and the private sector to develop prevention and intervention programs.
Promote the recognition, assessment, and study of environmental factors that affect children’s health and development. Efforts to encourage research about environmental hazards might involve establishing research centers or multidisciplinary studies; incorporating material on children’s environmental health into training for health care providers and other professionals; and promoting the collection and dissemination of harmonized data. Current multilateral efforts to advance international indicators for children’s environmental health include collaboration between Physicians for Social Responsibility, INCHES, and the U.S. Environmental Protection Agency, based on previous work by WHO and other organizations.
Reduce children’s exposure to pollutants through education, regulation, use of cleaner fuels, and reduction of environmental tobacco smoke. Strategies for reducing deaths from pneumonia and other respiratory conditions include cutting children’s exposure to smoke from air pollution, cooking stoves, and cigarettes. Some national governments have reduced indoor pollution by promoting safer, more efficient, more durable cook stoves.37 International health experts recommend a combination of educational programs and legislative interventions to halt tobacco use in settings frequented by children.38 Regulations on air pollution need to be enforced in cities, and include phasing out leaded gasoline, reducing emissions from coal-fired plants, and replacing fossil fuels with cleaner energy sources.
Invest in programs to increase access to clean water and sanitation facilities and to promote better hygiene practices. While diarrhea-related deaths between 1990 and 2000 declined by 50 percent due to oral rehydration therapy, there is little evidence that the incidence of diarrheal disease has fallen.39 Efforts to combat diarrhea include combining appropriate drug therapy with optimal breastfeeding practices, improving nutrition, increasing access to clean water and sanitation facilities, and improving personal and domestic hygiene.40 Several studies have shown that improving water and sanitation can reduce the number of diarrheal episodes by between 20 percent and 26 percent.41 Furthermore, better hygiene practices, such as washing hands regularly, can reduce the number of diarrhea cases by up to 35 percent.42
Strengthen interventions to prevent and treat malaria. While progress has been made in reducing ARIs and diarrheal disease, deaths from malaria have increased in the past 10 years, due in part to global climate change and in part to the emergence of antibiotic-resistant strains of the disease. Environmental improvements such as proper irrigation and drainage techniques, combined with the use of insecticide-treated bed nets and adequate medical treatment, could greatly reduce malaria’s spread. Several international initiatives, such as the Roll Back Malaria (RBM) partnership, have also been instrumental in addressing the problem. RBM seeks to halve the global incidence of malaria by 2010, and focuses on early diagnosis and prompt treatment; vector control and use of insecticide-treated bed nets; malaria treatment for pregnant women; and prevention of and response to epidemics.
Reduce children’s exposure to lead, and screen for lead poisoning. About 50 countries worldwide, including more than 20 less developed countries, have phased out leaded gasoline.43 For instance, Thailand phased out leaded gasoline between 1984 and 1996, and Bangkok’s atmospheric lead levels have decreased markedly.44 A survey of 1,000 children between 6 months and 72 months old in Chiang Mai, another Thai city, revealed that only 4.6 percent of the children had blood lead levels exceeding 10 µg/dl.45 Nevertheless, almost 100 countries (including countries in eastern Europe, the Middle East, and Africa) still use leaded gasoline, and few countries have identified and addressed other sources of lead in the environment.46
Efforts to phase out leaded gasoline and to reduce or eliminate other sources of lead exposure include the Global Lead Initiative, sponsored by the Alliance to End Childhood Lead Poisoning, to develop national action plans, fund technical assistance projects, and encourage civic participation in exchanging best practices and coordinating efforts within regions.
Reduce exposure to harmful pesticides by banning the use of the most toxic chemicals, educating users, and encouraging the use of integrated pest management to minimize the use of pesticides. In order to reduce the threat from pesticide exposure, international organizations, national governments, and industry have stepped up efforts to limit the exportation of dangerous chemicals, help affected countries develop national action plans for handling and disposing of pesticides, and encourage the use of environmentally friendly alternatives. As of June 2002, more than 150 countries had signed (and 11 had ratified) the Stockholm Treaty on Persistent Organic Pollutants, which phases out or restricts the use of 12 chemicals, including nine pesticides that persist in the environment and accumulate in the food chain. The treaty will become legally binding once 50 countries have ratified it. National efforts are also being developed. Costa Rica, for example, is fostering pesticide-free, organic farming by devoting more than 9,000 hectares to organic cultivation of 30 crops.47
Evaluate and address the plight of children employed at hazardous workplaces. Children are increasingly likely to be exposed to chemicals in the places where they live, play, and work. Much attention has been paid recently to mitigating environmental and other threats to children in all of these spheres, particularly at hazardous workplaces.
As of May 2002, more than 120 countries had ratified the Convention on the Worst Forms of Child Labor, which calls for withdrawing children age 16 and younger from intolerable and hazardous work situations, by identifying hazards and developing effective monitoring systems.48
Conclusion
While overall child mortality declined by 10 percent in the 1990s, much remains to be done to protect children from the myriad environmental threats to their health. Reducing long-term threats requires that underlying risk factors be addressed. Over the past 15 years, international, regional, and national attention has focused on environmental hazards’ effect on children’s health. Efforts now need to be made to measure these risks; build and strengthen community, national, regional, and international coalitions to address the problem; and develop policies and programs to prevent and mitigate environmental hazards for children worldwide.
References
- United Nations Environment Programme (UNEP) et al., Children in the New Millennium (New York: UNEP, 2002).
- UNEP et al., Children in the New Millennium.
- Dona Schneider and Natalie Freeman, Children’s Environmental Health: Reducing Risk in a Dangerous World (Washington, DC: American Public Health Association, 2000).
- UNEP et al., Children in the New Millennium.
- UNEP et al., Children in the New Millennium.
- World Health Organization (WHO), “Danger in the Air,” accessed online at www.who.int/inf-pr-2000/3n/pr2000-56.html, on June 18, 2002; and N. Bruce et al. “Indoor Air Pollution in Developing Countries: A Major Environmental and Public Health Challenge,” Bulletin of the World Health Organization 78, no. 9 (2000): 1078-92.
- World Bank, Indoor Air Pollution Newsletter: Energy and Health for the Poor, no. 2 (December 2000); and K. Smith, “National Burden of Disease in India from Indoor Air Pollution,” Proceedings of the National Academy of Sciences of the United States of America 97, no. 24 (2000): 13286-93.
- WHO, Health and Environment in Sustainable Development: Five Years After the Earth Summit (Geneva: WHO, 1997): 87; and Kirk Smith et al., “Indoor Air Pollution in Developing Countries and Acute Lower Respiratory Infections in Children,” Thorax 55, no. 6 (2000): 518-32.
- Hiremagalur N.B. Gopalan and Shannon Ryan, “Urban Air Pollution Management Focusing on Children’s Health” (paper presented at the Workshop on Air Pollution in the Megacities of Asia, Seoul, South Korea, Sept. 3-5, 2001)
- Kirk R. Smith and Sumi Mehta, “The Burden of Disease From Indoor Air Pollution in Developing Countries: Comparison of Estimates” (paper presented at USAID Global Consultation: The Health Impact of Indoor Air Pollution and Household Energy in Developing Countries: Setting the Agenda for Action, Summary Report for Participants, Washington, DC, May 3-4, 2000).
- WHO, “Bronchial Asthma: Fact Sheet,” accessed online at www.who.int/inf-fs/en-fact206.html, on June 12, 2002.
- Schneider and Freeman, Children’s Environmental Health.
- WHO, “Bronchial Asthma: Fact Sheet.”
- International Consultation on Environmental Tobacco Smoke and Child Health, “Consulation Report,” WHO/NCD/TFI/99.10 (Geneva: WHO, 1999).
- Kirk R. Smith et al., “How Much Global Ill Health Is Attributable to Environmental Factors?” Epidemiology 10, no. 5 (1999): 573-84.
- Devra Davis and Paulo H.N. Saldiva, Urban Air Pollution Risks to Children: A Global Environmental Health Indicator (Washington, DC: World Resources Institute, 1999).
- United Nations Population Division, “World Urbanization Prospects: The 1999 Revision,” accessed online at www.un.org/esa/population/
publications/wup2001/wup2001dh.pdf, on June 12, 2002. - UNICEF et al., “Global Water Supply and Sanitation Assessment: 2000 Data,” accessed online at www.childinfo.org/eddb/water.htm, on June 12, 2002.
- WHO, Health and Environment in Sustainable Development.
- UNICEF et al., “Global Water Supply and Sanitation Assessment: 2000 Data.”
- United Nations Human Settlements Programme, “The State of the World’s Cities, 2001” (Nairobi, Kenya: United Nations, 2001).
- H. Gelband and S. Stansfield, “The Evidence Base for Interventions to Reduce Under-Five Mortality in Low- and Middle-Income Countries,” CMH Working Paper Series, no. WG5:9 (Geneva: WHO Commission on Macroeconomics and Health, 2001).
- UNICEF, “Malaria Statistics,” accessed online at www.childinfo.org/
eddb/Malaria/index.htm, on March 18, 2002. - Gurinder S. Shahi et al., International Perspectives on Environment, Development, and Health: Toward a Sustainable World (New York: Springer Publishing Company, 1997).
- International Programme on the Elimination of Child Labour and the Statistical Information and Monitoring Programme on Child Labour, Every Child Counts: New Global Estimates on Child Labour (Geneva: International Labour Office, 2002).
- International Programme on the Elimination of Child Labour and the Statistical Information and Monitoring Programme on Child Labour, Every Child Counts.
- Environmental News Service, “Children Bear the Heaviest Burden of Environmental Disease,” accessed online at www.who.int/peh/
ceh/articles/burden.htm, on June 19, 2002. - The Alliance to End Childhood Lead Poisoning (AECLP) and Environmental Defense (ED), Global Dimensions of Lead Poisoning: An Initial Analysis (Washington, DC: AECLP and ED, 1994).
- Yasmin E. Von Schirnding and Richard F. Fuggle, “A Study of the Distribution of Urban Environmental Lead Levels in Cape Town, South Africa,” Science of the Total Environment 188, no. 1 (1996): 1-8.
- Helen Gavaghan, “Lead, Unsafe at Any Level,” Bulletin of the World Health Organization 80, no. 1 (2002): 82.
- U.S. Environmental Protection Agency, “Assessing Health Risks from Pesticides,” accessed online at www.epa.gov/pesticides/
citizens/riskassess.htm, on June 13, 2002. - César Chelala, “Environmental Impact on Child Health” (Washington, DC: Pan American Health Organization, 2000).
- James Weeks et al., eds., Preventing Occupational Disease and Injury (Washington, DC: American Public Health Association, 1991).
- U.S. Environmental Protection Agency, “Pesticides and Food: Why Children May Be Especially Sensitive to Pesticides,” accessed online at www.epa.gov/pesticides/food/pest.htm, on June 13, 2002.
- Allan Smith et al., “Contamination of Drinking Water by Arsenic in Bangladesh: A Public Health Emergency,” Bulletin of the World Health Organization 78, no. 9 (2000): 1093-103.
- Massee Bateman and Chris McGahey, “A Framework for Action: Child Diarrhea Prevention,” accessed online at www.ehproject.org/Pubs/
GlobalHealth/GlobalHealthArticle.htm, on June 17, 2002. - World Bank, Indoor Air Pollution: Energy and Health for the Poor 1, accessed online at http://lnweb18.worldbank.org/ sar/sa.nsf, on June 13, 2002.
- Tobacco Free Initiative, “Consultation Report,” accessed online at www.ash.org.uk/html/passive/html/who-ets.html, on June 13, 2002.
- Gordon McGranahan et al., Environmental Change and Human Health in Countries of Africa, the Caribbean and the Pacific (Stockholm: Stockholm Environment Institute, 1999).
- Patricia Billig and Diane Bendahmane, “Diarrhea Prevention: Lessons Learned,” accessed online at www.ehproject.org/PDF/
Lessons_Learned/diarrhea_prevention.pdf, on June 19, 2002. - Stephen A. Esrey et al., “Interventions for the Control of Diarrheal Diseases Among Young Children: Improving Water Supplies and Excreta Disposal Facilities,” Bulletin of the World Health Organization 63, no. 4 (1985): 757-72; Stephen A. Esrey et al., “Effects of Improved Water Supply and Sanitation on Ascariasis, Diarrhea, Dracunculiasis, Hookworm Infection, Schistosomiasis, and Trachoma,” Bulletin of the World Health Organization 69, no. 5 (1991): 609-21; and Sharon R.A. Huttly et al., “Prevention of Diarrhea in Young Children in Developing Countries,” Bulletin of the World Health Organization 75, no. 2 (1997): 163-74.
- Huttly et al., “Prevention of Diarrhea in Young Children in Developing Countries.”
- AECLP, “Launching a Global Lead Initiative: A Proposal to the World Summit on Sustainable Development” (draft, Washington, DC: AECLP, 2002).
- Naree Boontherawara et al. “Traffic Crisis and Air Pollution in Bangkok,” Thailand Environment Institute Quarterly Environment Journal 4, no. 2 (1994): 4-36.
- Tippawan Prapamontol et al., “Lead Screening in Young Children From Northern Thailand” (Chiang Mai, Thailand: Chiang Mai University,

 ">
">
 ">
">