
Disability and Aging
(August 2007) The rates of old-age disability have declined in recent decades, and it is expected that Americans will live longer before disability sets in than is true today. The reasons for the decline in disability are complex, and the promising trend could be countered by the rise in obesity.
As the accompanying chart shows, four fifths of 10 elderly Americans were not chronically disabled in 2004-2005, measured by their state of health and the daily tasks they are able to do. That is an improvement over three-quarters a decade earlier.
A similar trend has been documented in some Europe countries. Denmark, Finland, Italy, and the Netherlands show clear evidence of a decline in disability among the elderly.
The Prevalence of Disability in the Elderly Population Has Been Decreasing.
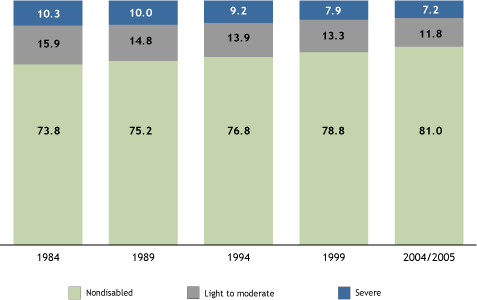
Source: K.G. Manton, X. Gu, and V. Lamb, “Change in Chronic Disability From 1982 to 2004/2005 as Measured by Long-Term Changes in Function and Health in the Elderly Population,” PNAS 103, no. 48 (2006): 18734-9.
Why Has Disability Decreased While Chronic Disease Increased?
This decrease in old-age disability has come as chronic diseases such as heart disease and diabetes have increased, a seemingly contradictory trend. But disability is determined by other factors in addition to health. As life expectancy in the older population has increased, more elderly people are living with chronic illnesses. However, these illnesses are not as disabling as they were in the past.
Assistive technologies (such as wheelchairs or hearing aids) have enabled many older people to stay active or enhance their physical abilities. In one study of older people living in the community, assistive technologies accounted for half of the decline in the number of people relying on personal care.
In the past, rising education levels have also contributed to recent improvements in old-age disability. Well-educated people tend to have greater income and savings, which buy better health care. People with more education also are less likely to engage in risky behaviors, or to work at jobs that produce stress and create other health risks. Education also helps postpone some types of mental deterioration.
According to Vicki Freedman at the School of Public Health in the University of Medicine and Dentistry of New Jersey, new evidence suggests that in the United States, rising education may no longer contribute to declines in disability rates. In the last decade, increases in the proportion of elderly with 12 years of education or more have not been associated with a corresponding decline in disability rates because the disadvantage of not having a college education has grown. Disability rates for those without a college degree continue to be much higher than disability among college graduates.
Improvements in mental abilities also can be linked to improved medical treatments. Recent declines in stroke rates and medical advances in treatment of stroke victims have contributed to a decline in the proportion of people with certain types of cognitive impairment (other than Alzheimer’s) since 1982.
Obesity Could Fuel Disability Increase Among Baby Boomers
There is concern that rising obesity in the United States could halt or reverse the decline in old-age disability, because older, obese people have more chronic illnesses, more limited activity and higher health care costs. Already there is evidence that Americans in their early 50s are less healthy than people of the same age a decade earlier.
Baby boomers ages 51 to 56 report being in poorer health, have more difficulty with daily tasks, and report more pain, chronic conditions, and psychiatric problems, according to some research. Based on current trends for people ages 50 to 69, disability rates could increase during the next decade from 8 percent in 2005 to 9 percent in 2015, reversing some or all of the recent gains.
Another potential red flag is that although all groups have improved disability rates, there remains a gap between affluent, well-educated Americans and those with less income and education. People with lower incomes and education also are more likely to be disabled during their last years of life.
These research findings have important implications for future cohorts of elderly Americans, who are projected to be more racially and ethnically diverse. Because Africans Americans and Hispanics tend to have less education and lower incomes than non-Hispanic whites, the disability rate disparity is expected to persist, and the decline in disability is expected to slow.
Impact of Disability Trends on Government Spending
The Census Bureau projects that by 2030, there will be 71 million people age 65 or older. The oldest baby boomers will start to turn 65 in 2011.
Research funded by the National Institute on Aging suggests that recent declines in disability rates at older ages are unlikely to produce significant cost savings for Medicare. The Medicare-eligible population will increase rapidly as baby boomers reach retirement age. That and the obesity epidemic are expected to contribute to a rise in Medicare expenses.
Although these trends point to potential fiscal problems for health and retirement systems, a more optimistic scenario is possible. The Bureau of Labor Statistics in 2006 projected increased labor force participation among people age 55 and older. Baby boomers could retire at later ages and use fewer health benefits compared with the current generation of elderly.
Some researchers project that further declines in disability rates will compress the demand for long-term care among the “oldest old” and boost productivity of the “young old,” those ages 65 to 84. They argue that current Medicare and Medicaid benefits should be preserved or even increased in order to accelerate health improvements in old age and to promote the trend of delayed retirement.
D’Vera Cohn is senior editor at the Population Reference Bureau. Mark Mather is deputy director of domestic programs at PRB. Marlene Lee is a senior policy analyst at PRB.
