
Ensuring Skilled Attendants at Birth in Rural Ghana
Evelyn Sakeah is a Ph.D. student in public health at Boston University. She is a participant in PRB’s 2012-2013 Policy Communication Fellows Program, funded by USAID through the IDEA project. This article was written as part of the Fellows Program.
While Ghana has made significant improvements in reducing the number of women who die from pregnancy-related complications, many women still needlessly die each year from these preventable problems.
In just one year (2010), approximately 2,700 women in Ghana died from pregnancy-related complications, and most of these deaths occurred in the period from late pregnancy through 48 hours after delivery. And the rural-urban differences in Ghana are stark: In 2008, only 43 percent of rural women had skilled attendants at their birth, while 84 percent of births to urban women were attended by skilled health personnel.1
Experts agree that access to skilled attendants at birth (doctors, nurses, midwives) is one way to decrease maternal deaths, and this access should be available to women in rural areas as well as urban areas.2 Since 2000, the government of Ghana has had an innovative program to improve maternal health, especially in rural areas, and the results are encouraging.
Reaching Rural Women
Many studies show that placing a midwife in a village could promote skilled attendants at birth in rural areas.3 For example, the Kenya Ministry of Health has collaborated with the United States Agency for International Development (USAID) and the Population Council’s Frontiers in Reproductive Health to scale up a Community-Based Midwifery program that enabled women to give birth at home safely or be referred to a hospital. The ministry employed and trained committed retired or unemployed midwives living in rural areas to assist women during pregnancy and childbirth and to provide postnatal care in their homes to manage minor complications and to aid prompt referral to hospitals if needed. These midwives contributed to increasing the proportion of women assisted by skilled attendants in four districts of the Western Province of Kenya.4
Ghana’s Community-Based Program to Improve Maternal Health
Ghana’s Community-Based Health Planning and Services (CHPS) program was established in 2000 to improve access and quality of health care and family planning services throughout the country.5 In most of the country, CHPS has not focused specifically on improving skilled deliveries, but in the Upper East Region, the Ghana Health Service piloted a new approach to addressing maternal mortality. Community health officer midwives (CHO-midwives) were trained and sent to CHPS compounds in the Upper East Region to offer integrated health services that include maternity care to rural women. The CHO-midwives are partnered with traditional birth attendants and other community members to provide skilled delivery services.
In 2012, as part of my doctoral research, I worked with the Ghana Health Service to evaluate this pilot program, conducting household surveys as well as key stakeholder interviews. The results of this research show that, in rural communities of the Upper East region, community members saw a huge and positive difference in delivery care. Women are now more likely to deliver safely.
Percentage of Female Respondents by Place of Delivery of Last Child, Kassena-Nankana East, Kassena-Nankana West, and Bongo Districts of the Upper East Region, Ghana, 2012
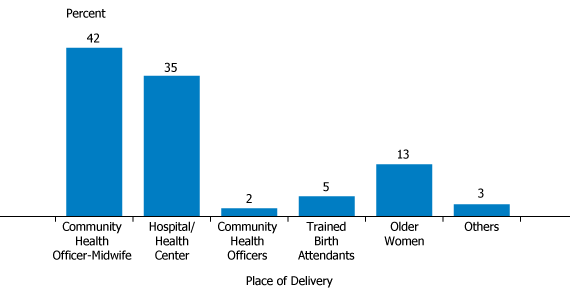
Source: Evelyn Sakeah, “Utilizing the Community-Based Health Planning and Services Program to Promote Skilled Attendants at Delivery in Rural Ghana,” dissertation submitted to Boston University School of Public Health in partial fulfillment of the requirements for the degree of doctor of public health, 2013.
Although some women still travel long distances to the hospitals and health centers for delivery care, more than 40 percent of women in rural communities sought skilled delivery care from CHO-midwives in the past three years (see figure). The most exciting news is that nearly 80 percent of women in CHPS zones in three districts of the Upper East Region were supervised by skilled attendants at birth in the past three years, notable progress toward achieving Millennium Development Goal 5 of increasing skilled delivery to 85 percent. One community elder expressed the sentiment that was commonly voiced about the program:
“…I will say that the government has done well by sending trained midwives to the communities to provide skilled delivery care. I am no more worried when pregnant women go to deliver because they will come back safely. We are thankful to the health authorities.” (Elder, Kassena-Nankana West District)
The Ghana Health Service also has trained traditional birth attendants to increase safe delivery care in rural areas, and to refer clients to skilled professionals if needed.6 Traditional birth attendants collaborate with CHO-midwives to provide skilled delivery services to women. Results from the program indicate that traditional birth attendants often refer or accompany their clients to CHPS compounds for skilled care. These findings are consistent with results from a previous study that found that this kind of collaboration resulted in traditional birth attendants referring or accompanying many more pregnant women to health facilities for skilled delivery care.7
Counting Benefits From the Program
Community members in the Upper East Region have reported that since the program started, women now rarely die or suffer injuries related to pregnancy.
The inclusion of midwifery within the Upper East Region CHPS program demonstrates how it is possible to extend skilled delivery services to rural communities of Ghana, as well as community members’ readiness to embrace skilled delivery care should government and the health authorities make the services available and accessible to them.
The government of Ghana and the Ghana Health Service can take practical steps to scale up this effective pilot from the Upper East Region to the broader national CHPS program and include skilled delivery care to ensure the safety of women during delivery.
References
- Ghana Statistical Service, Ministry of Health, and Macro International, Ghana Demographic and Health Survey 2008 (Calverton, MD: Macro International, 2008).
- WHO, UNICEF, UNFPA, and the World Bank, Trends in Maternal Mortality: 1990 to 2008 (Geneva: WHO, 2012).
- Jeremy Shiffman, “Generating Political Will for Safe-Motherhood in Indonesia,” Social Science and Medicine 56, no. 6 (2003): 1197-1207; and Frank K. Nyonator et al., “The Ghana Community-Based Health Planning and Service Initiative for Scaling Up Service Delivery Innovation,” Health Policy and Planning 20, no. 1 (2005): 25-34.
- Annie Mwangi and Charlotte Warren, Taking Critical Services to the Home: Scaling-Up Home-Based Maternal and Postnatal Care, Including Family Planning, Through Community Midwifery in Kenya (New York: Population Council, Frontiers in Reproductive Health, 2009).
- Nyonator et al., “The Ghana Community-Based Health Planning and Service Initiative for Scaling Up Service Delivery Innovation.”
- World Health Organization, Making Pregnancy Safer, A Joint Statement by WHO ICM and FIGO (Geneva: World Health Organization, 2004).
- A. Islam and F.A. Malik, “Role of Traditional Birth Attendants in Improving Reproductive Health: Lessons From the Family Health Project, Sindh,” Journal of the Pakistan Medical Association 51, no. 6 (2001): 218-22.
