Kata Fustos
Former Intern

April 12, 2011
Former Intern
Approximately 68 percent of people infected with HIV worldwide live in sub-Saharan Africa, where the virus disproportionately affects women. Gender-based violence has been identified as a significant driver of HIV/AIDS infections in women in the region, and international organizations are increasingly focusing on the elimination of violence against women as key in the battle against the spread of the epidemic.1 Prevention strategies need to address the unequal power between men and women, and norms and practices that put women at a higher risk of exposure to HIV.
In the last decade, women have become the face of HIV/AIDS in sub-Saharan Africa, as 61 percent of people living with the virus in the region are female. The highest rates of HIV/AIDS infections among 15-to-49-year-old women occur in southern Africa, particularly in Botswana, Lesotho, Swaziland, and South Africa. Figure 1 shows the differences in HIV prevalence rates between men and women in these countries, with women consistently infected in higher proportions than men. The gender gap is even more substantial among the younger age groups: In South Africa, the prevalence of HIV among young women ages 20 to 24 is approximately three times higher—21 percent compared with 7 percent—than among men of the same age. In Lesotho, around 8 percent of young women ages 15 to 19 are infected with HIV, while the prevalence rate is 3 percent among men in the same age group.2 These numbers indicate certain factors that increase women’s exposure to the virus.
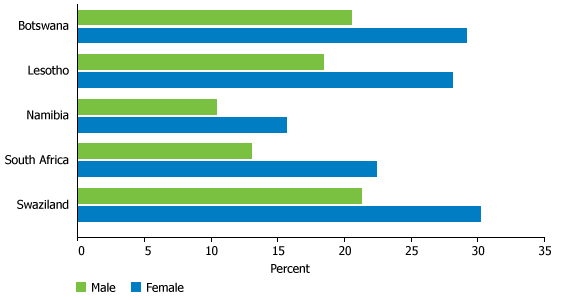 Source: Population Reference Bureau, The World’s Women and Girls 2011 Data Sheet (Washington, DC: Population Reference Bureau, 2011).
Source: Population Reference Bureau, The World’s Women and Girls 2011 Data Sheet (Washington, DC: Population Reference Bureau, 2011).
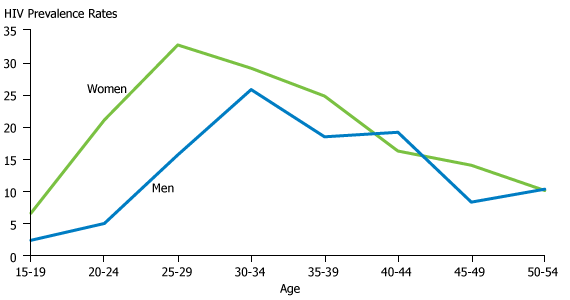
According to UNAIDS, women who have experienced violence are up to three times more likely to be infected with HIV than those who have not.3 Country statistics compiled by the United Nations show that younger women in Africa are more likely to experience physical or sexual violence than older women, generally from an intimate partner. Although exposure to violence for women varies by country and region, surveys consistently show that it peaks between ages 20 and 30, and then starts to decline. HIV prevalence also tends to reach a peak around age 25 among women. On the other hand, peak HIV prevalence among men occurs about five to 10 years later and at lower overall levels.4 Figure 2 shows the HIV prevalence rates among men and women in South Africa.
Violence increases the risk of HIV infection in women as a result of physiological and psychological reasons. Uninfected women are about twice as likely to contract HIV from infected men as vice versa.5 Biologically, women are more vulnerable to infection and forced sex further increases the risk of HIV transmission to women due to tears and lacerations, especially in adolescent girls. However, even the threat of violence can have serious negative consequences. Women fearing violence are less able to protect themselves from infection: They do not have the power to negotiate for safe sex or to refuse unwanted sex, they do not get tested for HIV, and they fail to seek treatment after infection. A 2005 survey found that about 60 percent of HIV-positive women chose not to receive treatment at a Zambian clinic because they feared violent behavior and abandonment by their family.6 Women report fearing discrimination, physical violence, and rejection by their family if they disclose their HIV-positive status. In a study on sexual violence and HIV in South Africa, 16 percent of males and 14 percent of females in the 15-to-19-year-old age group would not share a positive diagnosis with their family.7 Teenagers who had been forced to have sex in the past year were even more likely to hide their HIV-positive status.
Community acceptance of norms of masculine behavior and men’s use of power over women promotes power inequality between the genders, which can lead to violence. Several forms of male dominance, while supported in greater numbers by men, are also widely accepted by women. For example, the South African HIV and sexual violence study observed that, among 15-to-19-year-olds, 28 percent of males and 27 percent of females believed that a girl did not have the right to refuse sex with her boyfriend. And, 55 percent of males and 54 percent of females thought that “sexual violence does not include forcing sex with someone you know.”8 Furthermore, 15 percent of 19-year-old females and 12 percent of males in the study reported being forced to have sex in the past year before the survey.
In addition, the unequal power dimension is distorted further by large age differences in relationships. It is common for women in sub-Saharan Africa to marry at a young age or have older intimate partners who are sexually more experienced. Older men are also more likely to have been exposed to HIV/AIDS and more likely to infect their younger female partner, especially if women feel like they cannot negotiate for safe sex because of unequal power in the relationship. A study in Zambia found that only 11 percent of married women believed they had the right to ask their husband to use a condom, even if they knew he was infected with HIV. Less than 25 percent believed they had a right to refuse to have sex with him.9 In Lesotho, about 37 percent of married women believed that a man was justified in beating his wife if the woman argued with him. Twenty-three percent agreed that a beating was justified if a wife refused to have sex with her husband.10
Addressing violence against women and girls in the fight against HIV/AIDS is particularly difficult as most intervention strategies focus on the more traditional ways of containing the epidemic, such as condom use, antiretroviral drugs, and treatment for STIs.11 Nevertheless, long-term prevention programs need to address underlying social issues in addition to changing public policy. The Stepping Stones training program has been described as an example of a highly successful “life-skills” package that addresses issues related to gender, HIV, communication, and relationships in a community.12 It offers a model for “lasting and measurable change in gender-related attitudes and behaviors.”13 The program brings men and women together to discuss and analyze how certain factors in their own community make them vulnerable to HIV. In groups, often based on gender and age, they talk about the issues they face and develop strategies for overcoming them. Then, the groups come together and present the kinds of changes they would like to see. The potential for long-term change rests in this intergenerational dialogue, which can uncover and challenge negative social norms.
