
Global Burden of Noncommunicable Diseases
Noncommunicable diseases (NCDs), also referred to as chronic diseases, are the leading causes of death worldwide. In 2008, 80 percent of NCD deaths were in developing countries, up from 40 percent in 1990.1 NCDs will steadily increase the number of healthy years (or disability-adjusted life years—DALYs) lost in middle-income countries, but the loss will increase very quickly in low-income countries. By 2030, low-income countries will have eight times more deaths attributed to NCDs than high-income countries.2
NCDs Account for a Growing Share of Total Deaths, Especially in Developing Regions
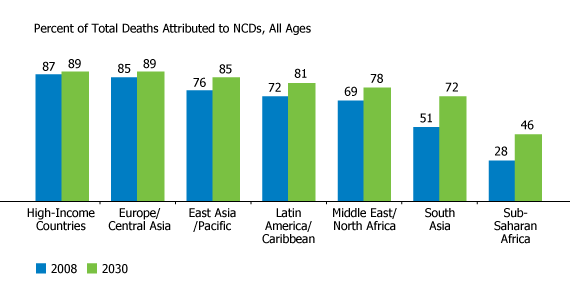
Source: Irina A. Nikolic, Anderson E. Stanciole, and Mikhail Zaydman, “Chronic Emergency: Why NCDs Matter,” World Bank Health, Nutrition and Population Discussion Paper (2011).
Alarmingly, NCD-related mortality is occurring at earlier ages in developing countries: 29 percent of NCD-related deaths in developing countries occur before age 60, compared with 13 percent in developed countries. For example, the average age of the first-time heart attack sufferer in South Asia is 53, six years younger than the world average.3 NCDs are now affecting more people who are in their prime economically productive years, and these deaths are frequently preceded by years of disability.
Four diseases, cardiovascular diseases, cancers, diabetes, and chronic respiratory diseases, are responsible for the majority of NCD-related illness and death. These four, along with mental illness, will cost the developing world $21 trillion over the next two decades.4 The international community has begun to pay closer attention to the enormity of the human and financial burden of chronic disease, especially after a 2011 high-level meeting on NCDs at the United Nations.
NCDs share four main behavioral risk factors, all of which will likely escalate in developing countries: tobacco use, harmful use of alcohol, insufficient physical activity, and unhealthy diet/obesity. According to the World Bank, more than half of the NCD burden could be avoided through health promotion and prevention initiatives.5 Relying solely on treatment options to combat NCDs is very costly, particularly in developing countries where governments and health infrastructures are unprepared to respond to this growing problem. A focus on strengthening protective factors and earlier investment in prevention of NCDs among young people is therefore essential.
Adolescence Is the ‘Last Best Chance’
The world now has the largest cohort of young people in history—1.8 billion. And 1.5 billion of these youth live in developing countries. (As in a recent Lancet series on adolescence, “young people” refers to people between ages 10 and 24.6)
Adolescence is arguably the last best chance to build positive health habits and limit damaging ones. Adolescence is a time when the influence of peers and parents, as well as the targeted marketing of unhealthy products and lifestyles, is significant. Risk factors for NCDs—especially the use of tobacco and alcohol—are often established during adolescence.7 For example, the harmful use of alcohol is a major risk factor for premature death and disability, and for adolescents it is a risk factor with the largest impact on DALYs, accounting for 7 percent of DALYs worldwide. There is a direct relationship between harmful levels of alcohol consumption and NCDs such as cancers and cardiovascular disease. Adolescents who begin drinking earlier are more likely to become dependent on alcohol within 10 years than those who begin drinking at an older age, and they also increase their risk of road traffic accidents, unprotected sex, intentional and unintentional injuries, poor mental health, and gender-based violence.8
Insufficient physical activity and unhealthy diet can also lead to an array of negative physical changes in adolescence such as high blood pressure and overweight/obesity, which can trigger NCDs such as cardiovascular diseases, diabetes, and cancers in adulthood. Physical inactivity is on the rise, particularly among women. Obesity among women is especially high in some countries in Latin America and the Middle East. Rapid urbanization is also a driving force behind these risks, and signs of insufficient physical activity and unhealthy diet are quickly emerging in developing countries.9
NCD risk factors can be less damaging if addressed early in life, when habits are not yet well-established. Minimizing risk factors for NCDs, particularly during adolescence, offers the opportunity for better health, more years of productivity, and lower health care costs. Some risks, such as poor nutrition, begin in childhood or during pregnancy and are a clear precursor for later health problems.
Pioneering Interventions
There are countries pioneering innovative interventions to lower the likelihood of youth smoking, protect against unsafe alcohol use, and support healthy diet and physical activity. These prevention activities combine resources from a wide variety of sectors including, but not limited to, health. One example is Thailand’s inventive approach to tobacco control: A domestic health promotion foundation developed through collaboration with foreign funding agencies was able to identify locally relevant research to control tobacco use. Smoking prevalence in Thailand consequently dropped from 59 percent for males and 5 percent for females in 1991 to 40 percent for males and 2 percent for females in 2009.
Some of the most cost-effective strategies to combat tobacco use and harmful use of alcohol include raising taxes and enforcing bans on advertising especially targeted to adolescents. Public promotion of what constitutes a healthy diet and the appropriate amount of physical activity, specifically 60 minutes a day for adolescents, is important. National and local governments can do more to ensure their communities are eating healthier by encouraging clear food labels; managing food taxes and subsidies; promoting healthy eating in schools and workplaces; restricting marketing of junk food and sugary beverages to children and adolescents; and providing incentives for the food industry to prepare foods with less sodium, trans-fat, and saturated fat. Communities must also work together to promote physical activity and healthy eating habits based on cultural appropriateness, especially within schools.
References
- World Health Organization, Global Status Report on Noncommunicable Diseases 2010 (Geneva: World Health Organization, 2011).
- Irina A. Nikolic, Anderson E. Stanciole, and Mikhail Zaydman, “Chronic Emergency: Why NCDs Matter,” World Bank Health, Nutrition and Population Discussion Paper (2011).
- Michael Engelgau et al., Capitalizing on the Demographic Transition: Tackling Noncommunicable Diseases in South Asia (Washington, DC: World Bank, 2011).
- David Bloom et al., The Global Economic Burden of Noncommunicable Diseases (Geneva: World Economic Forum, 2011).
- World Bank, Growing Danger of Noncommunicable Diseases (Washington, DC: World Bank, 2011).
- George C. Patton et al., “Health of the World’s Adolescents: A Synthesis of International Comparable Data,” The Lancet 379, no. 9286 (2012): 1665-75.
- World Health Organization, Tobacco Free Initiative (Geneva: World Health Organization, 2012).
- Ralph W. Hingson, Timothy Heeren, and Michael Winter, “Age at Drinking Onset and Alcohol Dependence: Age at Onset, Duration, and Severity,” Archives of Pediatric Adolescent Medicine 160, no. 7 (2006): 739-46.
- Barry M. Popkin, Linda S. Adair, and Shu Wen Ng, “Global Nutrition Transition and the Pandemic of Obesity in Developing Countries,” Nutrition Reviews 70, no.1 (2012): 3-21.
