
Improving Child Health Through Healthy Timing and Spacing of Pregnancies in Rural Ethiopia
Yohannes Dibaba is a Ph.D. candidate in the School of Public Health, College of Health Sciences, at Addis Ababa University, Ethiopia. He is a participant in PRB’s 2012-2013 Policy Communication Fellows Program, funded by USAID through the IDEA project.
(June 2013) Many countries have made progress in achieving the United Nations Millennium Development Goal 4: to reduce child mortality by two-thirds by 2015. Ethiopia’s achievement in reducing child mortality has been remarkable, but still today, one of every 17 Ethiopian children dies before age 1.
The Ethiopian Child Survival Strategy recognizes the complex set of factors that influence child health, including high fertility and inadequate birth spacing.1 Several aspects of women’s fertility behavior also influence child health and survival, including mother’s age at the birth of her children, length of birth intervals, and the number of births a woman has already had. Family planning can improve child health and survival by preventing births to older and younger women (ages that carry increased risks to maternal health), reducing the number of births per woman, and lengthening the interval between births.
Researching Child Mortality in Ethiopia
In Ethiopia, under-5 mortality declined dramatically from 166 deaths per 1,000 live births in 2000 to 88 deaths per 1,000 births by 2011, a reduction of 47 percent in 11 years. Infant mortality also declined by 39 percent during the same period—from 97 deaths per 1,000 live births to 59 deaths.2
My research used data collected from a demographic surveillance site (DSS) in southwestern Ethiopia to examine the influences of women’s fertility behavior on infant mortality and the use of vaccination services. The study involved 1,370 mothers who had 1,382 births in the two years before the survey date (March 2012).
Infant deaths are high in the study area. Among the 1,382 children born to the women in the study, 78 died in the first year of life—an infant death rate of 56 deaths per 1,000 live births. But there are marked differences in infant deaths by residence and wealth: Infant death is more than twice as high in rural areas than in urban areas in the study (66 deaths compared to 31). Similarly, there were 75 deaths per 1,000 births among poor households compared to 37 deaths among wealthy households.
Figure 1
Infant Deaths in Ethiopia, by Mother’s Age and Fertility
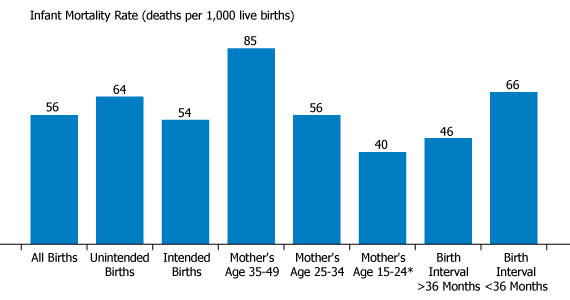
* There were fewer births to women below age 18 in the study (only 2 percent of births).
Source: Author’s research.
Older age of mother increases the chances of infant death. Infant deaths were higher when the mother’s age at birth was 35 years or older. Infant mortality was 85 per 1,000 live births for children born to women between ages 35 and 49, compared to 56 deaths per 1,000 live births among children born to women between ages 25 and 34 (see Figure 1). While the infant mortality rate was even lower among young women between ages 15 and 24, there were fewer births to women in this age group in the study population (only 2 percent of births occurred to women below age 18).
Shorter birth intervals increase the risk of infant death. Research has shown that longer birth intervals improve child survival rates, and this study observed a similar outcome. When birth intervals were shorter than 36 months, the infant mortality rate was 66 deaths per 1,000 births compared to 46 deaths when the intervals were longer than 36 months.
Fertility behavior also influences use of vaccination services. Seventy-eight percent of children ages 12 to 24 months had received at least one of the eight essential vaccination series recommended by the World Health Organization, but only 37 percent were fully vaccinated. But the percentage of children ages 12 to 24 months who received measles vaccination was 49 percent, and the vaccination rate was higher when the mother was younger (51 percent), when there are fewer children under 5 in the family, and when the pregnancy was intended (see Figure 2).
Figure 2
Measles Vaccination of Children by Women’s Fertility Behavior
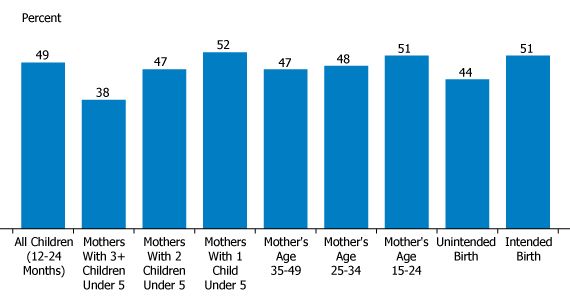
Source: Author’s research.
Healthy Timing and Spacing of Pregnancies
This study examined relationships between fertility behaviors and child health outcomes among 1,370 mothers in rural southwestern Ethiopia in 2012. Higher mortality among children is associated with shorter birth intervals, pregnancies to older women, unintended pregnancies, and a high number of births per mother. Similarly, measles vaccination coverage was lower when the mother’s age at birth was older, when the birth was unintended, and when there was more than one child under age 5 in the household. These results confirm the existing evidence of the relationship between fertility behavior and child health outcomes.
To reduce child mortality and improve child health, increased awareness in the community, particularly among women of childbearing age in rural areas, of the importance of the healthy timing and spacing of pregnancies is critical.
References
- Ethiopia Ministry of Health, National Strategy for Child Survival in Ethiopia (Addis Ababa: Central Statistical Agency and ICF International, 2005).
- Central Statistical Agency and ICF International, Ethiopia Demographic and Health Survey 2011 (Calverton, MD: ICF International, 2012).
