
Improving Safe Childbirth in India
Priyanka Dixit is a Ph.D. candidate in Population Studies at the International Institute for Population Sciences, Mumbai. She was a participant in PRB’s 2012-2013 Policy Communication Fellows Program, funded by USAID through the IDEA project. This article was written as part of the Fellows Program.
(May 2013) Despite more funding for health services during the past decade (per capita health spending rose from US$21 in 2000 to US$45 in 2009), India is unlikely to reach the targets for the health-related 2015 Millennium Development Goals (MDG).1 In particular, the government is searching for new strategies to improve maternal health and accelerate progress toward MDG 5: to improve maternal health by reducing by three-quarters the maternal mortality ratio, and achieve universal access to reproductive health.
One proven way to improve maternal and newborn health is for mothers to deliver in a health facility.2 Studies have documented that as women increase their use of maternal health care services, maternal and child deaths decrease.3 This pattern can be seen across the 15 major states of India. In states with lower rates of maternal death, the majority of mothers deliver their babies in a health facility. For example, southern states like Kerala and Tamil Nadu have more than 95 percent of deliveries in health facilities and have maternal mortality ratios of only 81 and 97 maternal deaths per 100,000 live births, respectively. On the other hand, Uttar Pradesh and Rajasthan, states from the central and northern region, have only 25 percent to 45 percent institutional delivery. In Uttar Pradesh, the maternal mortality ratio is 359; in Rajasthan, 318.
Slow Pace in the Rise of Institutional Delivery
While maternal and child health in India has improved, the level of delivery in a health facility, which is a major contributor for reducing the maternal mortality ratio, is low. At the national level, two out of five births take place at home. 4 The current estimated ratio in India is 212 maternal deaths per 100,000 live births, whereas the country’s MDG target is 109 per 100,000 live births by 2015. These 212 maternal deaths translate into about 56,000 pregnant women or new mothers dying annually, often from preventable causes.5
Antenatal Care Services Serve Two Purposes
Antenatal care (ANC) services during pregnancy serve dual functions. First, antenatal care provides a preventive service that monitors signs of pregnancy complications, detects and treats preexisting and concurrent problems, and thus lowers the risk of pregnancy complications. Second, ANC visits during pregnancy are an entry point for women into the health care system. Women who make ANC visits are exposed to health facilities and can be encouraged to continue such health care for themselves and their newborns.
There is, however, a debate on the importance of ANC visits for improving subsequent delivery in a health facility. Some studies have shown that ANC was an important factor for increasing delivery in a health facility. Others argue that a woman’s attitudes, beliefs, and motivations concerning ANC visits also lead them to seek delivery in a health facility and that ANC visits themselves do not increase the likelihood of a delivery in a health facility.6
Socioeconomic Barriers in Using ANC Services
My analysis of the India National Family Health Survey 2005-06 indicates that some measurable characteristics of women are associated with the frequency of ANC visits, and these characteristics might also affect a woman’s use of health care services. Large proportions of women from urban areas, from nonscheduled caste/tribe (groups of people who have historically enjoyed socioeconomic privilege), in the top wealth quintiles, and with high levels of education visited health centers more frequently to receive ANC compared to their counterparts. These same factors, however, would likely influence subsequent use of health services for delivery, making it difficult to isolate the role that ANC plays in increasing delivery in health facilities.
Research Findings
To study the impact of ANC visits on delivery in a health facility, I used NFHS 2005-06 data to create two groups of women matched in characteristics such as education, income level, residence, and caste. Matching two groups in this way helps control for measurable factors such as education, as well as some unmeasurable factors like a woman’s inherent attitudes, beliefs, and motivations. Thus, the difference between the two groups was in their use of ANC, and we were able to isolate the effect of ANC visits on the likelihood of subsequent delivery in a health facility.
The study was based on 7,219 mothers who did not make any ANC visits, 7,641 mothers who made one to two ANC visits, and 21,990 mothers who received more than two antenatal care visits for their youngest child.
Results showed that, among women who did not make any ANC visits, only 11 percent delivered in a health facility. Among women who received one to two ANC visits, only 24 percent delivered in a health facility. However, women who received three or more ANC visits were far more likely to have delivered in a health facility, 68 percent (see figure). Because we were comparing women who were otherwise similar, these results show that visiting health centers for ANC does have a positive effect on subsequent delivery in a health facility.
Percent Delivery in a Health Facility by Number of ANC Visits, 2005-06
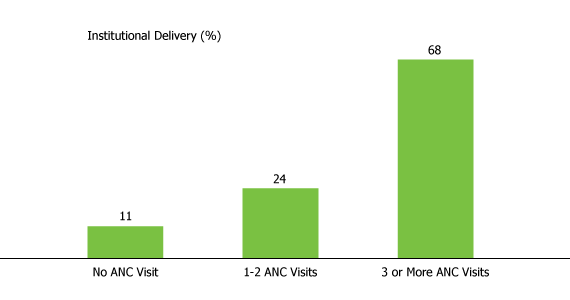
Sources: International Institute for Population Sciences (IIPS), National Family Health Survey (MCH and Family Planning), India 1992–93 (Bombay: IIPS, 1995), accessed on June 27, 2009; IIPS and ORC Macro, National Family Health Survey, 1998-99 (Mumbai: IIPS, 2000); and IIPS and ORC Macro, National Family Health Survey, 2007-08 (Mumbai: IIPS, 2007).
Continued efforts to improve maternal health in India and make progress toward MDG 5 should include ANC as a strategy to improve maternal health.
References
- United Nations, The Millennium Development Goals Report (New York: UN, 2010).
- Stephen S. Lim et al., “A Conditional Cash Transfer Program to Increase Births in Health Facilities: An Impact Evaluation,” Lancet 375, no. 9730 (2010): 2009-23; and Christiana R. Titaley, Michael J. Dibley, and Christine L. Roberts, “Type of Delivery Attendant, Place of Delivery and Risk of Early Neonatal Mortality: Analyses of the 1994–2007 Indonesia Demographic and Health Surveys,” Health Policy and Planning (2011), PMID: 21810892.
- Marjorie Koblinsky, Oona Campbell, and J. Heichelheim, “Organizing Delivery Care—What Works for Safe Motherhood?” Bulletin of World Health Organization 77, no. 5 (1999): 399-406; Wendy J. Graham, Jacqueline S. Bell, and Colin H.W. Bullough, “Can Skilled Attendance at Delivery Reduce Maternal Mortality in Developing Countries?” Studies in Health Services Organization and Policy 17 (2000): 97-130; and Lynn P. Freedman et al., “Practical Lessons From Global Safe Motherhood Initiatives: Time for a New Focus on Implementation,” Lancet 370, no. 9595 (2007): 1383–91.
- International Institute for Population Sciences (IIPS), National Family Health Survey (MCH and Family Planning), India 1992–93 (Bombay: IIPS, 1995), accessed on June 27, 2009; IIPS and ORC Macro, National Family Health Survey, 1998-99 (Mumbai: IIPS, 2000); and IIPS and ORC Macro, National Family Health Survey, 2007-08 (Mumbai: IIPS, 2007).
- India, Office of Registrar General, Sample Registration System, maternal and child mortality, and total fertility rates (2011).
- Vinod Mishra and Robert D. Retherfort, “The Effect of Antenatal Care on Professional Assistance at Delivery in Rural India,” Demographic and Health Research Working Paper 26 (2006).
