
Obesity Creeping Up on Less Developed Countries
(October 2005) In the developed world, obesity is an object of everyday conversation and mounting public concern. But a silent epidemic of obesity-related diseases—among them, cardiovascular diseases, stroke, and Type-2 diabetes—is also spreading rapidly across poor and middle-income countries, where such illnesses have been overshadowed by infectious diseases and undernutrition.1
Put simply, obesity is no longer just a rich person’s problem:
- One in every six people worldwide is already obese or overweight—and it is not uncommon even in sub-Saharan Africa to find overweight adults in the same households with underweight children.2
- About 80 percent of all cases of cardiovascular disease now occur in less developed countries, with 17 percent of deaths in poor countries in 2000 attributed to nutrition-related heart disease.3 Countries with per capita GDP that are well under $5,000—such as Pakistan and Nigeria—annually face significant risks from obesity and high cholesterol leading to heart disease.4
- And the total number of obese or overweight people is projected to grow by 50 percent in the next 10 years, primarily in poor countries. (The figure below shows the increases in rates of overweight people between 2002 and 2010 for selected countries representing a range of income levels.)
These developments promise to widen the health disparities between rich and poor and further burden already overwhelmed health care systems in the developing world. “Poor people and poor countries are the most vulnerable victims of the emerging epidemic of noncommunicable diseases related to obesity,” says Dr. Srinath Reddy, director of cardiology for the All India Institute of Medical Sciences in New Delhi.
Percent of Population That Is Overweight, Selected Countries,
2002 and 2010 (Projected)
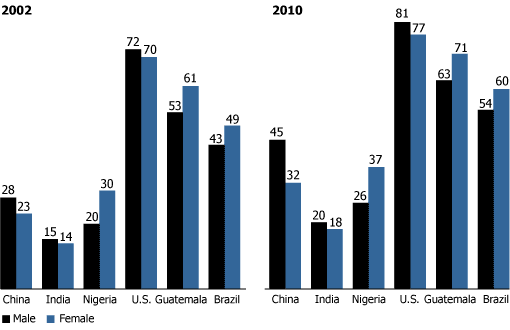
Note: “Overweight” is defined as having a Body Mass Index (weight in kilograms divided by height in meters squared) of between 25 and 30. “Obese” is defined as having a Body Mass Index of 30 or more.
Source: World Health Organization, “WHO Global InfoBase Online,” accessed at www.who.int, on Oct. 20, 2005.
Why Are Increasing Numbers in Poor Countries Becoming Obese?
The rise in obesity and related diseases in less developed countries can be traced in large part to the rapid nutrition transition in these countries—the shift from a diet of simple and sometimes traditional foods with little variation to a diet more reliant on processed foods, animal-source foods, fat, and sugar.5 This shift has been facilitated by the increasing internationalization and commercialization of the food trade.
The nutritional transition poses new challenges to nutritionists and public health experts who have spent decades battling undernutrition in poor countries. Instead of needing food programs that supplement food intake, developing countries need to provide education about overnutrition and how to limit food intake. And this need extends to all socioeconomic groups: From 1975 to 1997 in Brazil, for instance, obesity and overweight increased more among the poorest quartile of women than among the wealthiest quartile.6
Other changes—such as urbanization, reduced manual labor, and more motorization of transportation—have also contributed to higher obesity rates by lessening physical activity and thereby reducing calorie needs. But while all of these trends mimic similar progressions in developed countries at the turn of the 20th century, their development has been radically accelerated in less developed countries. For example, the death rate in India from cardiovascular disease among people between ages 35 and 65 now exceeds the rate for the United States before the 1950s, when aggressive treatment and prevention campaigns began.7
A Heavy Burden on Health Systems
The potential cost from obesity and overweight populations to poor countries is enormous. Health systems in less developed countries are not well equipped to treat large numbers of people suffering from noncommunicable diseases (NCDs) such as cardiovascular disease and diabetes.8
Many poor countries also find their health budgets already stretched thin as they try to address primary health care needs and infectious diseases. Thus, stressing medical interventions to treat obesity and its consequences will not be practical for most less-developed countries.
Public health interventions to prevent obesity might be a better bet. Recommendations do abound—making cities pedestrian-friendly, reducing salt and switching to unsaturated fats in food manufacturing, and banning advertising to children of sugared food and drinks.9 But such interventions have not yet been implemented widely or evaluated, and it will be challenging to integrate such steps into the well-entrenched system of programs to address undernutrition in poor countries.10
However, developing countries and international organizations are beginning to respond to the rise in NCDs among poor populations. For instance, the World Health Organization’s Mega-Country Network for Health Promotion campaigns for healthy lifestyles among the 60 percent of the world population that lives in the 11 largest countries of the world—which include such developing countries as Indonesia, Pakistan, Bangladesh, and Nigeria. This network is working on solutions that involve multiple sectors, including a focus on promoting health through schools and an annual Move for Health Initiative to increase physical activity.11
Research is also beginning to suggest that obesity itself can be used to identify without medical diagnosis those most at risk for several NCDs. “Obesity can serve as a surrogate for high blood pressure, high cholesterol, and diabetes in helping to target those at high risk for cardiovascular disease without any need for blood testing ” says Dr. Tom Gaziano, a heart researcher at Brigham and Women’s Hospital at Harvard Medical School who is researching cost-effective ways to screen and treat heart patients in South Africa and India. If this research is successful at pointing the way to low-cost identification of the most at-risk patients, broad-brush solutions such as eliminating salt in all processed foods could be avoided.
Nonetheless, some population-level interventions promise a multitude of benefits to countries that are either at high or low risk of rising obesity rates. These measures include modifying agricultural systems that don’t produce a healthy food supply, rectifying urban design and transport systems that discourage walking, eliminating taxes on healthier foods and/or increasing taxes on unhealthy foods, and requiring nutrition information to be provided at school lunch counters and at restaurants.12 While such policy changes have yet to be widely implemented, any of them could help avert the impending health disaster of obesity in the developing world.
Rachel Nugent is an international development economist and director of the Population Reference Bureau’s BRIDGE program.
References
- Ahmedin Jemal et al., “Trends in the Leading Causes of Death in the United States, 1970-2002,” Journal of the American Medical Association 294, no. 10 (2005): 1255-59.
- Ganapati Mudur, “World Needs Fresh Research Priorities and New Policies to Tackle Changing Patterns of Chronic Disease,” British Medical Journal 331, no. 7517 (2005): 596b; and Benjamin Caballero, “A Nutrition Paradox—Underweight and Obesity in Less Developed Countries,” New England Journal of Medicine 352, no.15 (2005): 1514-16.
- Mudur, “World Needs Fresh Research Priorities and New Policies to Tackle Changing Patterns of Chronic Disease”; and Caballero, “A Nutrition Paradox—Underweight and Obesity in Less Developed Countries.”
- Majid Ezzati et al., “Why We Need to Rethink the Diseases of Affluence,” PloS Med 2, no. 5 (2005): e133.
- Barry Popkin et al., “Understanding the Nutrition Transition: Measuring Rapid Dietary Changes in Transition Countries,” Public Health Nutrition 5, no. 6 (2002): 947-53.
- C. Monteiro et al., “Obesity and Inequities in Health in the Developing World,” International Journal of Obesity and Related Metabolic Disorders 28, no. 9 (2004): 1181-86.
- Stephen Leeder et al, “A Race Against Time: The Challenge of Cardiovascular Disease in the Developing World” (New York: Columbia University Earth Institute, 2005), accessed at www.earth.columbia.edu, on Oct. 18, 2005.
- Mudur, “World Needs Fresh Research Priorities and New Policies to Tackle Changing Patterns of Chronic Disease.”
- World Health Organization, “Global Strategy on Diet, Physical Activity and Health” (Geneva: WHO, 2002), accessed at www.who.int, on Oct. 18, 2005.
- Derek Yach and Robert Beaglehole, “Globalization of Risks for Chronic Diseases Demands Global Solutions,” Perspectives on Global Development and Technology 3, no. 1-2 (2003): 1-21.
- World Health Organization, “Health Promotion,” accessed at www.who.int, on Oct. 19, 2005.
- World Health Organization, “Global Strategy on Diet, Physical Activity and Health.”
