
U.S. Elder Care Is in a Fragile State
This article is the first in a two-part series on the demographic and policy dimensions of the nursing shortage in the United States.
(January 2002) Elder care in the United States is in critical condition. Over the last few years, nursing homes have become plagued with bankruptcies and stressed by understaffing, and the direct-care workers that these institutions and home-care agencies depend on have been going on strike or quitting in droves. With baby boomers approaching retirement age, the implications of this breakdown are sobering.
During the last three years, three of the nation’s four largest for-profit nursing-home chains entered Chapter 11 bankruptcy. According to Steven Dawson, president of the Paraprofessional Healthcare Institute, this situation stems from the homes’ inability to cope with changes in reimbursements from federally financed Medicare, which subsidizes long-term care. “They are beginning to climb back out of that crisis,” Dawson said, “but it’s not over yet.”
Few elderly citizens can expect Medicare or private insurance to cover the costs of their care, so it is not surprising that two out of three nursing-home residents rely on Medicaid to do the job. As a result, Medicaid, which was designed only as a safety-net program for the poor, is being stretched to the limit.
In addition to relying on Medicare and Medicaid, long-term care relies on health paraprofessionals — the direct-care workers — who typically earn poverty-level wages (see table). These people are the eyes and ears (and often the hands and legs) of elderly patients, the workers who quite literally do the heavy lifting to enable frail and often disoriented patients to get through each day (the figure below highlights the racial and ethnic composition of the direct-care workforce, compared with all service workers). Across the country, 2.1 million of these workers are employed in institutional care settings and through home-care agencies. As the baby-boom generation ages, the need for these workers, who now account for 38 percent of nursing-home employees and 50 percent of employees in home health care, will continue to expand. The U.S. Bureau of Labor Statistics recently projected a 58 percent rise in demand for home-care aides from 1998 to 2008.
Hourly Wages for Nurse Aides and Fast-Food Cooks, Selected States, 1999
| Nurse Aide | Fast-Food Cook | |
|---|---|---|
| Louisiana | $6.53 | $5.96 |
| Virginia | $7.67 | $6.26 |
| California | $8.93 | $6.86 |
| Connecticut | $11.32 | $7.14 |
| Average All States | $8.59 | $6.54 |
Source: U.S. General Accounting Office, “Nursing Workforce: Recruitment and Retention of Nurses and Nurse Aides Is a Growing Concern,” GAO-01-750T (May 17, 2001).
Racial/Ethnic Profile of Nurse Aides at Nursing Homes vs. All Service Workers
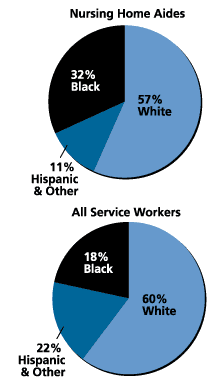
Source: U.S. General Accounting Office, “Nursing Workforce: Recruitment and Retention of Nurses and Nurse Aides Is a Growing Concern,” GAO-01-750T (May 17, 2001).
In the past, finding low-skilled, female workers to fill these jobs (86 percent of the positions today are filled by women) was easy. But the aging of baby boomers has also meant that the ratio of workers (women of prime working age, 25 to 54) to older people needing care has fallen; over the next 30 years it is projected to be cut in half. The opening up of less stressful low-wage work options during the recent “full employment economy,” coupled with that aging trend, has made direct-care workers much harder to find and even harder to keep. Providers have begun pleading with state authorities to raise the Medicaid reimbursement levels so that they can more easily raise the wages they pay.
Nursing homes’ financial and personnel difficulties have hurt the quality of care. The vast majority of nursing homes are certified by the Health Care Financing Administration (HCFA — now renamed the Centers for Medicare & Medicaid Services) so that they can qualify for Medicaid reimbursements. Among homes that are certified, each year for the past seven years up to 60 percent failed to pass the agency’s minimum health and safety standards. Labor groups and regulatory agencies alike attribute a large part of the poor quality to understaffing.
Labor Shortage or Labor Flight?
Because direct-care jobs are still generally filled by younger (under 45) women, it would seem a natural solution to recruit new workers from the ranks of post-welfare mothers. But, HCFA’s own bare-bones requirement of two weeks of pre-employment training for direct-care aides runs afoul of Congress’ 1996 welfare reform measures, whose “work first” provisions discourage pre-employment training for welfare leavers.
Moreover, the current staffing shortages, which are prevalent in professional nursing as well, outpace anything that can be explained by demographic trends alone. At nursing homes, average annual turnover of direct-care workers is very high, estimated from 40 percent to as high as 100 percent. Besides being bad news for quality care — bad for continuity, training, and morale — this instability is also expensive for providers.
Why are these employees quitting? In addition to wages that are only slightly higher than the average for fast-food workers, the General Accounting Office reports that roughly a third of all direct-care employees — whether in nursing homes or in home care — have no health coverage. These women also endure one of the highest rates of on-the-job injury in the country, one and a half times higher than that for construction workers. Steven Dawson points to disrespectful treatment as a significant cause as well. “Focus groups among these workers all show the same thing,” he said. “They complain that they’re treated as if they were invisible, at best, by nurse supervisors and other managers.”
The last few years have not brought entirely bad news for direct-care workers. Pressure from consumer and labor groups, as well as industry lobbying, has so far led 19 states to pass legislation upgrading direct-care wages through “pass-throughs” that earmark Medicaid funds for this purpose. For their part, direct-care workers and nurses alike have begun organizing in ever-larger numbers, leading a new wave of union growth and bargaining victories.
Last spring, a dramatic month-long walkout by nursing-home workers throughout Connecticut demonstrated their willingness to risk their jobs for improved state policies, although in the end it did not produce long-term changes.
Also last spring, approximately 22,000 home-care workers in Los Angeles County who work at least 112 hours per month were declared eligible to receive health and dental benefits under the county’s community health plan. This radical improvement in their status came after more than 10 years of labor negotiations.
With a recession now official, according to the National Bureau of Economic Research, it is uncertain whether that kind of success can be replicated across the country, whether by labor action or state initiative. Equally unclear is how soon federal lawmakers will be willing to enact more comprehensive changes. But it is certain that the current problems will not go away of their own accord.
Marc DeFrancis is a policy research editor and freelance writer based in Washington, D.C.
References
American Health Care Association, “The Looming Crisis: Fact Sheet on Long-Term Health Care,” accessed online at www.ahca.org, on Dec. 10, 2001.
Steven L. Dawson et al., “Direct-Care Health Workers: The Unnecessary Crisis in Long-Term Care” (New York: Paraprofessional Healthcare Institute, 2000).
Joan Fitzgerald, “Better-Paid Caregivers, Better Care,” American Prospect 12, no. 9 (May 21, 2001): 30-32.
Health Resources and Services Administration (HRSA), HRSA State Health Workforce Profiles (Washington, DC: U.S. Department of Health and Human Services, 2000).
HRSA, The Registered Nurse Population: National Sample Survey of Registered Nurses, March 2000-Preliminary Findings (Washington, DC: U.S. Department of Health and Human Services, February 2001).
Deborah Stone, “Why We Need a Care Movement,” The Nation 10, no. 270 (March 13, 2000): 13.
U.S. General Accounting Office, Health Workforce: Ensuring Adequate Supply and Distribution Remains Challenging, GAO-01-1042T (Aug. 1, 2001).
—, Nursing Workforce: Emerging Nurse Shortages Due to Multiple Factors, GAO-01-944 (July 10, 2001).
—, Nursing Workforce: Multiple Factors Create Nurse Recruitment and Retention Problems, GAO-01-912T (June 27, 2001).
—, Nursing Workforce: Recruitment and Retention of Nurses and Nurse Aides Is a Growing Concern, GAO-01-750T (May 17, 2001).
Mary Ann Wilner and A. Van Kleunen, “Who Will Care for Mother Tomorrow?” Journal of Aging and Social Policy 11, no. 2/3 (2000).
Websites
U.S. General Accounting Office
www.gao.gov
Paraprofessional Healthcare Institute
www.paraprofessional.org
National Clearinghouse on the Direct Care Workforce
www.directcareclearinghouse.org
