
The Poor-Rich Health Divide
(January 2004) Sweeping changes in public health have transformed life over the past century. On average, people live longer, healthier lives than ever before. Even so, this past century’s revolution in human health and well-being is incomplete. For people living on less than US$1 per day — and according to the World Bank there are more than 1 billion of them — health services and modern medicines are still out of reach. Moreover, many initiatives to improve the health of people in extreme poverty have been unsuccessful. A forthcoming PRB publication, “Improving the Health of the World’s Poorest People,” delves into the poor-rich health divide and what can be done to shrink it.
Health Effects of Economic Inequalities
In examining recent Demographic and Health Survey (DHS) data from more than 50 developing countries, researchers found that people in the lowest income groups fare worse than better-off groups on a range of health outcomes, including childhood mortality and nutritional status. On average, a child from the poorest of five income groupings (the poorest quintile) is twice as likely as a child in the richest quintile to die before age 5 (see Figure 1). The disparity is similar in maternal nutrition, with women in the poorest quintile twice as likely as those in the wealthiest to be malnourished.
Figure 1
Health Inequalities in Less Developed Countries
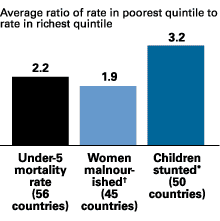
Note: Ratios are not adjusted for differences in population size across countries. Countries with indicator values <1 percent were excluded from the calculation so as not to skew the results.
*Children with a low height for age in relation to an international reference population of well-nourished children.
†In some countries, surveys measured malnutrition among women ages 15 to 49 or 15 to 44; in other countries, the surveys measured malnutrition among women with children under age 5.
Source: D. Gwatkin et al., Initial Country-Level Information About Socio-Economic Differences in Health, Nutrition, and Population, vols. I and II (Washington, DC: World Bank, November 2003).
Stunting, or chronic malnutrition among children under 5, reveals a more pronounced level of inequality. Children who are stunted are considered too short for their age compared with an international reference population; stunting is generally considered to reflect the effects of long-term malnutrition on a child’s physical growth. On average, stunting is more than three times as likely among children in the poorest quintile than in the wealthiest quintile. The inequalities in stunting are particularly large in Latin America and the Caribbean. Among the nine countries in the region included in the study — Bolivia, Brazil, Colombia, Dominican Republic, Guatemala, Haiti, Nicaragua, Paraguay, and Peru — an unweighted average of 35 percent of children in the poorest quintile were stunted, compared with 5 percent in the wealthiest quintile.
The DHS study shows that people in the poorest quintiles are less likely than those in better-off quintiles to use basic health services such as immunization, maternity care, and family planning. On average, children ages 12 months to 23 months in the wealthiest quintiles are twice as likely as those in the poorest quintiles to have received all of the basic childhood vaccinations. The World Health Organization recommends that children in this age range receive one dose each of BCG (tuberculosis) and measles, and three doses each of DPT (diphtheria, pertussis, tetanus) and polio vaccines. Among regions, inequality in immunization is especially high in sub-Saharan Africa: In the poorest quintile, only an average of 32 percent of children had been fully vaccinated, compared with 62 percent in the richest quintile.
The use of professional health care during childbirth also varies considerably. Births to women in the richest quintile are about five times more likely, on average, to be attended by a trained professional such as a doctor, nurse, or midwife (see Figure 2). Professional assistance at delivery is critical since a number of serious pregnancy-related complications cannot be predicted.
Figure 2
Inequalities in the Use of Health Services
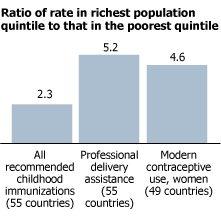
Note: Ratios are not adjusted for differences in population size across countries.
Source: D. Gwatkin et al., Initial Country-Level Information About Socio-Economic Differences in Health, Nutrition, and Population, vols. I and II (Washington, DC: World Bank, November 2003).
The level of inequality is also high for modern contraceptive use, especially in Sub-Saharan Africa. On average, married women in the wealthiest quintile are about five times more likely than those in the poorest quintile to use contraception. This may reflect disparities in access to family planning services, as well as different levels of demand for contraception. Less-educated women, for instance, tend to want larger families than better-off, more-educated women. The most extreme rich-poor differences are in some of the countries where at most 10 percent of women use modern contraception: Yemen, Chad, Mauritania, Mozambique, Niger, Nigeria, and Senegal.
Policy Responses to Health Disparities
Health systems are often unresponsive to the needs of the poor and increase their vulnerability to impoverishment. Services developed for the poor have often been of poor quality. In some cases, public spending on health — justified on equity grounds — benefits nonpoor groups more than the poor. Moreover, few countries have taken measures to track progress in reducing socioeconomic disparities in health. Instead, most state their objectives in terms of overall or average health improvements rather than how those gains are distributed.
The weight of evidence suggests that health disparities can be addressed. Even some of the poorest countries in the world have achieved substantial health gains among their most vulnerable people. Although public health has traditionally focused on improving the health of the majority, policies and programs can be reoriented, directing more benefits to poor and vulnerable groups. A number of projects have successfully mobilized community resources to secure essential drugs and trained health workers, and have established public-private partnerships to improve the quality and delivery of health services for the poor.
The research available indicates that a broad-based policy approach is the best avenue for redressing health disparities in less developed countries. In the long term, a comprehensive approach needs to influence the multiple social and economic determinants of health disparities, improving access to vital services and opportunities and reducing discrimination and isolation. The health system can also institute more immediate changes that translate into better health and quality of life for the poor.
Dara Carr is technical director for health communication at PRB.
This article is excerpted from the forthcoming PRB publication, “Improving the Health of the World’s Poorest People,” to be published in February 2004. The full text of that publication will be on PRB’s website.
