
Will Rising Childhood Obesity Decrease U.S. Life Expectancy?
(May 2005) A new study contends that rising childhood obesity rates will cut average U.S. life expectancy from birth by two to five years in the coming decades—a magnitude of decline last seen in the United States during the Great Depression.
The study, published in the March 18 issue of the New England Journal of Medicine, contradicts recent government projections that U.S. life expectancy will reach at least the mid-80s by the year 2080.1 Such forecasts, write lead author S. Jay Olshansky and his nine co-authors, are a “simple but unrealistic extrapolation of past trends in life expectancy into the future.”
In turn, other demographers have characterized the Olshansky team’s analysis as largely unsupported by evidence, and the article has spotlighted a long-standing debate about whether there are biological limits to an individual human lifespan—all amidst a recent flurry of contradictory research about how obesity effects morbidity and mortality rates. One new study from the Centers of Disease Control and Prevention (CDC) even argues that being overweight has a positive effect on life expectancy.2
But Olshansky, a professor of epidemiology and biostatistics at the University of Illinois-Chicago, remains convinced by his team’s conclusions. “If anything, we’re being conservative in our estimates,” he says. “We’re assuming no change in obesity levels from 2000 levels, and actually, they’ve gotten worse.”
Obesity and the Future of Medicine
Projecting life expectancy is more than an academic exercise. Many U.S. government agencies—including the Social Security Administration, Congress, and the military—use such forecasts to guide policymaking on issues from tax rates to the solvency of age-based entitlement programs.
And almost all these projections assume that U.S. life expectancy will continue to rise as steadily as it has since the 1930s, spurred by new medical approaches and technology as well as behavioral shifts towards healthier lifestyles. But Olshansky and his co-authors question whether medicine and public health interventions can counter the rapid increases in U.S. obesity rates over the last two decades, especially among children.
The incidence of obesity—which researchers have linked to an elevated risk of type-2 diabetes, coronary heart disease, cancer, and other health complications—rose approximately 50 percent in the United States in both the 1980s and 1990s. Two-thirds of all U.S. adults are now classified as overweight or obese, as are 20 percent to 30 percent of all children under age 15.
And Olshansky argues that this rapid rise in obesity rates will cause a “pulse event” of mortality in the United States—akin to the large number of deaths caused by an influenza pandemic or a war, but spread out over the next four or five decades.
“Any time there’s an increase in early-age mortality [deaths before age 50], it has an effect on overall life expectancy,” says Olshansky. “And when these children reach their 20s, 30s, 40s, and 50s, they’ll face a higher risk of death. It’s roughly equivalent to discovering that a large segment of our young people who never smoked suddenly decided to smoke.”
The Surprising Impact of Obesity Today
To demonstrate the future effects of rising obesity levels, Olshansky and his co-authors first calculated how current rates of adult obesity are diminishing overall U.S. life expectancy. Using studies that argue being obese reduces your life expectancy by nearly 13 years, the researchers estimated by how much overall rates of death would fall if every obese person in the United States lost enough weight to reach the optimal Body Mass Index (BMI) of 24. (Obesity is generally defined as having a BMI of 30 or above.) “In other words, to find out the effects of obesity, we statistically wiped out obesity,” says Olshansky.
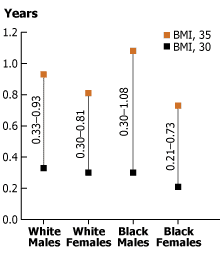
Life-Shortening Effect of Obesity According to Race and Sex in the
United States in 2000
Source: S. Jay Olshansky et al., “A Potential Decline in Life Expectancy in
the United States in the 21st Century,” New England Journal of Medicine 352, vol. 11: 1138-45.
This figure shows the potential gain in life expectancy at birth for the U.S. population in 2000, by race and sex, if obesity were eliminated. The range of estimates is shown between the bars on the basis of the assumption that everyone who is obese has a body-mass index (BMI) between 30 (lower square) and 35 (upper square) and acquires the risk of death of people with a BMI of 24.
They found that obesity now slices one-third to three-quarters of a year off overall life expectancy, depending on one’s race and gender (see figure). These figures don’t sound like much, says Olshansky, until you put them into context. “They are larger than the negative effect of all accidental deaths as well as homicides and suicides,” he says. “If you wiped out cancer, that would only add 3.5 years to overall U.S. life expectancy.”
And the effect of obesity will only grow, write Olshansky and his co-authors, as its prevalence further rises and children and young adults “carry and express obesity-related risks for more of their lifetime than previous generations have done.” Even eliminating a major disease such as cancer, they conclude, would not counter the negative consequences for life expectancy caused by this wave of deaths. “They will overwhelm the positive influences of technology,” says Olshansky.
Demographers Debate the Limits to Life Expectancy
But other demographers say the Olshansky team’s study simplifies the complex interplay of factors that have fueled 20th century gains in life expectancy in the United States and other developed countries. These analysts also characterize the study as part of a demographic paradigm—assuming a biological limit to life expectancy—that trends since 1950 have cast into doubt.
“It’s a Malthusian example of belief in the fixity of nature,” says Samuel Preston, professor of demography at the University of Pennsylvania and the author of a rejoinder to the Olshansky study in the same issue of the New England Journal of Medicine. “Their notion is that we wear out and die and there’s nothing to be done about it. The fact is that we have been very successful at postponing death at older ages, and other countries have been even more successful. It’s obvious that we should expect the life expectancy [82] that Japan has achieved.”
“Many demographers now accept that the biological maximum is not so well set,” adds Christine Himes, a sociologist at Syracuse University. “The [survival] curves are now being pushed out—more people are living past 100, and more past 110. There may be some maximum, but it’s pretty far out there, past 120.”
Preston makes three additional points in defending conventional life expectancy projections: that decreases in the rate of death at older ages in the United States have been constant since 1950, that extrapolating from past trends has provided the best forecasts, and that conventional projections have already incorporated the recent rise in obesity rates.
“We should do what we can to reduce levels of obesity,” Preston says. “But there are no long-term studies of the effect of childhood obesity on long-term mortality. And the claim this is going to offset all the factors working to increase life expectancy and result in a reduction of life expectancy is inaccurate.” Such factors, he says, might include genetic engineering, a continuing decline in the rates of infectious diseases and smoking, and changes in public behavior, such as increasing condom use among groups hit hardest by HIV/AIDS.
Olshansky, however, argues that future medical advances will principally benefit older people and only incrementally boost life expectancy. “We’ve squeezed about as much longevity per person at younger ages through science as we can,” he says. “Child obesity will influence early-age mortality, and therein lies the difference. Any time you get one of these pulse events—war, influenza, obesity, AIDS—it affects early-age mortality disproportionately.”
Others dispute the Olshansky study’s methods. “Some people have tried to forecast the future of mortality by getting best guesses for each cause and then trying to assemble them into an overall projection, but that method has never worked very well,” says Richard Suzman, associate director of behavioral and social research at the National Institute on Aging. “The mix of factors at play is too large, and there’s too much interrelation among them.”
And Himes, who studies the effects of obesity on health and functioning in later life, says the study has no empirical analysis of the specific effects of childhood obesity. “Olshansky’s approach is pretty simplistic—you can’t just extrapolate from current death rates by obesity status,” she says. “Those rates aren’t just based on obesity alone, but on other factors as well.”
The new CDC study has also raised questions about Olshansky’s conclusions. While it says that obesity killed almost 112,000 people in the United States in 2002, it also concludes that being merely overweight (having a BMI of 25-30) is associated with a lower rate of mortality than that of underweight people, especially after age 70. But Olshansky is unconvinced that obesity is less of a danger, pointing out that many recent studies point out what he calls a “startling” rise in diabetes rates.
“The CDC estimates use a different set of assumptions than we do, and they do not take into consideration the expected rise in obesity-induced deaths associated with today’s children as they grow older,” Olshansky argues. He is also perplexed that other demographers continue to defend the customary method of projecting life expectancy in the face of rising obesity rates.
“We now see children under the age of 15 who are obese at a rate of about 20 percent to 30 percent, whereas that figure was very close to zero a couple of decades ago,” he says.
Calls for a New Public Health Campaign
Olshansky, Preston, and other demographers interviews for this article do agree on one thing: Obesity is a serious and growing public-health issue that calls for a renewed public campaign. But Preston is optimistic that behavioral changes can counter America’s increasing waistlines.
“I think smoking as an addictive habit was probably harder to break than eating 30 or 100 calories a day too many,” says Preston. “The fact that we did break the back of the smoking addiction—and there was a huge campaign to do so—indicates that if we undertook a similar campaign, it might be similarly successful.”
Olshansky says he’s already undertaken such a campaign—in his own home. “One thing my generation learned is to clean our plates, to override our body’s internal mechanism that we’re full,” he says. “I’m acutely aware of that and am teaching myself and my children to stop eating when they’re full, and it’s been remarkable. I’ve lost 20 to 25 pounds in the last year.”
For More Information
S. Jay Olshansky et al. “A Potential Decline in Life Expectancy in the United States in the 21st Century,” The New England Journal of Medicine 352, no. 11 (2005): 1138-45.
Samuel H. Preston, “Deadweight? The Influence of Obesity on Longevity,” The New England Journal of Medicine 352, no. 11 (2005): 1135-37.
References
- Social Security Administration, “2002 OASDI Trustees Report” (Table V. A3.-Period Life Expectancies), accessed online at www.ssa.gov on May 5, 2005; and A.W. Cheng et al., “A Stochastic Model of the Long Range Financial Status of the OASDI Program” (Baltimore: Social Security Administration, 2004).
- Katherine M. Flegal, et al., “Excess Deaths Associate with Underweight, Overweight, and Obesity,” JAMA 293, no. 15 (2005): 1861-67.
