
Au Sénégal, les prostituées sensibilisent la population au SIDA
(Décembre 2000) La Communauté sénégalaise du SIDA vient en nombre assister aux réunions du Conseil d’administration d’une association locale de femmes appelée AWA. Les conseillers des Nations Unies, le personnel médical, les représentants d’organisations non gouvernementales et le programme national sur le SIDA viennent faire honneur aux femmes pour leur leadership dans la lutte contre le SIDA.
L’AWA est une association de prostituées qui, depuis 1993, mène à bien un programme de sensibilisation au SIDA dans les villes du Sénégal. Armées de brochures éducatives et revêtues de T-shirts arborant le logo de leur association — une paire de mains aux ongles vernis, portant des bracelets, joue du tam-tam sur lequel on a inscrit “VIH” — les femmes ont dévoilé leur message sur la lutte contre le SIDA dans la rue.
La familiarité avec la vie nocturne aide la campagne de lutte contre le SIDA
Dans les bars, les boîtes de nuit, les maisons closes et les relais routiers, elles éveillent l’intérêt des gens par des discussions animées, tout en essayant de convaincre les sceptiques que le SIDA existe vraiment et que les préservatifs peuvent prévenir la transmission du virus. Tout en faisant passer des agrandissements photographiques en couleur montrant des organes génitaux comportant des signes évidents d’infections sexuellement transmissibles (IST), elles décrivent les symptômes des IST les plus répandues et démontrent comment utiliser correctement un préservatif.
En s’appuyant sur le théâtre d’intervention et leur familiarité avec la vie nocturne durement acquise, les membres de l’AWA ont informé plus de 20.000 personnes sur le VIH et les IST et ont distribué plus de 180.000 préservatifs pendant une période de trois ans et demi, de janvier 1997 à juillet 2000 ; c’est du moins ce que nous apprend Marième Soumaré, assistante sociale et co-fondatrice d’AWA.
Par une chaude après-midi d’août, tout en se préparant pour le Conseil d’administration annuel, deux membres d’AWA discutent de l’organisation. “Nous sommes rejetées par tous. Vos parents vous battent et les gens dans la rue vous attaquent”, déclare l’une d’elles. “Pourtant, le ministre de la santé est un membre d’AWA et notre drapeau flotte bien avec les autres durant la Journée mondiale du SIDA”, ajoute une autre.
Les prostituées s’organisent par le biais des cliniques de vénérologie
L’association AWA (ou “Eve”) a été créée dans la polyclinique de Dakar à l’occasion d’une campagne de lutte contre le SIDA. En 1993, les employés de la clinique ont commencé à organiser des séances régulières dans le but d’informer les prostituées sur le SIDA et les IST. Fortes de leurs nouvelles connaissances et armées du soutien du personnel de la clinique, les femmes ont demandé à recevoir une formation supplémentaire de façon à pouvoir transmettre ces informations à leurs clients et aux prostituées clandestines qui ne sont pas inscrites sur les listes de la clinique locale de traitement des IST.
Madina Bambera, une ancienne prostituée membre du conseil d’administration d’AWA, a fait partie des premiers groupes de stagiaires. “J’ai vu mes amies mourir et, dans les bars, j’ai vu les femmes qui prenaient constamment des risques… c’est pourquoi, maintenant, je vais discuter avec elles”, déclare-t-elle.
L’appartenance à AWA a donné à Mme Bambera le sentiment d’avoir un but. Elle ne fait plus partie de ces prostituées qui déambulent dans les rues décrépites entre le marché principal et le relais routier ; elle joue désormais un rôle de premier plan dans la communauté. Sa parfaite connaissance du SIDA et ses liens étroits avec le corps médical de Dakar la rendent indispensable aux yeux des autres. Les mécaniciens et les chauffeurs qui fréquentent les rues viennent lui demander des conseils et des préservatifs, et parfois, elle parvient même à convaincre l’un d’entre eux de se rendre à la clinique pour subir un test de dépistage.
Environ 300 prostituées sont inscrites à AWA dans cinq villes sénégalaises. Organisée par le biais des cliniques de vénérologie d’état qui soignent les prostituées légalisées, le conseil d’administration d’AWA dispose de 10 membres, prostituées, sages-femmes, assistantes sociales et experts sur le SIDA. “Le pouvoir de décision est entre les mains des prostituées”, explique Mme Soumaré. “Mais comme la plupart d’entre elles sont illettrées, nous les aidons à organiser les activités et à faire les démarches en matière de financement.”
Le financement d’AWA n’a jamais été bien régulier, mais depuis 1993, diverses organisations internationales fournissent occasionnellement à l’organisation l’aide financière dont elle a besoin. La mise de fonds initiale provenant de l’Agence canadienne de développement international (ACDI) a permis à AWA de lancer ses activités et a été suivie par des apports de fonds provenant du Programme d’action communautaire sur le SIDA (PACS) de Family Health International (FHI), du Programme des Nations Unies pour le développement, de l’Opération Handicap International, et par un financement supplémentaire apporté par l’ACDI. D’après Mme Soumaré, de janvier 1997 à juillet 2000, AWA a reçu 48 millions de francs CFA (68.000 dollars US), ainsi qu’une assistance sous forme de formation, conseillers et médicaments. Elle explique que les membres de l’organisation ont l’intention de solliciter un contrat de 235 millions de francs CFA, soit un budget annuel de 110.000 dollars US sur trois ans, dans le but d’élargir leurs activités.
La législation sénégalaise “tolère” les prostituées
Depuis sa création, AWA est étroitement liée au Programme national sur le SIDA qui lui a fourni une certaine assistance technique. Les liens entretenus par AWA avec ce programme et les cliniques d’état ont été facilités par la législation sénégalaise qui “tolère” les prostituées. La législation portant sur les prostituées se préoccupe surtout de régler trois questions principales en fonction d’une série de décrets et de lois en vigueur depuis les années 60. Elle se donne pour mission de prévenir la sollicitation à des fins de prostitution, de contrôler les IST par le biais de tests de dépistage obligatoires administrés régulièrement et d’empêcher la prostitution chez les mineurs de moins de 21 ans.
La législation exige que les prostituées s’inscrivent auprès de la clinique de vénérologie de leur localité et qu’elles obtiennent une carte de travail spéciale. Pour conserver leur statut légal, les prostituées doivent se présenter chaque mois à la section spéciale des prostituées de la clinique de vénérologie locale où on leur fait subir régulièrement des tests de dépistage des IST et du VIH. Par suite du surcroît considérable de visiteurs, le personnel de la clinique affirme avoir été obligé de réduire le nombre de visites à une par mois, bien que la législation exige d’en passer deux. Une femme atteinte d’une IST doit remettre sa carte jusqu’à la fin de son traitement, une précaution visant à l’empêcher de travailler, puisque les autorités peuvent arrêter les femmes qui travaillent sans carte. Les prostituées doivent verser à la clinique 500 francs CFA (environ 80 cents) par mois pour le paiement des frais des tests de dépistage et de traitement, mais nombre d’entre elles ne le font pas.
Les prostituées officielles ont la possibilité de devenir membre d’AWA et de tirer parti des activités qu’offre cette organisation, tout en s’intégrant dans la famille informelle de l’organisation, ce qui est un avantage pour ces femmes fréquemment rejetées par leurs propres familles. Les membres reçoivent des informations sur le SIDA et les IST, ainsi qu’une formation au programme d’enseignement par les pairs d’AWA. L’organisation offre également une assistance en cas d’urgence, y compris des soins médicaux et une aide psychologique.
La difficulté de trouver un autre emploi
La formation professionnelle — qui occupe également une place importante au sein des activités d’AWA — est l’une des raisons principales qui poussent les prostituées à devenir membres de l’organisation. La plupart du temps, les femmes sont illettrées et n’ont aucune ressource financière, et d’ordinaire, c’est à elles seules qu’incombe l’éducation des enfants. Les prostituées sont tout à fait conscientes des dangers auxquels elles sont exposées. Comme le soulignent les sages-femmes, les IST, et en particulier le VIH, sont encore très répandus, y compris chez les membres d’AWA. “Nous avons besoin de trouver d’autres emplois à ces femmes afin qu’elles ne soient plus obligées de dire “oui” aux hommes qui refusent de se servir de préservatifs”, déclare Marie-Jeanne Ndoye, une sage-femme travaillant à la clinique.
Nombre de prostituées insistent sur le fait qu’elles souhaitent changer d’activité. “J’aimerais trouver le moyen de m’arrêter”, déclare une femme âgée d’une trentaine d’années qui a été interviewée à la station balnéaire de Mbour. “Il y a trop de maladies, et puis, je suis trop vieille… Ils n’ont qu’à me regarder et : Allez oust ! Du balai mémé !”, dit-elle, tout en faisant un grand geste de la main comme si elle balayait le sol. Comme d’autres membres d’AWA, elle voudrait travailler comme conseillère et, le soir, organiser dans les bars des séances de prévention contre le SIDA. Malheureusement, le budget de l’organisation suffit à peine à payer les quelques employés qui y travaillent.
Les membres d’AWA ont du mal à abandonner la prostitution. Les cours de formation visant à préparer les femmes à d’autres emplois n’ont pas eu beaucoup de succès et il n’a pas été très facile de créer des “tontines”, régime d’épargne répandu en Afrique Occidentale. Ramatoulaye Dioume, un ancien employé de FHI, a conseillé à l’organisation d’engager un spécialiste financier à plein temps car, comme l’avouent les assistantes sociales sans hésitation, elles n’ont ni le temps ni les compétences nécessaires pour s’occuper des questions financières.
La mission d’AWA est aussi d’assurer la protection des droits légaux des prostituées, mais les assistantes sociales se plaignent du manque de ressources pour protéger les femmes lorsqu’elles sont arrêtées et que l’on porte contre elles des accusations mensongères. Parfois, les femmes n’ont pas d’autres choix que de faire de la prison ou de satisfaire aux exigences pécuniaires ou sexuelles des forces de police, quand ce n’est pas les deux à la fois.
En dépit de certains points faibles, AWA offre de véritables avantages aux prostituées. Comme le démontrent les interviews, plus AWA leur offre d’avantages, tels que la protection juridique, la formation, les projets sur le micro crédit, jusqu’aux préservatifs gratuits, plus elles seront nombreuses à adhérer.
Toutefois, pour devenir membre d’AWA, il faut d’abord s’inscrire auprès de la clinique locale et, pour diverses raisons, un grand nombre de prostituées refusent de faire cette démarche initiale. Certains experts déclarent qu’un tout petit nombre de femmes qui pratiquent la prostitution sont effectivement inscrites, et ce, pour plusieurs raisons : nombre d’entre elles éprouvent un sentiment de gêne, d’autres ne font de la prostitution que de temps à autre et beaucoup ne se considèrent pas comme des prostituées, bien que leurs activités répondent aux critères établis par la législation sénégalaise, et notamment le fait de se livrer au racolage sur la voie publique et de consentir à des rapports sexuels pour de l’argent.
Augmentation du nombre de jeunes prostituées clandestines
L’une des raisons pour lesquelles les prostituées ne deviennent pas membres d’AWA est essentiellement que la législation stipule que les prostituées doivent être âgées d’au moins 21 ans. En outre, il faut noter que le nombre de jeunes prostituées a tendance à augmenter fortement, et que pour des raisons physiologiques et sociales, les jeunes femmes courent un risque accru de contracter le VIH. Comme l’a signalé Marième Soumaré, la législation a été établie avant que la conjoncture économique n’ait forcé tant de jeunes filles à se prostituer et avant que le SIDA n’ait accentué les risques auxquels elles sont exposées.
Un samedi après-midi typique dans la ville côtière de Mbour, où le commerce du sexe s’adressant aux touristes européens est florissant, illustre parfaitement la situation. Des jeunes filles, certaines n’ayant pas plus de 15 ans, s’appuient contre des tabourets et gloussent comme des écolières, ce qu’elles seraient si elles habitaient ailleurs. Portant jupes courtes et pantalons moulants, et arborant aux oreilles des rangées de minuscules anneaux brillant, en or elles sont les belles des bars de cette ville côtière paillarde.
D’après Mary Cissé Thioye, une assistante sociale de la polyclinique, les taux de prévalence enregistrés chez les prostituées de Mbour sont parmi les plus élevés du Sénégal — aux alentours de 29 %. Ces chiffres ne tiennent pas compte des jeunes filles qui ne sont pas légalement en âge d’être traitées par le centre de vénérologie local et qui, par conséquent, ne peuvent pas adhérer à AWA.
Les jeunes prostituées ne subissent aucun test
L’absence des prostituées clandestines sur les listes officielles des cliniques est une cause d’inquiétude pour les experts de la santé publique et du SIDA. Premièrement, ces femmes ne bénéficient d’aucun traitement des IST et ne subissent aucun test de dépistage du SIDA. Deuxièmement, les résultats des tests que l’on a fait subir aux prostituées officielles lors des examens médicaux mensuels permettent d’obtenir des données qui servent à calculer la prévalence du SIDA au Sénégal parmi les groupes à risque élevé. Or, le fait de ne pas inclure les taux de VIH des prostituées clandestines signifie que les taux de prévalence pourraient être considérablement plus élevés que les taux enregistrés à l’heure actuelle.
Malgré le besoin évident d’abaisser l’âge légal de la prostitution, les experts en la matière, les médecins, les travailleurs sociaux et les délégués du Programme national sur le SIDA s’accordent à reconnaître qu’il serait impossible de prendre cette mesure à cause des puissants dirigeants religieux du pays.
“L’âge légal de la prostitution au Sénégal ne sera jamais modifié”, déclare le Docteur Charlotte Faty Ndiaye, présidente de la Société des femmes contre le SIDA en Afrique (Society of Women Against AIDS in Africa). “Le seul fait de souligner que la prostitution est légale pour les personnes âgées de plus de 21 ans provoquera un tollé général. Les dirigeants religieux entameraient une campagne pour interdire la prostitution sous toutes ses formes.”
Entre-temps, la clinique a mis en œuvre une stratégie non officielle lui permettant de contourner la loi. Mary Cissé Thioye, qui travaille à la clinique d’IST de Dakar, explique qu’une femme de moins de 21 ans atteinte d’une IST pourrait probablement être traitée gratuitement par la clinique, mais elle devrait payer les coûts des tests de dépistage. Un test de dépistage du VIH coûte 5000 francs CFA (environ 7,50 dollars US), tandis qu’un test de dépistage des IST coûte 3000 francs CFA (ou 4,50 dollars US) — un prix suffisamment élevé pour dissuader une femme qui gagne sa vie en se prostituant de subir régulièrement les tests de dépistage. Il est également important de souligner que les travailleurs sociaux et le personnel médical ne seraient pas en mesure de suivre cette malade par des visites à domicile et par l’administration de nouveaux tests de dépistage comme ils le feraient pour une prostituée officielle.
Elargissement de la campagne de sensibilisation au SIDA
Les travailleurs sociaux, le personnel médical et les prostituées s’accordent pour reconnaître que des changements s’imposent. Ils soulignent le besoin de protéger les prostituées, et en particulier les jeunes qui sont en nombre croissant, et de faciliter le recueil d’informations précises concernant la prévalence du SIDA au sein des groupes à risque élevé. Entre-temps, AWA occupe une place importante dans la vie de ses membres.
“AWA nous permet d’avoir notre place aux côtés des femmes de notre société. La Journée mondiale du SIDA permet à toutes les femmes de se réunir, même moi. Avant, on n’osait pas y participer… On nous voyait uniquement dans la salle d’attente de la clinique. Maintenant, toutes les femmes ont quelque chose en commun”, déclare Madina Bambera, ancienne prostituée et membre du conseil d’AWA.
Victoria Ebin est journaliste indépendante et agent de consultation au PRB basée à New York.

Sex Workers Promote AIDS Awareness in Senegal
(December 2000) Senegal’s AIDS community turns out in force when the local women’s association, called AWA, holds its board meetings. UN advisors, medical personnel, representatives from nongovernmental organizations, and the National AIDS Program come to honor the women for their frontline position in the fight against AIDS.
AWA is an association for sex workers who, since 1993, have carried out an ambitious AIDS awareness program in towns across Senegal. Armed with educational brochures and wearing T-shirts with their stylish logo — a pair of hands with painted nails and bangles beating a pink tam-tam with “HIV” on the drumhead — the women have taken their message about AIDS prevention to the streets.
Knowledge of Nightlife Helps Anti-AIDS Campaign
In bars, nightclubs, brothels, and lorry parks (truck stops), they engage people in animated debates, persuading skeptics that AIDS really does exist and that condoms can prevent the virus. Passing around large, color photos of genitalia with obvious signs of sexually transmitted infections (STIs), they describe signs of the most common STIs and demonstrate correct condom use.
Using street theater and their hard-won knowledge of local nightlife, AWA members informed more than 20,000 people about HIV and STIs and distributed more than 180,000 condoms during a three-and-a-half year period, from January 1997 to July 2000, according to Marième Soumaré, a social worker and co-founder of AWA.
One hot afternoon in August, as two AWA members prepared for the annual board meeting, they talked about the organization. One woman said, “We are rejected by everyone. Your parents beat you, people on the street attack you.” Another woman interjected, “But the Minister of Health is a member of AWA and our banner is up there with all the others on International AIDS day.”
Sex Workers Organize Through STI Clinics
AWA (a translation of “Eve”) grew out of an AIDS prevention campaign at Dakar’s Polyclinic. In 1993, clinic staff began regular sessions to inform sex workers about AIDS and STIs. Inspired by their new knowledge and with the support of clinic staff, the women requested additional training so they could pass on the information to their clients and to the clandestine sex workers who are not registered with the local STI clinic.
Madina Bambera, a former sex worker who is now a board member of AWA, was among the first set of trainees. She said, “I saw my friends die and women in bars were still taking risks so … now I go around to talk to them.”
Membership in AWA has given Bambera a new sense of purpose. No longer just another sex worker on the run-down streets between the main market and the lorry park, she now has special status in her neighborhood. Her in-depth knowledge of AIDS and close ties with Dakar’s medical establishment make people seek her out. The garage mechanics and drivers who frequent the street come to her for advice and condoms and, occasionally, she even persuades one of them to come to the clinic for testing.
There are now about 300 sex workers enrolled in AWA in five towns in Senegal. Organized through the government-run STI clinics that treat legal sex workers, AWA has a 10-member board composed of sex workers, midwives, social workers, and AIDS experts. “The prostitutes have the decision-making power,” explained Soumaré. “But most are not literate, so we help organize activities and apply for funding.”
AWA’s funding has never been steady, but since 1993, international organizations have provided intermittent financial support. Start-up money from the Canadian International Development Agency (CIDA) helped launch their activities, followed by funding from AIDSCAP of Family Health International (FHI), the UN Development Programme, Handicap International, and additional funding from CIDA. According to Soumaré, from January 1997 to July 2000, AWA received 48 million CFA francs (US$68,000) and assistance in the form of training, consultants, and medicine. She says the organization is now planning to ask for a three-year contract of 235 million CFA francs, or an annual budget of US$110,000 for three years to permit them to expand their activities.
Senegalese Legislation “Tolerates” Sex Workers
Since its founding, AWA has been closely tied to the National AIDS Program, which provides some technical assistance. AWA’s links to this program and state-run clinics can be traced to Senegal’s legislation that “tolerates” prostitution. Based mainly on a series of decrees and laws made since the 1960s, legislation on sex workers focuses on three main points. It aims to prevent soliciting in public, control STIs through regular mandatory medical tests, and prevent sex work by minors who are under the age of 21.
The legislation requires sex workers to register with their local STI clinic and obtain a special ID card. To maintain their legal status, sex workers must report every month to a special sex workers’ section of their local STI clinic where they are regularly tested for STIs and HIV. Though the law calls for two visits per month, clinic staff say overcrowding has forced them to reduce the visits to one a month. A woman who has an STI must relinquish her card until treatment is completed, a precaution that aims to keep her from working, since the police can arrest her for working without her card. Sex workers are asked to pay the clinic 500 CFA francs (about 80 cents) a month for tests and treatment, but many do not.
Official sex workers are eligible to join AWA and take advantage of its activities as well as become part of its informal family, a bonus for women who are frequently rejected by their own. Members receive information on AIDS and STIs, including training in AWA’s peer-education program. The organization also provides help in emergencies, including medical care and psychological counseling.
Finding Other Occupations Is Difficult
Job training — another focus of AWA’s activities — is high on the list of reasons sex workers give for joining the organization. Most are illiterate, have no financial resources, and generally, are the sole source of support for their children. The sex workers are well aware of the dangers they face. As the midwives point out, even among AWA members, STIs, including HIV, are still too common. “We need to find other occupations for them so they don’t have to say ‘yes’ to men who won’t wear condoms,” said Marie-Jeanne Ndoye, a midwife at the clinic.
Many sex workers are clear about their desire to change. “I’m looking for a way to stop,” said a woman in her mid-30s, who was interviewed at the beach resort at Mbour. “There are too many diseases, and besides, I’m too old … They take one look at me and, ‘Whump, it’s out you go, Mama,” she said, making a forceful sweeping gesture with her hand. She would like to work as a peer educator, organizing AIDS prevention sessions in bars every night, a goal of other AWA members. Yet, their funding barely pays the small staff.
Leaving sex work is difficult for AWA members. Training courses to prepare women for other occupations have not met with much success, nor has it been easy to establish a “tontine,” a common savings plan in West Africa. Ramatoulaye Dioume, formerly of FHI, suggested that the organization needs a full-time financial specialist because, as the social workers are the first to admit, they do not have the time or financial skills.
AWA also aims to protect sex workers’ legal rights, but social workers complain about the lack of resources to protect women when the police arrest them on trumped-up charges. Sometimes the women have to choose between going to jail or meeting police demands for money or sex, or both.
Despite some weaknesses, AWA offers real benefits to sex workers. As their conversations illustrate, the more incentives AWA has to offer, such as legal protection, training, microcredit projects, even free condoms, the greater the numbers who will join.
But becoming a member of AWA requires registering at the local clinic and, for various reasons, significant numbers of sex workers do not take this first step. In fact, some experts claim that only a fraction of the women involved in sex work are registered. Their reasons vary: many are too embarrassed; some work only occasionally; and many do not consider themselves prostitutes, though their activities meet the criteria set out in Senegal’s legislation of soliciting, having sex, and accepting money.
Number of Young, Clandestine Sex Workers Increasing
One of the major reasons sex workers do not join AWA is the law that states sex workers have to be at least 21 years old. At the same time, the number of young sex workers is increasing sharply, and the young women face heightened risks of HIV infection for physiological and social reasons. As Marième Soumaré pointed out, the law was made before economic conditions forced so many young girls into prostitution and also before AIDS added to the dangers facing them.
A Saturday afternoon in the beach town of Mbour, which has a thriving sex market for European tourists, illustrates the situation. Girls, some as young as 15, lean on bar stools and giggle like the schoolgirls they would be elsewhere. Dressed in short skirts and skin-tight trousers, with rows of tiny gold hoops glittering in their ears, they are the belles of the bars in this raunchy seaside town.
Prevalence rates among sex workers of Mbour are among the highest in Senegal — around 29 percent, according to Mary Cissé Thioye, a social worker at the Polyclinic. These figures do not take into account the young girls whose age makes it illegal for them to be treated at the local STI center and makes them ineligible for AWA membership.
Young Sex Workers Not Tested
The absence of clandestine sex workers from the official clinic lists is a reason for concern among public health and AIDS experts. First, these women are not being treated for STIs or tested for HIV. Second, the test results from official sex workers’ monthly check-ups provide data for calculating Senegal’s AIDS prevalence rates among high-risk groups. Not including the HIV rates of clandestine sex workers means the prevalence rates could well be considerably higher than the rates now reported.
Despite the clear-cut need to lower the age for legal prostitution, experts in the field, physicians, social workers, and officials at the National AIDS Program agree that it would be impossible to take this step because of the country’s powerful religious leaders.
“The legal age of prostitution will never be changed in Senegal,” said Dr. Charlotte Faty Ndiaye, president of the Society of Women Against AIDS in Africa (SWAA). “Even to point out that prostitution is legal for those over 21 will raise a furor from the public. The religious leaders would start a campaign to make all prostitution illegal.”
Dr. Karim Seck, an adjunct to the director of the National AIDS Program, agreed. “The religious leaders would lobby. Already they say we have authorized prostitution. If we try to lower the age, we will only have more problems.”
In the meantime, the clinic has an informal strategy to work around the laws. Mary Cissé Thioye, who works at the STI clinic in Dakar, said that a woman under 21 could probably receive free treatment for an STI at the clinic, but she would have to pay for testing. The HIV test costs 5000 CFA francs (about US$7.50), while the testing for STIs is 3000 CFA francs (US$4.50) — high enough to prevent a woman who earns her living from sex work to avoid regular testing. Equally important, social workers and medical staff would not follow up on her case with house calls and re-testing as they would for a registered sex worker.
Expanding the AIDS Awareness Campaign
Social workers, medical personnel, and sex workers agree that changes need to be made. They point to the need to protect sex workers, especially the growing numbers of young ones, and to facilitate the gathering of accurate information on AIDS prevalence among high-risk groups. In the meantime, AWA is filling a place in the lives of its members.
“AWA lets us take our place among the women of our society. At International AIDS day, all the women are there, and I am, too. Before, we didn’t dare participate … We were only in the waiting room of the clinic. Now, we have something to share with other women,” said Bambera, the former sex worker and AWA board member.
Victoria Ebin is a freelance journalist and consultant to the Population Reference Bureau, based in New York City.
Latest UN data on HIV/AIDS: www.unaids.org.
Resourcers
View All
Cervical Cancer Is Major Health Problem in Latin America
Date
December 1, 2000
Author
PRB
(December 2000) Cancer of the uterine cervix is a major public health problem in Latin America and the Caribbean. Based on 1990 data from the International Agency for Research on Cancer (IARC), it represents the most common cause of cancer for women in the region (52,000 new cases per year) and the fourth leading cause of death among women ages 15 to 64 (25,000 deaths per year).
Haiti has the region’s highest incidence of cervical cancer (91 cases per 100,000 women) and Nicaragua has the highest mortality from the disease (33 deaths per 100,000 women).
Cervical cancer is caused primarily by certain strains of the human papillomavirus (HPV), a common sexually transmitted infection. According to the Pan American Health Organization (PAHO), 60 percent of this type of cancer occurs in women between 35 and 60.
Cervical cancer is preventable and can be treated effectively provided women know about the disease and the means to detect and prevent it; many women in Latin America and the Caribbean do not know about cervical cancer or about available screening and treatment programs. Prevention efforts have focused on using the Papanicolaou (Pap) smear to screen at-risk women and then treating the precancerous lesions by removing the diseased tissue. Most countries in the region offer Pap screening but they lack prevention programs and do not offer follow-up or treatment in cervical cancer cases detected by the smear.
Overall, 63 percent of women in the region have had a Pap smear at least once, but there are great differences across countries. While 70 percent of women in Brazil and Costa Rica have had at least one Pap smear, only 35 percent of women in Nicaragua have had at least one test. The vast majority of these women have been screened during their reproductive life, at young ages when the risk of precancerous lesions is lower. It is important to note that one Pap test alone is essentially useless; women need to obtain regular Pap tests.1
Women from lower socioeconomic status and those with less education are less likely to know of the Pap test. Furthermore, women with the least education are more likely to be diagnosed with later stages of cervical cancer. In most instances, they do not have the financial resources to obtain treatment.
Whatever the screening test used, a fundamental problem in the region is the follow-up of screened women and the provision of diagnosis and treatment for cancer cases detected during the screening. A recent study in Peru showed that only 20 percent of women who had a Pap smear that identified a precancerous lesion received a diagnosis and follow-up treatment.2
There are effective alternatives to Pap tests and efforts to use HPV testing to identify women at high risk for cervical cancer. Researchers are also working to produce a viable vaccine against one or two types of HPV. There are also simple and inexpensive techniques to treat precancerous lesions, like cryotherapy, that can be applied in primary care clinics throughout Latin America and the Caribbean, thus reducing much potential suffering for affected women.
A Woman’s Perspective
Women’s feelings are often not considered and made an integral part of care, even in difficult situations when a woman needs to be told that cancer has been diagnosed.
“When they tell you that you have cancer, you get all nervous; and even though they explain it quickly, you somehow don’t hear. They said ‘Do you have any questions?’ and I said ‘No, its okay I understand everything clearly,’ but I did not understand, and I was so nervous that all I wanted was to leave. They told me what I had, and I started crying, for blocks and blocks, as if someone had died within me. People were looking at me and my little girl; I was looking at the trees, as though I had never seen them in my entire life. I thought that tomorrow I was going to be dead, and who would care for my children.” I wanted to question the physician, who didn’t even look at me; instead, he said ‘Go outside’.”3
In the Region, Central America Has the Highest Incidence and Mortality Rates
Cervical cancer is a significant reproductive health problem in the countries of Latin America and the Caribbean, which have one of the world’s highest incidence and mortality rates for the disease, according to IARC.4 Generally, incidence is high across many of the countries in the region, regardless of their development status. Countries with low and medium low economic status, however, exhibit higher mortality levels. Among the sub-regions, Central America has the highest incidence and mortality rates.
According to PAHO, trends in the region suggest that mortality due to cervical cancer did not decline between 1960 and 1993 but remained fairly constant (five to six deaths per 100,000 women).5 This scenario applies to countries as varied as Brazil, Colombia, Cuba, Ecuador, Guatemala, Trinidad and Tobago, Uruguay, and Venezuela. Three countries — Chile, Costa Rica, and Mexico — have recorded changes over time, but not always for the better. For instance, in Costa Rica, there was a reduction in mortality from 1965 to 1973; however, this may be due to improved coverage and accuracy in the certification of deaths rather than due to real reductions. Chile realized a decline in mortality from cervical cancer among women under 35, but not among older women, who represent the majority of cases. In Mexico, on the other hand, there appears to have been an increase in deaths from cervical cancer, but this may be due to better certification of deaths.6
Women Typically Become Infected During Their Teens, 20s, or 30s
Cervical cancer is a disease that largely affects middle-aged and elderly women. Sixty percent of this type of cancer occurs in women between 35 and 60 who are in the prime of life and important supporters of their families. Unlike many cancers, cervical cancer can be prevented. The first step is to educate women about how to protect themselves against HPV, a common sexually transmitted infection (STI) that can cause cervical cancer. According to the World Health Organization’s Programme on Cancer Control, over 99 percent of cervical cancers are due to certain types of HPV. Other important factors associated with the disease include tobacco use, number of sexual partners (for either the woman or her partner), early age at first intercourse, and early age at first birth.
Women typically become infected with HPV during their teen years and in their twenties or thirties. However, it may take 20 or more years for cervical cancer to develop after the initial infection. Cervical cancer develops slowly from precancerous lesions (dysplasia). There are typically three stages: low-grade cervical dysplasia, high-grade dysplasia, and invasive cancer. Seventy percent of low-grade dysplasia disappears over time and does not require treatment. High-grade dysplasia, which will progress to cancer within 10 years if left untreated, requires both treatment and regular monitoring. Invasive cancer, if not treated with surgery and radiation therapy, is always fatal.8
Primary prevention, which includes a focus on using condoms or other barrier methods and engaging in mutually monogamous sexual relationships, help prevent cervical cancer, but it is unclear how these strategies affect the overall incidence of the disease. Preventing HPV transmission may pose greater challenges than most STIs. It is easily transmitted, asymptomatic, and the virus can remain in the body for years. Furthermore, HPV can occur in the genital and anal parts of the body, including areas not covered by male condoms.
Proper Screening Can Be an Effective Intervention
Secondary prevention strategies such as inexpensive screening, treatment, and follow-up have been highly effective in reducing the incidence of cervical cancer. To date, prevention efforts have focused on using the Pap smear to screen at-risk women and then treating the pre-cancerous lesions by removing the diseased tissue. In situations where screening quality and coverage is high, this procedure has significantly reduced the incidence of cervical cancer. In Latin America and the Caribbean, an estimated 63 percent of women have had a Pap smear. There is, however, great variability in coverage across countries. For example, PAHO survey data suggest that only 35 percent of women in Nicaragua have had a Pap smear at least once, compared with 70 percent in both Brazil and Costa Rica. In Haiti, there is no national screening policy for cervical cancer, and there are only a small number of cytologists throughout the country.9
Other factors such as age, education, income, and residence contribute to large differences in Pap smear coverage across the region. For instance, according to PAHO, in Brazil, Chile, and Mexico, women from lower socioeconomic status are less likely than their better-off counterparts to know of the Pap test or to have undergone a test. In addition, in some countries such as Ecuador, the incidence of cervical cancer is almost twice as high among women with no education or only primary education when compared to those with secondary or higher education. And women with the least education are more likely to be diagnosed with later stages of cervical cancer (stages III or IV) whereas women with higher education have their cancers detected earlier.9
When implemented properly, screening can be an effective intervention for cervical cancer. According to the IARC, screening once every three years can produce a 91 percent reduction in lifetime incidence of the disease, while an interval of five years confers an 84 percent benefit.10 Furthermore, treating the precancerous tissue protects women from developing cervical cancer in the future.
In addition to being easy and effective, screening and treatment of precancerous lesions is cost-effective when compared with expensive hospital-based treatment of invasive cancer. According to the World Bank, it costs about US$100 per disability-adjusted life year (DALY) gained to conduct cervical cancer screening (defined as screening women every five years, with follow-up for identified cases). This compares with about US$2,600 per DALY for treatment of invasive cancer and palliative care.11
While screening and treatment programs have been highly successful in reducing deaths from cervical cancer in more developed countries, they have not been applied successfully in Latin America and the Caribbean. Researchers at PAHO have cited several specific weaknesses to implementing and sustaining screening and treatment programs. These include:
- Low levels of coverage for high risk women (those ages 35 to 64 who have no access to screening programs) and inappropriate repetitive screening of younger lower risk women (under 30) through family planning and prenatal care programs. This does not mean that younger women should not obtain Pap smears. Most screening programs miss older women who do not seek family planning and prenatal care programs and only come to medical attention at late stages of their disease.
- Lack of timely consultation due to a lack of understanding about cervical cancer or sociocultural barriers, or both, among women at risk; limited access to health services; and poor communication between women and their health care providers.
- Poor quality of cytology tests; lack of knowledge about other screening options; and insufficient monitoring, treatment, and follow-up for women with abnormal cytology results
- Little knowledge by policymakers about the total societal costs of various screening and treatment options.12
In order to surmount these weaknesses, some countries have restructured their cervical cancer screening programs. Strategies have been adopted to limit screening to women at highest risk of high-grade dysplasia, to reduce the frequency of screening among women who have had at least one normal smear, and to recommend regular follow-up rather than treatment for young women with mildly abnormal smears.
Screening Methods Other Than Pap Smears Can Also Detect Cervical Cancer
Visual inspection involves simply looking at the cervix for any signs of early cancer. Though this procedure has not been effective in identifying precancerous conditions, it has yielded positive results. Visual inspection with acetic acid (VIA) involves wiping the cervix with a solution of acetic acid (vinegar), illuminating the cervix, and then having a trained health care worker inspect the area with the naked eye. The vinegar causes precancerous tissue on the cervix to appear as white blotches. Results of several studies in developing countries have shown that VIA can be as effective as Pap smears in detecting high-grade lesions. According to researchers with JHPIEGO, a reproductive health agency affiliated with Johns Hopkins University, more than 75 percent of pre-cancerous lesions in cervical tissue can be revealed using this screening method.13 This procedure may become a first line of defense against cervical cancer in developing nations. It is less expensive and complex than Pap smear screening and may allow for screening and treatment to occur in the same visit. Using VIA will still require training a broad range of primary care providers to make determinations about proper treatment for precancerous lesions.
In addition to visual inspection procedures, other researchers have focused on using HPV testing to identify women at high risk for cervical cancer. These scenarios may prove promising for developing countries in the future; however, barriers such as cost and technical requirements prevent their use in low-resource settings.
Finally, there are also efforts underway to produce a vaccine for HPV. According to PATH, nearly 30 HPV vaccines are being tested in clinical trials. If effective, a vaccine would reduce the risk of cervical cancer significantly in the treated population. A viable vaccine against one or two types of HPV may be available in as little as five years.14
Two Relatively Simple Treatment Options
In addition to screening, adequate treatment services need to be provided. In the past, many countries have provided inadequate monitoring of women with abnormal cytology smears and have delayed confirming the diagnosis and treating the high-grade lesions. There has also been “overtreatment” of preinvasive cervical lesions with aggressive and costly approaches such as cone biopsy or hysterectomy, as opposed to more appropriate, outpatient approaches.
Two relatively simple treatment options exist for destroying or removing pre-cancerous tissue. One common method, cryotherapy, which involves freezing abnormal tissue, has an overall effectiveness rate of 80 percent to 90 percent. Cryotherapy has particular advantages in low-resource settings:
- The equipment can be relatively cheap and easy to operate.
- Specialist surgical skills are not required, although trained physicians must perform the procedure (often they are not available at the primary health care level).
- Complications are rare, although the procedure can have negative health effects such as bleeding, discharge, and cervical scarring.
- It reduces the number of visits a woman must make to receive proper care.
Another procedure, the loop electrosurgical excision procedure (LEEP), which uses a thin electrified wire to excise cervical lesions, also has high efficacy (90 percent to 95 percent). A PAHO survey of health professionals in the region indicated that many preferred and used LEEP.15
Education Is Key to Prevention and Treatment
Despite the availability of screening and treatment options for cervical cancer, many women in Latin America and the Caribbean do not know about the disease nor are they aware that detection and treatment can prevent the health problem. For instance, in one study carried out by researchers at Mexico’s National Institute of Public Health and the National Autonomous University of Mexico, nearly 42 percent of the women were not familiar with the purpose of the Pap test. Of this group, only about 3 percent had ever had the test.16 Another study conducted by a University of Chile researcher determined that Chilean women avoided taking the Pap test as they were afraid of being reproached by health-care workers for having failed to have the test at the recommended interval (60 percent), feared experiencing pain from the test (39 percent), feared bleeding (20 percent), and feared losing part of their uterus (14 percent). In addition, of the women with intrauterine devices, over 25 percent feared removal of the device.17
Efforts to improve women’s awareness and health providers’ knowledge of prevention options are critical to achieving a successful cervical cancer prevention program. Most importantly, information needs to reach all women but particularly those who are at the highest risk for treatable, pre-cancerous lesions (those between the ages of 35–60). PATH has recommended several approaches including using established communication channels like the mass media; local community and women’s groups, their children, and their husbands; and linking screening to an important event in a woman’s life such as becoming a grandmother. In addition, health providers need to be educated about the public health rationale for limiting the frequency of screening, focusing on older women, and emphasizing treatment of pre-cancerous conditions.18
Liz Creel is a population specialist at the Population Reference Bureau.
References
- Jacqueline Sherris, Program for Appropriate Technology in Health (PATH), personal communication with author, November 2000.
- Cristina Ferreccio, Pan American Health Organization (PAHO), personal communication with author, November 2000.
- M. Matamala et al., “Calidad de la atencion desde un enfoque de genero,” Mujer, Salud y Desarrollo (Washington, DC: PAHO, 1995.)
- Jacques Ferlay, D. Maxwell Parkin, and Paolo Pisani, “GLOBOCAN: Cancer Incidence and Mortality Worldwide” (Lyon, France: International Agency for Research on Cancer, 1998).
- PAHO, Cervical Cancer Screening in Latin America and the Caribbean, November 1996.
- Sylvia Robles, Franklin White, and Armando Peruga, “Trends in Cervical Cancer Mortality in the Americas,” Bulletin of the Pan American Health Organization 30, no. 4 (1996): 290-301.
- PAHO, Health in the Americas, Vol. 1 (1998): 171-73.
- K. Nasiell et al., “Behavior of Mild Cervical Dysplasia During Long-Term Follow-Up,” Obstetrics and Gynecology, 67, no. 5 (May 1986): 665-69; and P. Holowaty et al., “Natural History of Dysplasia of the Uterine Cervix,” Journal of the NCI 91, no. 3 (Feb. 1999): 252–58 as cited in Jacqueline Sherris and Cristina Herdman, “Preventing Cervical Cancer in Low-Resource Settings,” Outlook 18, no. 1, September 2000.
- Anthony Miller and Sylvia Robles, “Workshop on Screening for Cancer of the Uterine Cervix in Central America,” Bulletin of the Pan American Health Organization 30, no. 4 (1996): 397-408.
- Fabián Corral et al., “Limited Education as a Risk Factor in Cervical Cancer,” Bulletin of the Pan American Health Organization 30, no. 4 (1996): 322-29.
- Miller and Robles, “Workshop on Screening for Cancer of the Uterine Cervix in Central America.”
- D.T. Jamison et al., Disease Control Priorities in Developing Countries (New York: Oxford University Press, 1993).
- PAHO, PAHO Backgrounder Sheet, accessed online at www.paho.org/
English/Dpi/releases1999/rl990921.htm on Sept. 22, 1999. - The Lancet, March 13, 1999 as cited in Environmental Health Perspectives 107, no. 10 (Oct. 1999), accessed online at http://ehpnet1.niehs.nih/gov/docs/1999/107-10/forum.html.
- Adrienne Kols and Jacqueline Sherris, “Vaccines: Promise and Challenges,” (Washington, DC: PATH, July 2000).
- Amie Bishop, Jacqueline Sherris, Vivien Davis Tsu, and Maggie Kilbourne-Brook, “Cervical Dysplasia Treatment: Key Issues for Developing Countries,” Bulletin of the Pan American Health Organization 30, no. 4 (1996): 378-86.
- Patricia Nájera Aquilar et al., “Factors Associated with Mexican Women’s Familiarity with the Purpose of the Pap Test,” Bulletin of the Pan American Health Organization 30, no. 4 (1996): 348-53.
- Silvia Álvarez, “Knowledge and Fears Among Chilean Women With Regard to the Papanicolaou Test, Bulletin of the Pan American Health Organization 30, no. 4 (1996): 354-61.
- Jacqueline Sherris, Planning Appropriate Cervical Cancer Control Programs (Washington, DC: PATH, 1997).
What Do These Terms Mean?
Cervix: the narrow passage at the lower end of the uterus, which connects with the vagina.
Cytologist: a person trained in the study of the structure and function of cells. The examination of cells under a microscope is used in the diagnosis of various diseases such as cervical cancer, where cells are obtained by scraping the cervix.
Palliative care: the World Health Organization defines this as the active, total care of patients whose disease is not responsive to curative treatment (or for whom curative treatment is not available). It aims to provide the best possible quality of life for patients and their families. Palliative care includes control of pain, of other symptoms, and of psychological, social, and spiritual problems.
For More Information
The Alliance for Cervical Cancer Prevention was formed in 1999 with the support of the Bill and Melinda Gates Foundation to clarify, promote, and implement strategies to prevent cervical cancer in developing countries. It is composed of five international agencies:
- EngenderHealth, a family planning and reproductive health agency,
- the International Agency for Research on Cancer (IARC), WHO,
- JHPIEGO Corporation, a reproductive health agency affiliated with Johns Hopkins University,
- the Pan American Health Organization (PAHO), WHO, and
- PATH (Program for Appropriate Technology).
For more information about the Alliance, visit their website at www.alliance-cxca.org

Early Sexual Activity Raises HIV Risk for Trinidad and Tobago Girls
(December 2000) Jean Jones (not her real name) spent most of her childhood and early teens at a home for children. At 15, she got lucky and went to live with relatives. At 16, however, she had a son, discovered that she had HIV, and that her relatives no longer wanted her around.
Jones and her seemingly healthy 5-year-old son now live at the home of a health worker.
“Sometimes, I just cry; I don’t eat, and I get sick all the time. I know I’ll die sometime soon, but I’m not too worried about myself; it’s my son I am concerned about,” says Jones, bundled up at the edge of a bed in the health worker’s modest home.
Six Times as Many Girls as Boys 15-19 Years Have HIV in Trinidad and Tobago
Jones’ HIV/AIDS condition is replicated many times over among the young female population of Trinidad and Tobago. In the age group 15–19 years, six times as many young women as young men have HIV. This is a dramatic turnaround of the numbers over the last five years. It has come about because of certain factors, including early sexual initiation.
A survey was conducted of 676 young adults (10–29 years old) in Tobago in April by the Family Planning Association; the Tobago AIDS Society; the Caribbean Epidemiology Centre, with support from the Dutch Embassy in Trinidad and Tobago; and the German Technical Cooperation Agency in Tobago. The study found that sexual activity starts as early as 10 years old, the average age being 14 years old for boys and girls combined. Thirteen percent of those 10–14 years old had had sex.
The overall young age of sexual initiation as reported by the study reaffirms that young people between the ages of 10 and 24 years are at high risk of acquiring HIV infection, states the report of the survey.
Young Women Have Older Partners
Along with the quantitative findings, focus groups were also conducted. Participants of these groups remarked on the phenomenon of young women having sex with older men, where materialism plays a role. The report points out that older men are usually able to afford more enticements. It notes that the men take advantage of their more favorable financial positions when they seek relationships with young girls. Unfortunately, a consequence of this age differential between males and females in sexual relationships is that the young women are more susceptible to HIV infection.
Incest, a subject that is not talked about or acknowledged, has a heavy impact on girls. Six percent of the young people surveyed — all girls — said they had had sex with a father, stepfather, uncle, or older brother.
Some girls did not see anything wrong with having sex with a member of the family, says Anne-Marie De Gazon-Washington, a youth officer who was part of the team that conducted the survey. “If that is so, you have to consider how that translates into risky, grown-up behavior.”
Young Mothers Are Passing the Virus to Their Babies
A key problem that goes along with rising sexual activity and HIV transmission among young people is the increasing number of young women who transfer the virus to their babies. At the Tobago Regional Health Authority hospital in the capital, Scarborough, HIV testing was conducted on the umbilical cords of newborn babies. The infection rate of the babies of mothers in the 14-24 age group was about 3.6 percent — roughly double the rate for older women.
Addressing these potentially infected babies is urgent.
“If something is not done about mother-to-child transmission, we run the risk of realizing the international norm of 30 percent of the babies born to HIV-positive mothers contracting the virus,” says the hospital medical director of Tobago, Dr. Maria Dillon-Remy. That would severely affect the 750 babies born in Tobago every year and eventually the 50,000 population of the island, Dr. Dillon-Remy observed.
Dr. Violet Duke of the Ministry of Health in Trinidad says the government has developed a policy that includes voluntary screening for pregnant women. The next stage is to provide treatment for mothers who develop AIDS after having their babies, “otherwise we will have a generation of orphans,” notes Duke. The third stage of the policy would be to begin making combination HIV drug therapy available to persons infected with AIDS.
Under the new policy, a pilot study began in August 1999 with voluntary screening of women for HIV. With the assistance of the Medical Research Foundation of Trinidad and Tobago, six women were treated during pregnancy and, along with their babies, they also received treatment during delivery with AZT. Five other babies whose mothers had not received the drug during pregnancy received AZT treatment. Only one of the 11 babies among those women who were treated has developed the virus.
Given the study results, “We hope to soon be able to offer universal screening to all mothers,” says Dr. Dillon-Remy, noting that the incentive given to women with HIV that their babies can be spared the virus “has proven to be the most important reason why mothers are taking the test.”
Some Teenagers Say the Problem of High-Risk Sexual Behavior Begins at Home
Young people have their own ideas about the reasons for early sexual activity among their peers.
Adana Clarke, 18, says one reason that young people, especially girls, assume high-risk behavior at an early age has to do with the failure of parents to speak with their children about sex, postponing the issue until the young people are all but out of their teenage years.
Referring specifically to girls, she adds that “a lot of young people are not given love and affection in their homes, and when they get out onto the streets and the fellas tell them ‘I love you,’ they feel wanted. And because they have low self-esteem, they are forced into sexual behavior at an early age.”
Charles Smith, just out of high school, says parents employ a double standard that is also contributing to the spread of the virus in Tobago. He notes that while parents caution their girls about “appropriate behavior,” they leave their boys “to do as they wish.”
Policy Recommendations Include Services for Young People
Policy recommendations coming out of a workshop on the Sexual Health Needs of Youth in Tobago include the establishment of youth empowerment centers where young people can go for lifestyle counseling and adolescent and health services without the stigma of visiting an AIDS clinic for testing.
One policy approach recommended is the reorientation of health services in order to create youth-friendly, youth-specific approaches to sexual and reproductive health. The young people fear for confidentiality in a small society.
One desire of the youths is for the government and the Tobago House of Assembly, the body responsible for the administration of the local affairs of Tobago, to adopt a policy of having an official youth representative in the Assembly to look after the interests of young people.
One important policy recommendation, however, is for sex education to be offered at school as well as at home. Another calls for increasing the self-esteem of young girls, “especially to have girls who are sexually violated by fathers and uncles begin to understand that it is wrong, and to end the culture of silence about sex in our society,” says youth officer, Anne-Marie De Gazon-Washington.
Tony Fraser is a freelance writer in Trinidad.
Resources
View All
For China, a Census That Really Counts
(December 2000) Tracking down more than one billion Chinese citizens is no easy task, but China’s government is about to try. From November 1 to 15, more than five million census-takers will visit China’s estimated 350 million households to conduct the fifth national census since the founding of the People’s Republic in 1949. The reliability of the data will be a question, to be sure, especially since local officials pay a price if births in their bailiwick exceed targets. Even so, the final tally will be viewed in Beijing as a report card on the government’s population stabilization program, possibly leading to a tightening of birth restrictions even as family planning services continue to expand.
The official goal is to be under 1.3 billion. If the census total (due in February) surpasses that figure, some experts believe the government will step up pressure on families to limit births. “I don’t think they’ll change the rules, but they could get tougher on enforcement,” says Susan Greenhalgh, a China population specialist at the University of California-Irvine. Current rules limit most urban couples to one child — two if both parents are only children — while rural residents may have two children. These limits are widely evaded, however, and implemented unevenly throughout China, making enforcement a key issue. The 1990 Census revealed higher than expected fertility levels and was followed by a draconian toughening of enforcement, though no clear-cut connection between the two has been documented.
If the government meets its goal, stricter enforcement is not expected to be as high a priority. In some cases, modest adjustments to the urban one-child policy might even be possible. Officials in Shanghai have already granted residency rights to second-born children, giving them access to public education and health care. Any future reforms are likely to be downplayed, however, and coupled with calls for achieving national population targets. “There’s a tremendous fear that if they liberalize too quickly, people will rush to have more children,” says Greenhalgh, “so there’s a go-slow approach to reform.”
China’s Population, 1950-2050
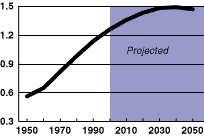
Source: U.S. Census Bureau, International Data Base.
Whether or not the census results please Beijing, the government will probably continue its efforts to improve the availability and quality of family planning services, a movement underway since the mid-1990s. Family planning service centers have sprung up across China, offering method choice counseling, reproductive health services, prenatal care, and pre-marital counseling. The government estimates that 660 of China’s 3,000 counties have participated in the movement so far, marking a sizable shift in how population goals are pursued in some areas. “There has been a sea change in attitude, rhetoric, and intention,” says Joan Kaufman of the Ford Foundation in Beijing, though she is quick to point out that local approaches vary widely and that much retraining is needed.
China’s interest in the quality of family planning services, with increased emphasis on reproductive health, was sparked by the 1994 International Conference on Population and Development in Cairo, which stressed the value of such services. The State Family Planning Commission (SFPC) first introduced the reforms in 1995, starting with six rural counties and five urban districts in eastern China. The UN Population Fund and the Ford Foundation became involved in funding the reform effort through the SFPC in the late 1990s.
The government’s interest in family planning as a means of moderating population growth has also risen as China’s economy has shifted from state planning to free-wheeling markets, a transition that has made coercive approaches less workable. The erosion of control has been particularly pronounced in the countryside, where the majority of China’s population still resides. Increasingly affluent parents can often afford to pay the fines or bribes necessary to have above-quota children, or simply travel to a new area to escape scrutiny. As a result, while the government claims that the national fertility rate is 1.8 children per woman, some Chinese demographers believe the real number lies between 2.0 and 2.3. With traditional controls looking ineffective, the government appears to hope that a more customer-oriented approach will fit better into China’s changing society.
Although Chinese officials are reportedly happy with the results of the reforms undertaken so far, practical obstacles will impede the expansion of family planning services in the future. Among other problems, shortages of technical expertise and limited funding are key constraints. Financial concerns are compounded by wasteful duplication of services between the family planning service centers and local health facilities, a problem that has sparked heated debate in Beijing.
And as for birth restrictions, while officials may tinker with the policy, there is broad consensus in China that controlling population growth remains critical to the country’s development. In March, for example, the government announced plans to apply birth limits more strictly to China’s ethnic minorities, groups that have been relatively free from such controls in the past. “It would be a fantasy to think that the population stabilization goals will go away — they won’t,” says Kaufman. “It’s how they’re pursued that is the question.”
Bingham Kennedy, Jr. is associate editor of Population Today.
Resources
View All
Nafis Sadik, Architect of ICPD
Date
December 1, 2000
Author
PRB

Nafis Sadik will retire at the end of this year from the UNFPA. Source: UN Photo 185585/ J. BU 1060L
This is the final installment in a series profiling people who have influenced thinking about population over the past century. A year’s worth of profiles could not do justice to all the people who deserve recognition. Our hope is that, by bringing you the insights of today’s population specialists on the contributions of their predecessors and contemporaries, we have personalized a century of population change and demographic work.
(Population Today, November/December 2000) Many people think of Nafis Sadik as the symbol of the remarkable new consensus that emerged from the International Conference on Population and Development (ICPD) in Cairo in 1994. This profile is an account of how Dr. Sadik helped make ICPD happen and why she deserves much of the credit for its success.
Nafis is an “in-from-the-field, up-through-the-ranks” leader with a masterful grasp of population issues. As a young doctor in Pakistan in the late 1950s, she taught rural women and men about family planning. She also helped develop the country’s first population policy as a member of the National Planning Commission. After joining the UN Population Fund (UNFPA) in its formative years, Nafis quickly rose to become director of operations, assistant executive director, and then executive director.
I have known Nafis since 1975. When I headed the U.S. Agency for International Development’s Office of Population in the early 1980s, she and I worked to minimize disruptions caused by the Reagan administration’s efforts to eliminate U.S. population assistance. I knew from the beginning that Nafis was an extremely able program manager; I learned later what a skillful diplomat she is.
In 1992, Nafis was named secretary-general of the ICPD. At that time, two political currents with profound implications for ICPD were flowing through the international community. The first was opposition to population policies that placed demographic objectives ahead of women’s health. The second was demand for a more active role for nongovernmental organizations (NGOs) in international political affairs. Nafis’ challenge was to channel both in a positive direction.
Rights advocates argued that demographic targets led to heavy-handed, even coercive, programs. Program administrators defended targets as necessary to keep program workers focused. Nafis, a longtime program administrator, was inclined to side with the latter. But as she listened to the impassioned voices of women, she changed her mind. When it was time to draft the conference document, her position was clear: The objective should be to serve individual needs. If that were done well, population growth would take care of itself. That point of view prevailed.
Representatives of international NGOs and foundations urged Nafis to open the ICPD to NGOs. Nafis at first hesitated but realized that civil society would not be denied a significant role in future global negotiations. She urged all governments to include NGO representatives in their delegations, and she supported an NGO presence throughout the ICPD process. In turning a political necessity into a virtue, Nafis also helped permanently change the role of civil society in international political conferences.
Perhaps Nafis’ most important contribution to ICPD was the introduction of global goals for the year 2015. Speaking before the final preconference meeting in April 1994, she proposed five 20-year goals: increased availability of family planning services; reduced infant mortality; reduced maternal mortality; increased life expectancy; and increased access to education, especially for girls and women. Her proposal demonstrated the interrelationship of key development goals: None could be achieved unless all were achieved.
ICPD culminated a distinguished career: from grassroots doctor to architect of one of the most successful international agreements of the last 30 years — certainly the most important in the history of the global population movement. While many deserve credit for the new ICPD orientation toward population and family planning, Nafis Sadik stands tallest because of her imagination, political skill, and leadership.
Steven Sinding is professor of clinical public health at Columbia University. He directed population programs at the Rockefeller Foundation from 1991 to 1999, and at the U.S. Agency for International Development from 1983 to 1986.
Articles in This Series
- Alfred Lotka, Mathematical Demographer
- Margaret Sanger, Birth Control Pioneer
- Alan F. Guttmacher, People’s Physician
- Gregory Pincus, Father of the Pill
- John D. Rockefeller 3rd, Statesman and Founder of the Population Council
- Reimert T. Ravenholt, USAID’s Population Program Stalwart
- Nafis Sadik, Architect of ICPD
Resources
View All
How Involved Are Fathers in Raising Children?
(December 2000) Most of the research on parenting in the United States has surveyed mothers, but not fathers. The recent surge of interest in the father’s role has promoted surveys of both parents, which have, incidentally, documented substantial discrepancies between men’s and women’s reports about their relative involvement in raising their children. A 1999 University of Maryland study explored these discrepancies by asking a sample of mothers and fathers about five domains of parenting: discipline, play, emotional support, monitoring of activities and playmates, and basic care.
Parents were asked: “Ideally, who should discipline children, mainly the mother, mainly the father, or both equally?” Similarly, respondents were also asked: “In parenting your children, who disciplines the children, mainly you, mainly the child’s father/mother, or both parents equally?” Questions were repeated for each domain of childrearing and were asked both of parents who currently had children in the home as well as of parents who had adult children.
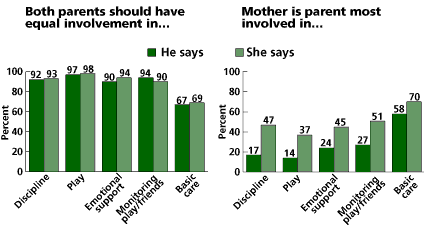
There is overwhelming consensus between men and women that parenting should be shared equally across most domains, as shown in the figure. For four of the areas — disciplining children, playing with children, providing emotional support, and monitoring activities and friends — at least 90 percent of men and women say these parenting domains should be shared equally. More than two-thirds of men and women say that caring for children’s needs should be shared equally by mothers and fathers.
Parents’ reports of actual involvement, however, do not agree. Mothers are far more likely than fathers to report that the mother is the main disciplinarian of children (47 percent, compared with 17 percent), and that it is mainly the mother who plays with children (37 percent, compared with 14 percent). Similarly, mothers are far more likely than fathers to report that the mother provides most of the emotional support of children (45 percent compared with 24 percent) and that the mother is the one who mainly monitors their children’s activities (51 percent compared with 27 percent). More mothers than fathers believe that mothers are the main caretakers of children (70 percent vs. 58 percent). Overall, fathers are much more likely to hold the view that domains are shared equally with their partners, while mothers are much more likely to report that they are primarily the ones involved in rearing their children.
Reference
Melissa Milkie, Suzanne M. Bianchi, Marybeth Mattingly, and John Robinson, “Fathers’ Involvement in Childrearing: Ideals, Realities, and Their Relationship to Parental Well-Being.” (Revised version of a paper presented at the annual meeting of the American Association for Public Opinion Research, Portland, OR, May 18–21, 2000.)
This article is excerpted from the Population Bulletin “American Families” (Vol. 55, No. 4, December 2000), published by the Population Reference Bureau.
Suzanne M. Bianchi is professor of sociology and faculty associate in the Center on Population, Gender and Social Inequality at the University of Maryland, College Park.
Lynne M. Casper is health scientist administrator and demographer at the Demographic and Behavioral Sciences Branch, National Institute of Child Health and Human Development.

Older Women: Living Longer, Living Alone
Date
November 20, 2000
Author
PRB
(November 2000) Three quarters of older American men live in a family setting, while only half of older American women do. In 1999, 9.8 million people ages 65 and older lived alone, 77 percent of whom were women. The percentage of older people living alone increases with age. In 1999, about 15 percent of men and 31 percent of women ages 65 to 74 lived alone, but among those 75 and older, 20 percent of men and 51 percent of women lived alone. The percentage of women ages 75 and older living alone has increased by 10 percentage points since 1970.
The percentage of older people residing in institutions has been declining in recent years. According to the National Nursing Home Survey, the percentage of people ages 85 and older residing in nursing homes declined from 22 percent in 1985 to 19 percent in 1997. Among people ages 75 to 84, the percentage in nursing homes declined from 6 percent in 1985 to 5 percent in 1997. This decline may reflect the decline in disability rates among the older population, reported by several sources, and the increase in the availability of home health services over this period. Though the percentage of older people in nursing homes declined, the absolute number of older people in nursing homes increased, from 1.3 million in 1985 to 1.5 million in 1997, because the total number of older people in the population has increased.
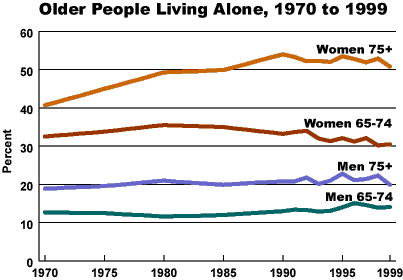
Citations
Most of the data, charts, and graphs on the older population are based on tabulations from the Census Bureau’s March Current Population Survey (CPS).
Resources
View All
La population et les changements climatiques
(Novembre 2000) En général, les négociations internationales visant à freiner les changements climatiques ont tendance à se concentrer sur les schémas de consommation dans les pays industrialisés plutôt que sur la croissance démographique mondiale. A ce jour, ce sont les pays industrialisés qui ont produit la plupart des émissions de gaz à effet de serre ; d’après le Centre d’analyse de l’information relative au gaz carbonique du département de l’Energie des États-Unis (CDIAC), en 1996, les États-Unis à eux seuls ont été responsables de 23 % du total mondial des émissions de gaz carbonique. Les niveaux astronomiques d’émissions dans un grand nombre de pays développés proviennent essentiellement des schémas de consommation qui entraînent des taux d’émission élevés par habitant (voir figure 1). Aux États-Unis, en 1996, les émissions de gaz carbonique par habitant étaient de 20 tonnes métriques, tandis qu’en Allemagne et au Japon, ces chiffres étaient respectivement de 10,5 et 9,3 tonnes métriques. Par contre, la moyenne mondiale pour cette année était de 4 tonnes métriques par habitant.
Figure 1
Emissions de gaz carbonique par habitant : Les dix pays les plus élevés, 1996
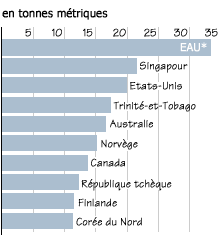
* EAU = Emirats arabes unis
Source : Département de l’Energie des États-Unis, Centre d’analyse de l’information relative au gaz carbonique, publiée dans World development indicators 2000 de la Banque mondiale.
Les pays en voie de développement contribuent rapidement et de façon appréciable aux changements climatiques. Cependant, compte tenu de la forte croissance des économies et des populations des pays en voie de développement, ces derniers connaissent également des niveaux élevés d’émission de gaz carbonique. En Chine, entre 1980 et 1996, les émissions de gaz carbonique sont passées de 1,5 à 2,8 tonnes métriques par habitant, alors que la population est passée de 984 millions à 1,22 milliards. Ainsi donc, en 1996, la Chine a été responsable de 15 % du total des émissions dans le monde, venant juste derrière les États-Unis (voir figure 2). En 1996, ensemble, les pays en voie de développement ont représenté 23 % des émissions mondiales, par rapport à moins de 17 % en 1980.
Figure 2
Emissions totales de gaz
carbonique : Les dix pays les plus élevés, 1996
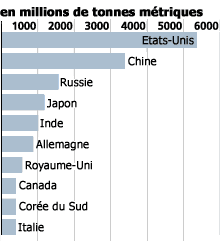
Source : Département de l’Energie des États-Unis, Centre d’analyse de l’information relative au gaz carbonique, publiée dans World development indicators 2000 de la Banque mondiale.
A longue échéance, les efforts déployés pour limiter les changements climatiques devront prendre en compte non seulement les schémas de consommation qui contribuent aux émissions élevées par habitant, mais aussi le nombre croissant de consommateurs dans le monde. Pour impliquer les pays en voie de développement dans l’élaboration de solutions, les accords futurs sur les changements climatiques seront appelés à accepter la notion que les peuples du monde ont le même droit d’accès à l’environnement pour éliminer le carbone produit par la combustion de combustibles fossiles. Si ce principe est adopté, la taille de toute la population du monde deviendrait une variable critique. En effet, plus la population augmente, moins la moyenne du niveau des émissions par habitant a tendance à être à la mesure des niveaux acceptables de production de gaz à effet de serre. En d’autres termes, au fur et à mesure que la population augmente, le droit d’un individu à polluer a tendance à diminuer.
La croissance de la population a également tendance à faire augmenter le nombre d’individus qui seront touchés par les changements climatiques, bien que l’on ne sache pas très bien jusqu’à quel point des communautés spécifiques seront affectées. Outre les hausses de températures et les changements atmosphériques, nombre d’effets moins évidents pourraient se faire sentir. La production agricole risque de s’accroître dans certaines régions, mais de diminuer fortement dans d’autres, ce qui aura tendance à aggraver la malnutrition. Le réchauffement de la planète pourrait également entraîner une redistribution des insectes, vecteurs de microbes pathogènes porteurs de maladies telles que la malaria, la fièvre rouge, la fièvre jaune et l’encéphalite risquant d’infecter les populations privées d’immunité.
Le Groupe intergouvernemental d’experts sur l’évolution du climat a identifié l’Afrique comme le continent le plus vulnérable aux impacts des changements projetés étant donné que la pauvreté endémique a tendance à paralyser la capacité d’adaptation. Mais d’autres régions seront également touchées. Les pays à forte densité de population côtière – la Chine, l’Inde et les États-Unis par exemple – seront sans doute confrontés à des dégâts d’une ampleur considérable induits par l’élévation du niveau de la mer. Dans les pays qui sont sensibles aux inondations tels que le Bangladesh, les violentes tempêtes et la modification de la configuration des pluies risquent d’exacerber les problèmes existants et de mettre en danger des communautés vivant déjà sur des terres vulnérables. En fin de compte, bien que nous ne sachions pas quel sera l’impact exact des changements climatiques, il est presque certain que ceux-ci auront des répercussions inattendues à l’échelle planétaire.
Bingham Kennedy, Jr., est rédacteur adjoint au PRB.
Ressources
Voir tout
The Baltics: Demographic Challenges and Independence
(November 2000) Latvia, Estonia, and Lithuania are in the midst of a transition to independence after nearly 50 years of domination by the Soviet Union. Some of the first laws passed by the newly independent governments placed strict limits on who could become a citizen and actively promoted use of the native languages. Latvia’s laws were probably most severe — only Latvians whose families were citizens before 1940 automatically gained citizenship to independent Latvia — all others had to meet stringent qualifications — including fluency in the Latvian language and 16 years of residency. The laws left many former Soviet citizens, many of whom were long-term residents, without citizenship in any country. International critics, most vocally from Russia, claimed these laws infringed on the civil rights of the large ethnic minorities within these countries.
Reforms in 1998 extended citizenship options for non-Latvians, but a new language law taking effect in September 2000 has renewed tensions over ethnic relations. The new law requires that government officials demonstrate a fluency in Latvian a problem in many large cities where Russian is still the predominate language. Schools are required to phase in Latvian language instruction and some long-time teachers are being challenged to learn Latvian.
Some citizenship requirements have been modified in Estonia as well, but Baltic nationalists remain firm in their desire to assert their ethnic identities. Their actions can be better understood within the context of their political histories and current demographic realities. After World War II, tens of thousands of Soviet troops and Russian colonists were brought to the region to solidify Soviet domination. Russian was the official language in the Baltics and was taught in the schools. Relatively few of the foreigners learned the Baltic languages.
The end of Soviet rule in 1991 left thousands of Russians, along with smaller numbers of Ukrainians, Poles, Belorussians, and other foreigners, living in newly independent countries. Many Russians colonists and military personnel left the region in the early 1990s, but most remained. In the late 1990s, ethnic Russians still made up at least one-third of both Estonia and Latvia, and about 9 percent of Lithuania. Ukrainians, Poles, and other foreigners made up another 5 percent to 10 percent of these countries’ populations.
Independence also ushered in extremely low fertility rates and rising mortality rates, which-combined with the initial exodus of tens of thousands of immigrants-caused the population to decline during the 1990s. With the low birth rates and slower outflow of foreigners, these populations will continue to include large ethnic minorities, and language and citizenship are likely to remain hot political issues.
Taken together, the three Baltic states have 7.5 million inhabitants within an area of 67,600 square miles. The region consists of relatively flat and low-lying moist land that has few natural resources, but its strategic location on the Baltic Sea provides a valuable outlet to the sea. Access to seaports prompted imperial Russia and later the Soviet Union to invade and rule the area.
The Baltic countries achieved statehood only in the 1920s, after the Russian revolution and World War I. But their new independence was shattered by World War II when the Baltic region became part of the Soviet Union as part of a secret pact between Nazi Germany and the USSR. Their incorporation into the USSR was never recognized by the United States, and each country maintained diplomatic legations in Washington that served as ready-made embassies after independence. Lithuania was the first of the former Soviet republics to declare independence, on March 11, 1990. Estonia and Latvia followed suit the following year.
Estonia: Forging Closer Ties to the European Community
Estonia is the smallest of the Baltic countries both in land area and population. But it is the wealthiest of the three and is likely to become the first to be admitted to the European Union. It still imports most of its energy fuels from Russia and other former Soviet republics, but trade with Finland and other European countries has replaced lost trade with Russia. As the country forges closer economic ties to the rest of Europe, pressure to improve the civil rights of non-Estonians has increased.
Estonia has about 1.4 million inhabitants. The country is basically flat, dotted with lakes and peat bogs. The northern shore, called the Glint, is cut by limestone escarpments that allow for good harbors, including the harbor at Tallinn, the capital.
The Estonian language, which belongs to the Balto-Finnic group of the Finnic-Ugric languages and uses Latin characters, was made the official language in 1989. The teaching and use of Estonian are promoted throughout society, yet ethnic Estonians make up less than two-thirds of the population. About 30 percent of the population is Russian; Ukrainians and Belorussians make up another 5 percent.
Estonia’s population was just over 1 million in 1950 and reached 1.6 million in 1990. The birth rate had been constant at about 16 births per 1,000 population for many years; the total fertility rate (TFR) — or average number of children born per woman — was about 2.2 children per woman, just above the level needed to maintain a stable population size. By 1998, the birth rate had fallen just below 9 while the death rate was 13 per 1,000 population, which meant that more people died than were born each year. The TFR was among the world’s lowest, at 1.2 children per woman. Emigration, primarily of Russians, caused a net population loss of about 90,000 between 1989 and 1994, but the outflow slowed in the later 1990s. By 2000, the population had fallen to an estimated 1.4 million persons and was declining by about 8,000 per year.
Post-independence Estonians are waiting longer to marry but not necessarily waiting longer to have children. The average age at first marriage for Estonian women rose from 22.5 in 1990 to 24.3 in 1998. The average age when women have their first child rose more slowly: from 22.9 to 23.6. The proportion of babies born to unmarried women shot up from 27 percent in 1990 to 52 percent in 1998. Access to contraception was limited, especially in the economic and social disruptions of the 1990s. Abortion is prevalent. There were an estimated 152 abortions for every 100 births in 1997.
Life expectancy suffered after independence, but began to recover in the later 1990s. Life expectancy at birth for Estonian males dropped from 66.6 years in 1988 to 61.1 years in 1994, while it slipped from 75.0 to 73.1 for females. Health conditions have improved as the country transitions to a free-market economy, but life expectancy at birth still has not returned to the pre-independence levels for men, and is only slightly higher for females. In 1998, life expectancy was 64.4 years for males and 75.5 years for females-well below the averages for other northern European countries.
With its low birth rate and large foreign community, the ethnic Estonian population is not likely to increase its share of the country’s population, and the country’s residents are slowly accepting their new reality as a multicultural society. In a recent survey reported by the Baltic News Service, a large majority of ethnic Estonians said they believed that different nationalities could get along and work together, and about three-fourths said that different languages and cultures enrich the society. The same survey found that a large majority of non-Estonian residents said they considered Estonia their home and felt loyal to the government. These attitudes are a marked change from a 1993 survey in which only 29 percent of Russian-speakers said they were treated fairly in the country.
Latvia: A Struggle for Identity
Latvia is the middle Baltic country, with Estonia to the north and Lithuania to the south. Latvia’s strong brand of nationalism may reflect the fact that ethnic Latvians are a slim majority of the population and a minority in many of the country’s largest cities. The Latvian language, using Latin letters, belongs to the Baltic group of Indo-European tongues. It has only one other modern counterpart, Lithuanian.
Latvia has been ruled by outsiders throughout most of its history. Prior to the USSR’s breakup, Latvia was independent only during the interwar period, 1918 to 1940. In June 1993, Latvia finally held its own elections, replacing the legislature from the Soviet era and electing a president. In 1995, the Council of Europe granted Latvia membership, over Russian objections. Latvia is now applying for acceptance to the European Union, which would bring a number of economic benefits.
Latvia’s stringent citizenship law has been a stumbling block to its acceptance by European countries. Even after some requirements were relaxed, relatively few non-Latvians sought or gained citizenship, and many resented their treatment by Latvians. By June 1997, less than three-fourths of the country’s population were citizens, but less than 5 percent of the eligible population of non-Latvians had applied for citizenship.
Latvians have been divided about the treatment of non-Latvians-many fear international isolation and condemnation if they do not improve ethnic relations within the country. Others insist on reinforcing a strong national identity.
Latvia’s population was 2.67 million in January 1991, when it gained independence. It slipped to 2.44 million in January 1999, as the number of Slavic emigrants increased and the birth rate went into a freefall. From 1990 to 1992, about 90,000 emigrants left the country. It is the falling birth rate and rising death rate, however, that reversed Latvia’s demographic trends.
In 1990, there were 14 births per 1,000 population and women had 2.0 children, on average. Between 1990 and 1998, however, the annual number of births were cut in half, and the fertility rate fell to 1.1 children per woman. The annual number of deaths rose sharply until 1994, then fell back to the 1990 level. In 1999, there were about five deaths for every three births in Latvia.
The fertility decline reflected delays in marriage-the average age at first marriage for women rose from 22.2 in 1990 to 24.0 in 1998. But couples waited even longer to have children or chose not to have them at all. The share of births to unmarried women rose, but not as rapidly or as high as in Estonia. In 1990, about 17 percent of births were out of wedlock; by 1998, about 37 percent were out of wedlock. Abortion is also prevalent. In 1998, there were 108 abortions for every 100 births in Latvia.
Life expectancy for males fell sharply from 64.2 in 1990 to 60.7 in 1994; female life expectancy fell more slowly during the period, from 74.6 to 72.9 years. As conditions improved in the second half of the decade, life expectancy rose back to pre-independence levels. In 1998, life expectancy was 64.1 years for males and 75.5 years for females.
Lithuania: Ethnically Homogeneous
Lithuania is the largest Baltic state in population and territory. It includes 3.7 million people in a little more than 25,000 square miles. The country physically separates mainland Russia from the Russian oblast Kaliningrad, on the Baltic coast. Lithuania was once one of the strongest military powers in Europe. In the 14th century, the domain of the Grand Duchy of Lithuania stretched across Europe as far as Ukraine. But the end of the 16th century, Lithuania was reduced to the comparatively small size it is today.
Lithuania is by far the most ethnically homogeneous of the Baltic countries. In 1998, the population was 82 percent Lithuanian, 8 percent Russian, and 6 percent Polish.
Lithuania’s birth rate dropped from 15 births per 1,000 to 10 per 1,000 between 1990 and 1999, while its death rate remained just under 11. The TFR fell from 2.0 births per woman in 1989 to 1.3 in 1999. Women marry at a relatively young age, compared with the other Baltic states, and the age is declining-in contrast to elsewhere in Europe. In 1998, the average age at marriage for women was 22.9 years, and the average age at first birth was 26.3. Abortion is less prevalent here than in Estonia or Latvia, but is still relatively common. In 1997, there were 60 abortions for every 100 births.
Life expectancy at birth for males reached a high of 67.9 years in 1986–1987, but fell to 64.8 by 1994. It increased to 65.9 years in 1997, still below the highs of the mid-1980s. For females, the slide was far less over this period. Life expectancy at birth for females fell from 76.6 to 74.9, and then rose back to 76.8 in 1997.
Unlike the other Baltic countries, relations with the small Russian minority are quite good. All residents are permitted to attain citizenship, regardless of their ethnic origin, a policy that facilitated Lithuania’s entry into the Council of Europe. Lithuania is working toward membership in the European Union, which may further weaken its ties to the former Soviet republics.
Mary Kent is the editor of Population Bulletin at the Population Reference Bureau.
For More Information
The Baltic Nations: Demographic Challenges in the Transition to Independence
Baltic News Service, “Most Non-Ethnic Estonians See Themselves as Loyal to Estonia – Survey,” Oct. 10, 2000. Accessed online on Oct. 26, 2000.
Council of Europe, Recent Demographic Developments in Europe 1999 (Belgium: Council of Europe, 1999).
Eastern Europe and the Commonwealth of Independent States 1999 (London: Europa Publications, 1998).
Europe Information Service, European Report, “Minorities Issues Trouble EU-Latvia Joint Parliamentary Committee,” Oct. 11, 2000. Accessed online on Oct. 26, 2000.
Carl Haub, “Population Change in the Former Soviet Republics,” Population Bulletin 49, no. 4 (Washington, DC: Population Reference Bureau, 1994).
Alain Monnier, “La conjoncture démographique: l’Europe et les pays développés d’outre-mer,” Population 54, no. 4-5 (juillet-octobre 1999).






