When the Grocery Store Closed, a Town Lost More Than Food

The closure of a local grocery store or clinic is often framed as an economic loss or a mere inconvenience. But a new case study raises questions about whether the consequences, especially for small towns, may be broader—affecting residents’ lives well beyond access to goods and services.
Danielle Rhubart and colleagues at Pennsylvania State University examined how the loss of “vital places”—everyday locations such as grocery stores, pharmacies, primary care clinics, schools, and churches—may affect health through social and environmental pathways. Focusing on a rural township in Pennsylvania, they argue that such places function as health infrastructure, particularly in rural areas with limited alternatives.
On paper, the township’s income and poverty levels did not signal severe economic distress, the researchers noted. While some local jobs had disappeared, many residents commuted about 30 miles to a nearby university town, likely cushioning the economic effects of business closures. Yet the physical landscape reflected gradual decline: the population had dropped over the past three decades, and many community institutions had closed.
Using in-depth interviews with 26 long-term residents over eight months in 2022, Rhubart and team situated these losses within a social determinants of health framework, which links health outcomes to factors such as economic stability, transportation, social connection, and the built environment (figure). Their findings suggest that when essential community institutions disappear, the effects can ripple through daily life, increasing isolation, financial strain, and barriers to healthy behavior.
Figure. Rural Disinvestment Could Undermine Health Through Interconnected Pathways
A conceptual framework for how the loss of rural vital places affects economic stability, education, and other social determinants of health
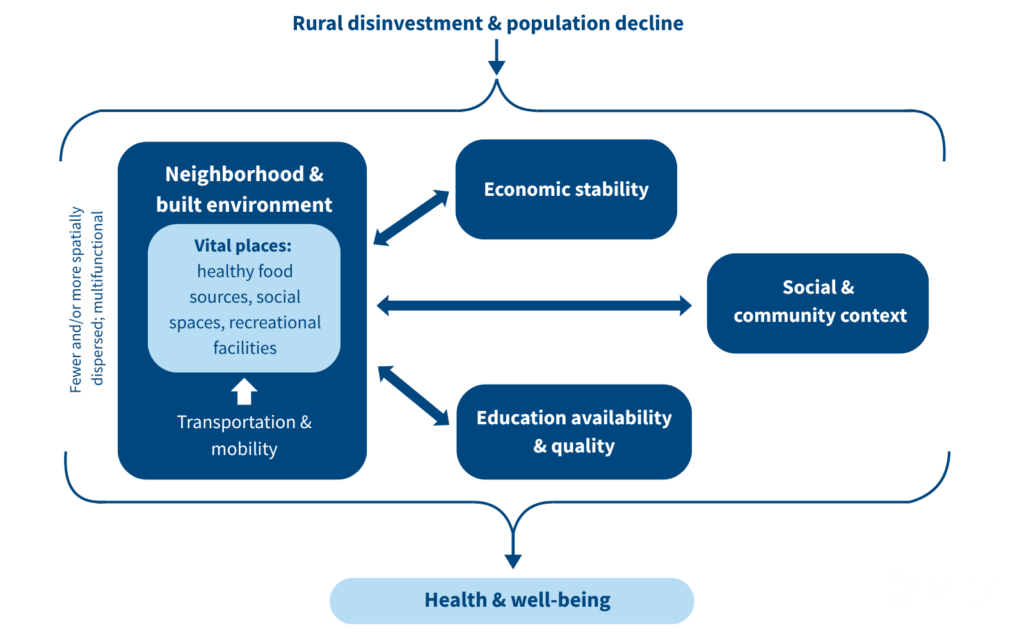
Source: Danielle Rhubart et al., “The Loss of Rural Vital Places: A Case Study Using the Social Determinants of Health Framework,” Wellbeing, Space and Society 7 (2024): 100228.
The study addresses what the authors describe as a relative lack of attention to rural contexts in research on vital places, and extends the social determinants of health framework to a small-town setting. In rural settings, the authors note, even a single closure “can ripple through the community, creating a desert for nutritious foods, physical activity, or social connection.”
Scrambling for Fresh Food
In the Pennsylvania community, the most immediate impact residents described was the loss of basic services. When the town’s only grocery store closed, many had to travel long distances for food. For older adults and those without reliable transportation, access became more difficult. One resident noted, “A dozen people that I know personally don’t have a way to the grocery store.”
A dollar store eventually opened, but residents said it offered limited fresh food. People noticed the impact on diets. “Obesity [is] the biggest problem, and because of the lack of places to get good food, they’re relying on snack foods and quick and easy foods,” another resident said.
The grocery store had also served as a gathering place, and its closure disrupted daily routines and casual social contact, people reported.
Staying Active Became a Challenge
Coupled with the loss of the town’s grocery store, a lack of accessible places to exercise further constrained the community’s ability to support health year-round.
Township residents described abundant outdoor recreation—hiking, fishing, kayaking and hunting—and praised the area’s natural beauty. But these activities were largely seasonal, and indoor exercise facilities were absent. A local trail system intended for walking and running had become dominated by four-wheelers, limiting safe use.
Several residents linked the lack of year-round recreational spaces to health concerns, including obesity. “These people don’t have anywhere to go. There’s no YMCA, Planet Fitness, no exercise establishments, so they sit and watch TV, and they sit on their porch. They don’t do anything,” one said.
Social Interaction Declined as Gathering Spots Vanished
As vital spaces disappear, more than convenience was lost, people emphasized. Like the grocery store, other local businesses, churches, and restaurants had functioned as informal meeting spaces—and their closure reduced opportunities for routine interaction. “There’s no place where you just run into people and talk,” one resident explained.
The authors note that fewer gathering spaces can erode social ties, which are recognized within the social determinants of health framework as important to overall well-being. In sparsely populated areas with few alternatives, the loss of even one gathering space can weaken these ties and reshape patterns of interaction.
Getting Anywhere Cost More Time and Money Than It Used To
Residents also described economic impacts, including job losses tied to business closures and higher travel costs as they ventured elsewhere to get what they needed. As one person put it, “There used to be quite a few businesses that supported the community, but most of them are gone or really pared down.” Spending shifted to neighboring towns as residents sought alternatives.
Limited transportation options compounded these effects. With sparse public transit and long distances between services, access to food, health care, and employment became more time-consuming and costly.
The Local School Held the Community Together—but Enrollment Was Shrinking
The township’s elementary school served as a central institution and source of community identity. Residents described it as a hub where families knew one another and valued its small size, close teacher-to-student ratios, and strong interpersonal connections. Having a local school also meant children did not have to travel long distances, reinforcing daily community ties and freeing up schedules.
But population loss and broader institutional challenges have reduced enrollment in recent years, shrinking class sizes and raising concerns about the school’s long-term viability. A former teacher notes, “It’s hard to see the declining enrollment at school. When I was still teaching, which was 10 years ago, there were two classes of every grade: two first, two second, K through fifth. And now there is one of each.” For many, the school represents more than education—it is a key site of social cohesion and local pride, whose future feels increasingly uncertain.
Neighbors Helped Fill the Gaps, Hauling Groceries and Running Errands
As vital places closed, residents described stepping in to support one another—especially older adults with limited mobility. Neighbors picked up groceries, delivered food pantry items, and used trips out of town to run errands for others. Many expressed pride in the community’s willingness to help. “I have to be off the mountain. Who needs what while I’m there? [I’d get] a grocery list of things for different people.”
Social media, particularly a local Facebook group, became an important tool for coordinating assistance and sharing community news, including information about road conditions, power outages, and neighbors’ needs. Still, limited internet access meant not all residents could benefit equally from these digital connections.
Community Institutions as Health Infrastructure
In rural settings, vital places often serve multiple functions simultaneously—economic, social, and practical. Their loss, therefore, can affect several dimensions of daily life at once.
This study suggests that policies aimed at improving rural health should consider the preservation and support of multifunctional community institutions, as well as investments in transportation and infrastructure. The findings underscore the broader public health principle that health is shaped not only by medical care and genetics, but by the environments in which people live.
Reference
- Danielle Rhubart et al., “The Loss of Rural Vital Places: A Case Study Using the Social Determinants of Health Framework,” Wellbeing, Space and Society 7 (2024): 100228.



